犬・猫の呼吸器臨床研究会
短頭種気道症候群(BAS)研究班の報告(2020.12.31更新 計136)
2021年8月1日より犬・猫の呼吸器臨床研究会 VeRMS Study Groupのホームページは独立いたしました。本ページは、2021年7月31日までの情報となります。それ以降の情報は、www.verms.or.jp で更新しております。
短頭種気道症候群一般、非短頭種の咽頭閉塞、重度上気道閉塞疾患に対する気管切開、犬の睡眠時無呼吸症候群の文献レビュー
テーマは、「BASの術前評価に応じた術式選択」「咽頭気道閉塞症候群89例」「気管切開下軟口蓋拡大切除術の外科成績」、「睡眠時無呼吸症候群の定義と定量」、「一時的気管切開200例-適応、周術期安全性、救命率の向上」、「永久気管切開術70例-適応、新術式による術後合併症の減少と長期QOLの安定」、「Tチューブによる重度喉頭気管閉塞疾患の管理」
短頭種気道症候群 BAS、一般
2020
Seneviratne M, Kaye BM, Ter Haar G. Prognostic indicators of short-term outcome in dogs undergoing surgery for brachycephalic obstructive airway syndrome. Vet Rec 2020;187:403.
短頭種閉塞性気道症候群に対する手術を受けた犬の短期転帰の予後因子
BACKGROUND: The aims of this study were to assess the impact of epidemiological variables, severity of presurgical respiratory signs, diagnostic findings from pharyngeal and laryngeal examination using a new grading scheme and CT scan images, on postsurgical outcome in dogs undergoing surgery for brachycephalic obstruction airway syndrome (BOAS). METHODS: An owner-based questionnaire was used to grade dogs based on their respiratory signs before surgery and at least six weeks after surgery. Epidemiological data and results from presurgical pharyngeal and laryngeal examination and CT scan findings for 75 dogs undergoing airway surgery were collected from the medical records. RESULTS: 70.7 per cent of dogs showed an improvement in respiratory signs following rhinoplasty and palatoplasty. This improvement was associated with the severity of inspiratory efforts and the Poncet score on presentation, but not with any other clinical sign or anatomical abnormality found during BOAS assessment, nor by the degree of craniofacial shortening as determined by CT-scan. Presurgical snoring was positively associated with the degree of narrowing of pharyngeal dimensions. CONCLUSIONS: Dogs presenting with clinical signs of BOAS benefit from rhinoplasty and palatoplasty alone. The degree of narrowing of pharyngeal dimensions appears to be associated with severity of snoring while soft palate length alone was not.
コメント:BAOSに対して軟口蓋切除術と鼻孔形成術を実施した犬の術後転帰について、予後因子を検討した回顧的研究。術前の吸気努力のグレードが高くなるほど、術後の改善がみられた。鼻孔、咽頭、喉頭に対して、新しいグレーディングシステムを提案しているが、術後転帰と関連はみられなかった(いいのペットクリニック 飯野亮太-2020.12.29)。
Franklin PH, Liu NC, Ladlow JF. Nebulization of epinephrine to reduce the severity of brachycephalic obstructive airway syndrome in dogs. Vet Surg 2020. doi. 10.1111/vsu.13523
犬におけるBAS重症度軽減を目的としたエピネフリン吸入療法
OBJECTIVE: To determine the preoperative and postoperative effect of nebulized epinephrine on brachycephalic obstructive airway syndrome (BOAS) severity in dogs. STUDY DESIGN: Prospective clinical study. SAMPLE POPULATION: Thirty-one client-owned pugs, French bulldogs, and English bulldogs with moderate to severe BOAS. METHODS: Whole body barometric plethysmography was used to determine BOAS severity (BOAS index; 0%-100%) prior to and after nebulization with 0.05 mg/kg epinephrine diluted in 0.9% saline preoperatively. The same protocol was repeated postoperatively (within 24 hours of surgery). RESULTS: Five dogs were excluded because they did not tolerate nebulization, and postoperative data were available for 13 dogs. Epinephrine nebulization resulted in a decreased BOAS index across all breeds of dog both before (9.6% [3.1% to -30.2%], n = 26) and after surgery (14.3% [0.9% to -24.3%], n = 13). The preoperative reduction in BOAS index was greater (17.3% [1.8% to -27.4%]) in dogs with a baseline BOAS index >70% (P = .006) and in pugs (16.9% [0.8% to -27.4%]) compared with French bulldogs (5.2% [3.1% to -30.2%], P = .03). Simple linear regression was used to identify a positive relationship between baseline BOAS index and reduction in BOAS index for pugs (n = 10, P = .001). Nausea was noted as a side effect in four dogs. CONCLUSION: Nebulized epinephrine reduced the BOAS index of dogs in this study. This effect was clinically significant in preoperative dogs with a BOAS index >70% and in dogs recovering from surgery. CLINICAL SIGNIFICANCE: This study provides evidence to support the use of nebulized epinephrine in the perioperative management of BOAS-affected dogs.
コメント:中等度~重度のBAS犬31頭(パグ、フレンチブルドッグ、イングリッシュブルドッグ)を用いた前向き研究。術前のエピネフリン吸入療法は、特に重度のBAS犬において、有意に呼吸機能を改善させた。(大樹どうぶつ病院 福田大介2020.10.18)
Lindsay B, Cook D, Wetzel JM, et al. Brachycephalic airway syndrome: management of post-operative respiratory complications in 248 dogs. Aust Vet J 2020;98:173-180.
BAS症例248頭に対する整復手術術後合併症の管理
OBJECTIVE: As ownership of brachycephalic dog breeds rises, the surgical correction of components of brachycephalic airway syndrome (BAS) is increasingly recommended by veterinarians. This study’s objective was to describe the incidence of, and strategies for the management of post-operative respiratory complications in brachycephalic dogs undergoing surgical correction of one or more components of BAS. METHODS: Medical records of 248 brachycephalic dogs treated surgically for BAS were retrospectively reviewed for demographic information, procedures performed, post-operative complications and treatment implemented, hospitalisation time, and necessity for further surgery. RESULTS: Pugs, Cavalier King Charles Spaniels and British Bulldogs were the most commonly encountered breeds. Dogs which experienced a complication were significantly older (mean was 5.5 years, compared with 4.1 years [P < 0.01]). Fifty-eight dogs (23.4%) had complications which included: dyspnoea managed with supplemental oxygen alone (7.3%, n = 18), dyspnoea requiring anaesthesia and re-intubation (8.9%, n = 22), dyspnoea necessitating treatment with a temporary tracheostomy (8.9%, n = 22), aspiration pneumonia (4%, n = 10), and respiratory or cardiac arrest (2.4%, n = 6). Five of the 22 dogs requiring anaesthesia and re-intubation deteriorated 12 or more hours after post-surgical anaesthetic recovery. The overall mortality rate in this study was 2.4% (n = 6). Age, concurrent airway pathology, and emergency presentation significantly predicted post-operative complications. CONCLUSION: Our data show the importance of close monitoring for a minimum of 24 h following surgery by an experienced veterinarian or veterinary technician. Surgical intervention for BAS symptomatic dogs should be considered at an earlier age as an elective procedure, to reduce the risk of post-operative complications.
コメント:オーストラリアにおける報告。BASに対する外科手術において、中齢以降での実施は、術後合併症の発生率の上昇と有意に相関すると報告している(大樹どうぶつ病院-福田大介2020.6.23)。
Yoon H, Yu J, An G, et al. CT and radiographic evaluation of bronchial collapsibility at forced expiration in asymptomatic brachycephalic dogs. Vet Radiol Ultrasound 2020;61:167-180.
CTおよびX線を用いた、上気道症状を伴わない短頭種における強制呼気時の気管支虚脱性の評価
Bronchial collapse due to bronchomalacia is an important cause of chronic coughing in dogs. Radiographic and CT evidence of bronchial collapse has previously been reported in healthy Beagle dogs under forced expiration. However, published studies in brachycephalic dog breeds that are prone to bronchial collapse are currently lacking. In the present prospective analytical experimental study, CT and radiography were used to measure the bronchial diameter and collapsibility of each pulmonary bronchus during end-expiratory, 5 mL/kg forced-expiratory, and 10 mL/kg forced-expiratory phases in 17 asymptomatic brachycephalic dogs and six healthy Beagle dogs. Bronchial collapsibility was significantly greater during forced expiration, than that at the end of expiration in both groups (P < .001). Bronchial collapsibility measurements of the left lung lobes and the right cranial, middle, and accessory lobes were significantly higher in asymptomatic brachycephalic dogs than those in healthy Beagle dogs, during all expiratory phases (P < .05). The higher bronchial collapsibility of brachycephalic dogs was also supported using CT multiplanar reconstruction images and radiography. In conclusion, radiographic and CT measures of bronchial collapsibility in asymptomatic brachycephalic dogs are higher than measures in healthy Beagle dogs. Therefore, measures of bronchial collapse in brachycephalic dogs should not be evaluated using the same baseline measures as those used for healthy Beagle dogs.
コメント:無症候性の短頭種と健康なビーグルについて、CTおよびX線を用い呼気時気管支虚脱の程度を比較した論文。無症候性であっても、短頭種では、呼気時の気管支虚脱がビーグルに比べ有意に認められた。著者らは、短頭種の呼気時気管支径を評価する際、健康なビーグルで得られたデータと単純に比較することはすべきでないと結論づけている(大樹どうぶつ病院 福田大介-2020.6.23)。
Fenner JVH, Quinn RJ, Demetriou JL. Postoperative regurgitation in dogs after upper airway surgery to treat brachycephalic obstructive airway syndrome: 258 cases (2013-2017). Vet Surg 2020;49:53-60.
短頭種閉塞性気道症候群の犬における上気道外科手術後の吐き戻し:258例(2013-2017)
OBJECTIVE: To determine the incidence of and risk factors for regurgitation in dogs within 24 hours of surgical management of brachycephalic obstructive airway syndrome (BOAS). STUDY DESIGN: Retrospective single center study of dogs undergoing BOAS surgery over four years (2013-2017). ANIMALS: Two hundred fifty-eight client-owned dogs referred for surgical intervention for BOAS. METHODS: Electronic medical records were searched for dogs that had undergone surgery for BOAS at a UK specialist referral hospital. Data were assessed by using univariable binomial logistic regression; confounding factors were then identified in a multivariable model. RESULTS: There was an increase in the proportion of dogs that regurgitated while hospitalized preoperatively vs during the first 24 hours postoperatively, from 28 (10.9%) to 89 (34.5%), respectively (P < .0001). History of regurgitation (P = .017, odds ratio [OR] 2.539, 95% confidence interval [CI] 1.178-5.469) and age (P = .008, OR 0.712, 95% CI 0.553-0.916) were detected as risk factors for postoperative regurgitation. For every 1-year increase in age, the odds of experiencing postoperative regurgitation were reduced by 28.8%. CONCLUSION: Corrective surgery for BOAS was associated with a marked incidence of postoperative regurgitation. Younger dogs and those with a history of regurgitation were predisposed to postoperative regurgitation. CLINICAL SIGNIFICANCE: The increased frequency of regurgitation after surgical treatment of BOAS, especially in younger dogs, provides justification for counseling owners regarding this postoperative complication.
コメント:BOASの整復術後に吐き戻しの頻度は増加し、より若い犬と吐き戻し歴のある犬では、特に起こりやすい。若い犬で増加する理由として、未熟な食道括約筋、重度な呼吸器症状が推察されているが、回顧的研究のため不明。犬種や喉頭虚脱のステージとは関連がなかった(いいのペットクリニック 飯野亮太-2020.6.22 )。
2019
Riggs J, Liu NC, Sutton DR, et al. Validation of exercise testing and laryngeal auscultation for grading brachycephalic obstructive airway syndrome in pugs, French bulldogs, and English bulldogs by using whole-body barometric plethysmography. Vet Surg 2019;48:488-496. PDFあり
全身圧プレスチモグラフィを用いた運動負荷試験および喉頭聴診によるBAOSの重症度判定の妥当性評価
OBJECTIVE: To determine whether the sensitivity of clinical examination for assessing upper airway disease severity in 3 breeds of brachycephalic dogs can be improved by incorporating an exercise test (ET) or by auscultation of a laryngeal stridor to predict laryngeal collapse. STUDY DESIGN: Prospective clinical study. ANIMALS: Client-owned brachycephalic dogs (n = 44 ET; n = 57 laryngeal stridor assessment). METHODS: In the first part of the study, clinical examinations were performed at rest and after 5-minute walk and 3-minute trot tests, and a grade reflective of brachycephalic obstructive airway syndrome (BOAS) severity was assigned. Whole-body barometric plethysmography was used as a comparative, objective measure of disease severity. In the second part of the study, the degree of laryngeal collapse present in dogs undergoing BOAS surgery was compared to pre-exercise and postexercise laryngeal stridor detected during functional testing. RESULTS: The sensitivity of clinical examination for BOAS diagnosis was 56.7% pre-ET, 70% after a 5-minute walk test, and 93.3% after a 3-minute trot test. The sensitivity of laryngeal stridor as a predictor of laryngeal collapse was improved after exercise (70%) compared with before exercise (60%). Specificity of laryngeal stridor for laryngeal collapse was 100% (pre-exercise and postexercise). CONCLUSION: The sensitivity of clinical examination for BOAS diagnosis was improved by inclusion of an ET, particularly the 3-minute trot test. Audible laryngeal stridor was highly specific but only moderately sensitive for laryngeal collapse. CLINICAL SIGNIFICANCE: Inclusion of a 3-minute trot test and careful auscultation for laryngeal stridor are recommended during BOAS assessment of brachycephalic dogs.
コメント1:BOASリスク犬種において、運動負荷試験および喉頭の聴診によってPhysical examinationによる上部気道閉塞の重症度判定および喉頭虚脱の有無の検出力の感度および特異度の上昇がみられた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
コメント2:パグ、フレンチブルドッグ、イングリッシュブルドッグを用いた2種類の前向き研究。第一の研究:BASの重症度判定を行う際の運動負荷試験の有効性を、全身気圧プレチスモグラフィを用い評価した(n=44)。診断感度は運動負荷試験により上昇した(3分間の速歩をメニューに含めるとよい)。第二の研究:運動前後における喉頭ストライダーの有無を評価し、その後手術によって喉頭虚脱の有無を確認した(n=57)。運動負荷により、こちらも診断感度が上昇した。喉頭ストライダーの存在は、喉頭虚脱の診断において特異性が極めて高かった。(まるふく動物病院 福田大介-2019.5.6)
コメント3:BAOSの臨床診断評価において、3分間小走り運動負荷試験により感度を上げることができる。また、喉頭ストライダーをもっているすべての犬は喉頭虚脱をもっているが、ストライダーがなくても喉頭虚脱を除外することはできない(いいのペットクリニック 飯野亮太-2020.5.5)。
Kirsch MS, Spector D, Kalafut SR, et al. Comparison of carbon dioxide laser versus bipolar vessel device for staphylectomy for the treatment of brachycephalic obstructive airway syndrome. Can Vet J 2019;60:160-166.
BAS犬の軟口蓋過長整復術におけるCO2ガスレーザーとバイポーラ電気メスの比較
Carbon dioxide (CO2) laser and bipolar vessel sealing device (BSD) are industry standards for soft palate resection. No studies exist to directly compare these 2 techniques in a clinical setting. The purpose of this study was to describe and compare clinical outcomes for dogs that underwent CO2 laser versus BSD staphylectomy. Medical records of brachycephalic dogs that underwent CO2 laser (Group-L) or BSD staphylectomies (Group-B) between September 2013 and September 2017 were reviewed retrospectively. Of 60 dogs that met the inclusion criteria, 26 dogs (43%) were designated Group-L and 34 (57%) Group-B. Techniques did not differ in procedure or anesthetic time (P = 0.52 and P = 0.19, respectively) or major complication rates [intraoperative (P = 1.00), post-operative (P = 0.72), short-term (P = 1.00), and long-term (P = 0.68)]. This study suggests that patient outcomes are similar for dogs undergoing staphylectomy performed by CO2 laser and BSD.
コメント:BAS犬に対する軟口蓋過長整復術60件の臨床転帰を、使用した電気デバイス(CO2ガスレーザー:26件 vs. バイポーラ電気メス:34件)で比較した研究。手術時間や麻酔時間、主要な合併症発生率に有意差は認められなかった。(まるふく動物病院 福田大介-2019.5.6)
Kim YJ, Lee N, Yu J, et al. Three-dimensional volumetric magnetic resonance imaging (MRI) analysis of the soft palate and nasopharynx in brachycephalic and non-brachycephalic dog breeds. J Vet Med Sci 2019;81:113-119.
短頭種と非短頭種における3D-MRIを用いた軟口蓋と鼻咽頭の評価
The purpose of this study was to use magnetic resonance imaging (MRI) to compare the volumes and three-dimensional configurations of the soft palate and nasopharynx in non-brachycephalic and brachycephalic dogs with different body weights, and infer which factors influence nasopharyngeal volume. This was a retrospective observational study. The brain MRI medical records of all dogs referred to the Veterinary Medical Center, Chungbuk National University, between 2013 and 2016, for evaluation of intracranial disease were reviewed. There was a significant difference in the two-dimensional parameters including soft palate length/skull length ratio (P<0.01) and maximum soft palate thickness (P<0.01), and three-dimensional parameters which included soft palate volume (P<0.01), nasopharyngeal volume (P<0.01), soft palate/total upper airway volume ratio (P<0.01), and nasopharyngeal volume/total upper airway volume ratio (P<0.01), between brachycephalic and non-brachycephalic dog breeds. Nasopharyngeal volume correlated positively with the maximum soft palate thickness and body weight in all breeds. The three-dimensional morphologic grades of soft palate were significantly different between the two groups. In brachycephalic breeds, Grade 3 was observed in 33% of cases but was absent in non-brachycephalic breeds, where Grade 1 was present in 85% of the cases. We can conclude that three-dimensional morphology and upper airway volume are significantly different between brachycephalic and non-brachycephalic breeds, and body weight and maximum soft palate thickness are the key factors associated with a decreased nasopharyngeal volume.
コメント1:MRIを用いて短頭種および非短頭種の軟口蓋および鼻咽頭を比較した論文。平面的な比較でも種々のパラメータが有意に異なっていたが、鼻咽頭容積は軟口蓋の最大厚および体重と正に相関していた(ダクタリ動物病院東京医療センター 田畑達彦-2019.5.1)。
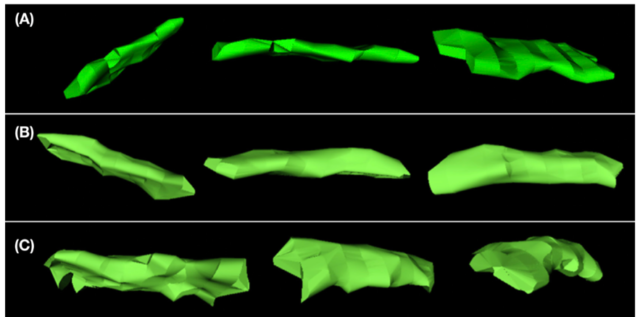
コメント2:MRI検査を受けた犬127頭(短頭種42、非短頭種85)における後ろ向き研究。3D-MRIにより各種パラメーターを測定し、その結果をもとに鼻咽頭容積に影響する因子を推測した。短頭種は非短頭種に比べ、軟口蓋の3D形態グレード(下図参照)が有意に高く、鼻咽頭容積は有意に小さかった。また、体重や軟口蓋の厚みと、鼻咽頭容積には負の相関がみられたため、これらはBASの病態に関して重要な因子であると結論付けられる。(まるふく動物病院 福田大介- 2019.5.6)。
Liu NC, Genain MA, Kalmar L, et al. Objective effectiveness of and indications for laser-assisted turbinectomy in brachycephalic obstructive airway syndrome. Vet Surg 2019;48:79-87.
BAOSに対するレーザー焼灼補助下鼻甲介切除術の効果の客観的評価および客観的適応基準
OBJECTIVE: To evaluate the effectiveness of laser-assisted turbinectomy (LATE) in treating brachycephalic obstructive airway syndrome (BOAS) and to investigate the potential indications. STUDY DESIGN: Prospective clinical study. SAMPLE POPULATION: Client-owned pugs, French bulldogs, and English bulldogs (n = 57). METHODS: A BOAS index was obtained from whole-body barometric plethysmography before BOAS conventional multilevel surgery (CMS) and 2-6 months post-CMS. Dogs with BOAS index >50% and BOAS functional grades II-III after CMS were considered candidates for LATE. A BOAS index was repeated 2-6 months after LATE. Intranasal lesions and a measurement of soft tissue proportion at the rostral entrance of choanae (STC) were recorded on the basis of computed tomography images. Logistic regressions were used to assess the intranasal predictors for being LATE candidates. RESULTS: Twenty-nine of 57 dogs were candidates for LATE, all of which were pugs or French bulldogs. The median BOAS index of dogs that were operated on (20/29 candidates) decreased from 67% post-CMS to 42% after LATE (P < .001). Soft tissue proportion at the rostral entrance of choanae was the only predictor for candidacy for LATE. Pugs (P = .021; cutoff = 64%) and French bulldogs (P = .008; cutoff = 55%) with higher STC were more likely to be candidates for LATE. After LATE, 12 of 20 dogs had temporary episodes of reverse sneezing, and nasal noise was noted in 8 of 20 dogs when sniffing and excited. CONCLUSION: Laser-assisted turbinectomy was an effective treatment for dogs with intranasal abnormalities and a poor response to CMS. Soft tissue proportion at the rostral entrance of choanae was a predictor of candidacy for LATE in pugs and French bulldogs. CLINICAL SIGNIFICANCE: Computed tomography-based measurement of STC can be used to predict whether LATE is required in addition to CMS in pugs and French bulldogs with BOAS.
コメント1:CTおよびプレチスモグラフィを用いたBAOS重症度指標を用い、レーザー焼灼補助下鼻甲介切除術(LATE)の効果を評価した論文。従来の複合的上気道整復術でもBAOS重症度指標が十分改善しなかった症例をLATE適応とした。LATEを適用し、さらにBAOS指標は改善した。多変量解析にてLATE適応の予測因子はCT上での鼻甲介入り口部分の軟部組織比率であった(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
コメント2:CT検査による後鼻孔吻側入口における断面積での軟部組織比率(STC)が高いほど、レーザーによる鼻甲介切除術の適用となりやすい。一方、吻側異常鼻甲介、尾側異常鼻甲介、鼻中隔変位については適用基準とはならない(いいのペットクリニック 飯野亮太-2020.12.29)。
2018
Liu NC, Troconis EL, McMillan M, et al. Endotracheal tube placement during computed tomography of brachycephalic dogs alters upper airway dimensional measurements. Vet Radiol Ultrasound 2018;59:289-304.
気管内挿管がCTを用いた気道の測定に与える影響
Computed tomography (CT) is used to document upper airway lesions in dogs with brachycephalic obstructive airway syndrome. The presence of an endotracheal tube during CT scanning is often required for general anesthesia. We hypothesized that the endotracheal tube placement would change the soft tissue dimensions of the upper airway. The aims of this prospective, method comparison study were to evaluate the reliability of the previously reported upper airway CT measurements with endotracheal tube placement, and to propose measurements that are minimally affected by the endotracheal tube. Twenty brachycephalic dogs were included in this study. Each dog underwent head/neck CT with an endotracheal tube, followed by a second scan without the endotracheal tube. Ten measurements of the soft palate, nasopharynx, and trachea were performed. Tracheal dimension was significantly larger with the endotracheal tube compared to without, whereas the soft palate cross-sectional area was significantly smaller with the endotracheal tube than without the endotracheal tube. The influence of the endotracheal tube on the caudal nasopharynx cross-sectional (transverse-sectional) area varied with a mean proportional absolute difference of 35%. Rostral soft palate thickness, tracheal perimeter, and cross-sectional area of the rostral nasopharynx were the measurements least affected by the endotracheal tube (intraclass correlation coefficient = 0.964, 0.967, and 0.951, respectively). Therefore, we proposed that these three measurements may be most useful for future brachycephalic obstructive airway syndrome studies that require CT scanning of intubated animals. However, with endotracheal tube placement, measurements of soft palate length, caudal nasopharyngeal cross-sectional area, and trachea height and width may not be reliable.
コメント:気管内挿管がCTを用いた気道の測定に与える影響に関する論文。挿管をすることでしない場合と比較し、軟口蓋の厚さ、気管内径、吻側側の鼻咽頭の横断面積に有意な変化はなかった。一方、軟口蓋の長さ、尾側の鼻咽頭の横断面積、気管の高さと幅は変化があり信頼できない(ダクタリ動物病院東京医療センター 田畑達彦-190502)。
Kaye BM, Rutherford L, Perridge DJ, et al. Relationship between brachycephalic airway syndrome and gastrointestinal signs in three breeds of dog. J Small Anim Pract 2018;59:670-673.
短頭3犬種における短頭種気道症候群と消化器症状との関連
OBJECTIVES: To assess the breed-specific prevalence of, and effects of corrective airway surgery on, gastrointestinal signs in French bulldogs, English bulldogs and pugs presenting with brachycephalic airway syndrome to a referral teaching hospital. MATERIALS AND METHODS: In this retrospective study, ptyalism, regurgitation and vomiting were graded at presentation using a previously established scoring system. Staphylectomy and nares resection were performed on all dogs. Gastrointestinal signs were re-assessed via telephone follow-up at least 6 weeks after surgery. RESULTS: Ninety-eight dogs were included: French bulldogs (n=43), English bulldogs (n=12) and pugs (n=43). Overall population prevalence of all gastrointestinal signs was 56%. Breed-specific prevalence for French bulldogs was 93%, English bulldogs 58% and pugs 16%. There was post-surgical clinical improvement in gastrointestinal signs for the whole study population, especially in French bulldogs. CLINICAL SIGNIFICANCE: The prevalence of gastrointestinal signs in dogs presenting with brachycephalic airway syndrome and improvement in these clinical signs following corrective surgery may vary between breeds.
コメント1:短頭種における軟口蓋過長および外鼻孔狭窄整復後の転帰に関する論文。Includeされた犬の約半数で消化器兆候が認められ、またその割合はフレンチブルドッグで圧倒的に高かった。また、術後全ての犬で消化器兆候は改善した(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
コメント2:フレンチブルドッグ43頭、イングリッシュブルドッグ12頭、パグ43頭について、軟口蓋過長整復術、外鼻孔狭窄整復術前後の胃腸症状(流涎、胃食道逆流、嘔吐)の発生率を調査した文献。3犬種合わせると胃腸症状の発生率は56%であったが、犬種ごとにみてみるとフレンチブルドッグ93%、イングリッシュブルドッグ58%、パグ16%だった。術後、胃腸症状がもっとも改善したのはフレンチブルドッグであった(まるふく動物病院 福田大介-2019.4.2)。
Arulpagasam S, Lux C, Odunayo A, et al. Evaluation of Pulse Oximetry in Healthy Brachycephalic Dogs. J Am Anim Hosp Assoc 2018;54:344-350. PDFあり
健康な短頭種におけるパルスオキシメーターの評価
Brachycephalic airway syndrome (BAS) is characterized by increased upper airway resistance due to conformational abnormalities occurring in brachycephalic dogs (BD). In this prospective study, we evaluated pulse oximetry (SpO2) and arterial blood gas values in 18 healthy BD and compared these values with those of 18 healthy mesocephalic and dolichocephalic dogs (MDD). All dogs were assigned a BAS score based on an owner questionnaire. Inclusion criteria included presentation to the hospital for a problem unrelated to the respiratory system and unremarkable blood analyses and physical examination. In awake dogs, SpO2 values were obtained from a minimum of two sites. Dogs were then sedated, and SpO2 values were obtained again concurrently with an arterial blood gas sample. The SpO2 values were significantly lower in BD compared with MDD, but there were no statistically significant differences between BD and MDD for any arterial blood gas parameters. Based on the BAS score, BD who were moderately BAS-affected (n = 5), had significantly lower arterial saturation of hemoglobin with oxygen values on arterial blood gas when compared with MDD (n = 18). Although BD had statistically lower SpO2 values than MDD, the mean SpO2 values for both groups were within the normal range.
コメント:健康な短頭種18頭(うち、中等度のBASと評価された犬が5頭)と非短頭種18頭をSpO2、SaO2について比較。短頭種では非短頭種に比べ有意にSpO2が低かったが、SaO2で有意差は認められなかった。中等度BAS群5頭と非短頭種群を比べると、SaO2でも有意差が認められた(まるふく動物病院 福田大介-2019.4.2 )。
Hughes JR, Kaye BM, Beswick AR, et al. Complications following laryngeal sacculectomy in brachycephalic dogs. J Small Anim Pract 2018;59:16-21. (PDFあり)
短頭種気道症候群における喉頭小嚢切除術後合併症
OBJECTIVES: To evaluate the effect of sacculectomy on the immediate postoperative complication rate in dogs affected with brachycephalic obstructive airway syndrome. MATERIALS AND METHODS: Retrospective review of clinical records of brachycephalic dogs with everted saccules that underwent surgery for brachycephalic obstructive airway syndrome between 2009 and 2014. Dogs were grouped as those having nares resection and staphylectomy only and those having nares resection, staphylectomy and laryngeal sacculectomy. Complications were scored as mild, moderate or severe. RESULTS: In total, 37 dogs were included in the sacculectomy group and 44 in the comparator group. Dogs that had undergone sacculectomy were more likely to develop postoperative complications, with 18 of 37 developing complications, nine of which were moderate to severe. In the group without sacculectomy, nine of 44 dogs developed complications, of which one was severe. Different breed distribution between groups might also impact this outcome. CLINICAL SIGNIFICANCE: The results suggest that sacculectomy might increase morbidity following brachycephalic airway surgery, but repeat studies are required to confirm this result. Further information is also required to determine whether the short-term risks of sacculectomy are outweighed by superior long-term functional outcome.
コメント:外科療法が適応となったBAS犬81頭を、喉頭小嚢切除術群(軟口蓋過長整復術+外鼻孔狭窄整復術+喉頭小嚢切除術)37頭と非喉頭小嚢切除術群(軟口蓋過長整復術+外鼻孔狭窄整復術)44頭に分け、術直後期合併症を比較した後ろ向き研究。喉頭小嚢切除術群では、18/37で合併症が発生し、そのうち9頭が中等度~重度であった。非喉頭小嚢切除術群では、9/44で合併症が発生し、そのうち1頭が重度であった(まるふく動物病院 福田大介-2019.4.2)。
Norgate D, Ter Haar G, Kulendra N, et al. A comparison of the effect of propofol and alfaxalone on laryngeal motion in nonbrachycephalic and brachycephalic dogs. Vet Anaesth Analg 2018;45:729-736. (PDFあり)
非短頭犬種と短頭犬種間におけるプロポフォールとアルファキサノンの喉頭運動への効果の比較
OBJECTIVE: To compare the effect of propofol and alfaxalone on laryngeal motion under a light plane of anaesthesia in nonbrachycephalic and brachycephalic dogs anaesthetized for nonemergency procedures. STUDY DESIGN: Prospective, randomized clinical trial. ANIMALS: A total of 48 client-owned dogs (24 nonbrachycephalic and 24 brachycephalic). METHODS: A standardized premedication of methadone (0.2 mg kg(-1)) and acepromazine (0.01 mg kg(-1)) was administered intramuscularly. Dogs were randomly assigned to be induced with increments of propofol (1-4 mg kg(-1)) or alfaxalone (0.5-2 mg kg(-1)). Laryngeal assessment was performed under a light plane of anaesthesia by a surgeon (GTH) who was unaware of the induction protocol. Laryngeal movement was assessed as either being present when abduction of the laryngeal cartilages upon inspiration was identified, or absent when abduction was not recognized. Simultaneously, a 60-second video was recorded. The same surgeon (GTH) and an additional surgeon (NK) re-evaluated the videos 1 month later. Categorical comparisons were studied using Chi square and Fisher’s exact test where appropriate. Pairwise evaluation of agreement between scorers was undertaken with the kappa statistic (kappa). RESULTS: There were no significant differences (p > 0.05) identified between the presence or absence of laryngeal motion between dogs administered propofol or alfaxalone, as well as when analysing nonbrachycephalic and brachycephalic dogs separately. The majority of dogs (>75%) maintained some degree of laryngeal motion with both protocols. Agreement between assessors was excellent (kappa = 0.822). CONCLUSIONS: Alfaxalone maintained laryngeal motion similarly to propofol in nonbrachycephalic and brachycephalic dogs. CLINICAL RELEVANCE: Both agents would appear appropriate for allowing assessment of laryngeal motion in nonbrachycephalic and brachycephalic dogs. The assessment technique of subjective evaluation of laryngeal motion via peroral laryngoscopy under a light plane of anaesthesia produced consistent results amongst assessors, regardless of the induction agent used.
コメント:48頭の飼育犬(24頭の短頭種、24頭の非短頭種)の喉頭鏡検査にて、麻酔導入剤をプロポフォール、アルファキサロンの二種で使い分け、喉頭の運動機能への影響を評価した前向き無作為下臨床試験
目的
1、プロプフォールとアルファキサロンでの喉頭運動機能への影響の差異の確認
2、検査者間での喉頭運動機能評価の差異の確認
プロトコル
前投与アセプロマジン0.01mg/kg、メサドン0.2mg/kg
導入プロポフォール4mg/kg、アルファキサロン2mg/kg、to effect投与
結果
1、使用導入剤、短頭種、非短頭種に関わらず、87.5%の犬で喉頭運動を確認できた。
2、検査者間において、喉頭鏡下喉頭運動性の評価に差異は出なかった。
新奇性として捉えられる点
1、2004年のjacksonらの報告にて、アセプロマジンは喉頭運動機能抑制があるとされているが、本研究では報告の1/5量である0.01mg/kgで使用したことにより、導入薬剤の投与速度を下げることを可能にし、検査においての導入薬剤必要最低用量を投与することができた。これにより、喉頭運動機能抑制を最低限にしたのではないかと考えられるため、前投与としてアセプロマジンは有用性があると考えられる。
2、2004年のjacksonらの報告にて、喉頭評価にはチオペンタール導入が最適とされているが、2017年のSmalleらの報告にて、六頭の犬においてアルファキサロン、プロポフォール、チオペンタールで差異なしとされている。2015年のMonagleらの報告にて、人では、脳幹におけるニューロステロイドが標的とするGABA受容体が無いことにより、アルファキサロンは脳幹での活性を示さないため、アルファキサロンが気道抵抗、呼吸運動への影響が最も少ないとされている。
犬の脳幹におけるGABA受容体の局在性を論じた報告はないため、人同様の結果が生じるかは確かではないが、短頭種や呼吸障害がある犬の検査時の安全性も考慮し、より呼吸抑制が低いとされるアルファキサロンを第一選択として考えて良いのではないか。
(上大岡キルシェ動物病院 山下 智之-2019.3.12)
Sarran D, Caron A, Testault I, et al. Position of maximal nasopharyngeal maximal occlusion in relation to hamuli pterygoidei: use of hamuli pterygoidei as landmarks for palatoplasty in brachycephalic airway obstruction syndrome surgical treatment. J Small Anim Pract 2018. (PDFあり)
翼状突起に関連した最大鼻咽頭閉塞位置:短頭種閉塞性気道症候群の外科的治療における軟口蓋切除時のランドマークとして翼状突起の利用
OBJECTIVES: To assess the influence of complete nasopharyngeal occlusion on respiratory signs in brachycephalic dogs. To determine the cranio-caudal position of rostral nasopharyngeal occlusion in relation to the hamuli pterygoidei in brachycephalic dogs. To determine whether using the hamuli pterygoidei as anatomical landmarks for palatoplasty results in clinical respiratory improvement. MATERIALS AND METHODS: Prospective study of dogs diagnosed with brachycephalic obstructive airway syndrome. The dogs were scored according to the severity of their clinical respiratory signs and the nasopharynx was CT scanned. The site of most rostral nasopharyngeal occlusion was measured in relation to the hamuli pterygoidei. Measurements were compared between brachycephalic obstructive airway syndrome group, completely occluded and partially occluded groups. The hamuli pterygoidei were used as the most cranial landmarks for the palatoplasty incision, such that the incision was made at the point of maximal nasopharyngeal occlusion. Owners were interviewed through telephone for the medium-term follow-up. RESULTS: Thirty-five dogs were included. There was no significant association between the severity of respiratory clinical signs and extent of nasopharyngeal occlusion. Maximal nasopharyngeal occlusion was always located directly caudal to the hamuli pterygoidei (mean +/-sd value of 94 +/-65 mm). hamuli pterygoidei were easily palpable perioperatively in all cases. There was a significant improvement of clinical grades postoperatively. CLINICAL SIGNIFICANCE: The hamuli pterygoidei are a reliable landmark for soft palate incision for palatoplasty in these cases but the distance between them and the site of maximal nasopharyngeal occlusion varied greatly.
コメント:短頭種閉塞性気道症候群であるフレンチブルドックの軟口蓋切除において、翼状突起をランドマークとして、CT検査にて鼻咽頭道の最大閉塞位置を決定し手術を実施した前向き試験。臨床的グレードは有意に低下したが、鼻咽頭の閉塞状態(完全もしくは部分)と臨床的グレードとの関連はなかった。従来の方法による軟口蓋切除より全例において吻側位置で行ったが、術後に鼻炎は認められなかった(いいのペットクリニック 飯野亮太-2019.3.3)。
Downing F, Gibson S. Anaesthesia of brachycephalic dogs. J Small Anim Pract 2018;59:725-733.
短頭種の麻酔
Brachycephalic breeds of dog have grown in popularity in the UK and so form an increasing proportion of cases requiring anaesthesia. These breeds are predisposed to several conditions, notably brachycephalic obstructive airway syndrome and gastro-oesophageal reflux, that have important implications for anaesthetic management and carry high risk for complications. This review incorporates peer-reviewed veterinary literature with clinical experience in a discussion on perioperative management of brachycephalic dogs. We focus on preoperative identification of common concurrent conditions, practical strategies for reducing anaesthetic risk and improving postoperative management. Comparisons of brachycephalic obstructive airway syndrome with the human condition of obstructive sleep apnoea are included where appropriate.
コメント:BASのレビュー。BASとヒトのOSAを比較している。OSA患者では、術前術後のCPAP療法や呼吸理学療法が必須となっているが、獣医療では、メリット・デメリットなどを考慮し適応を検討する必要がある(まるふく動物病院 福田大介-2018.12.20)。
2017
Belch A, Matiasovic M, Rasotto R, et al. Comparison of the use of LigaSure versus a standard technique for tonsillectomy in dogs. Vet Rec 2017;180:196.
LigaSureを用いた扁桃腺切除の有用性
The principal aim of this study was to document the effectiveness of tonsillectomy in dogs using a vessel-sealing device compared with a standard technique with tonsillectomy forceps. A secondary aim of the study was to document histopathological changes of the excised tonsillar tissue in dogs with brachycephalic obstructive airway syndrome. 20 dogs were studied. The time taken to remove a tonsil using LigaSure was a mean of 44.8 seconds (sd 15 seconds, 95 per cent CI 40 to 57 seconds) and with the standard technique a mean of 305.9 seconds (sd 67 seconds, 95 per cent CI 272 to 349 seconds). Significantly less haemorrhage occurred using LigaSure compared with the standard technique. Histopathology of the tonsils was characterised by multifocal neutrophilic and lymphocytic inflammation, and 1-2 mm of heat-induced coagulation necrosis at the cut edge of LigaSure tonsils. This study shows that LigaSure is significantly faster and resulted in less bleeding than the standard technique.
コメント:扁桃腺切除を従来法とLigaSureを用いた方法とで比較した論文。LigaSureを用いた場合、手術時間約50分と従来法の約1/5であり、出血も有意に少なかった(ダクタリ動物病院東京医療センター 田畑達彦-2019.5.1)。
Liu NC, Oechtering GU, Adams VJ, et al. Outcomes and prognostic factors of surgical treatments for brachycephalic obstructive airway syndrome in 3 breeds. Vet Surg 2017;46:271-280.
BAOS3犬種(バグ、フレンチブル、イングリッシュブルドッグ)における外科手術の転帰と予後因子
OBJECTIVE: To determine prognostic indicators for the surgical treatment of brachycephalic obstructive airway syndrome (BOAS) and to compare the prognosis of 2 multilevel surgical procedures. STUDY DESIGN: Prospective clinical study. SAMPLE POPULATION: Client-owned pugs, French bulldogs, and bulldogs (n = 50). METHODS: Noninvasive whole-body barometric plethysmography (WBBP) was used to assess respiratory function before, 1 month and 6 months after upper airway corrective surgery. Postoperatively, BOAS indices (ie, ascending severity score generated from WBBP data, 0%-100%) that equaled to or exceeded the cut-off values of BOAS in the diagnostic models were considered to have a “poor prognosis.” A multivariate logistic regression was used to assess predictors for prognosis. RESULTS: The median BOAS indices decreased after surgery (from 76% to 63%, P < .0001), although dogs with indices in this range would still be considered clinically affected. Age (odds ratios [OR] = 0.96, 95% confidence interval [CI]: 0.93-0.99, P < .05), body condition (OR = 0.06, 95% CI: 0.01-0.39, P < .01), laryngeal collapse (OR = 6.1, 95% CI: 1-37.22, P < .05), and surgical techniques (OR = 7.94, 95% CI: 1.17-54.01, P < .05) were associated with postoperative prognosis. The multivariate model suggests modified multilevel surgery (MMS) may have a better outcome than traditional multilevel surgery (TMS) (P = .034). The positive predictive value of the logistic model was 84% (95% CI: 68-94%) and the area under the receiver operating characteristic (ROC) curve was 89% (95% CI: 78-99%, P <.0001). CONCLUSIONS: Younger age, normal body condition, presence of laryngeal collapse, and treatment with TMS were negative prognostic factors after surgical treatment of BOAS. MMS is recommended, particularly in dogs with a higher probability of poor prognosis.
コメント1:プレチスモグラフィを用いてBOAS手術前後の臨床的な改善だけでなく、客観的な指標を用い比較し、予後因子を検討した論文。若齢であること、BCS<7/9、喉頭虚脱のグレードがⅡまたはⅢであること、術式が新従来の術式であることが予後不良因子であった(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
コメント2:術前に若齢であることが術後にBAOS指標が悪化し、術前に肥満体型(BCS7/9以上)が術後のBAOS指標が改善するということは理解し難い(犬・猫の呼吸器科 城下幸仁−2019.3.26)。
Liu NC, Troconis EL, Kalmar L, et al. Conformational risk factors of brachycephalic obstructive airway syndrome (BOAS) in pugs, French bulldogs, and bulldogs. PLoS One 2017;12:e0181928.
パグ、フレンチブル、ブルドッグのBASの構造的危険因子
Extremely brachycephalic, or short-muzzled, dog breeds such as pugs, French bulldogs, and bulldogs are prone to the conformation-related respiratory disorder-brachycephalic obstructive airway syndrome (BOAS). Affected dogs present with a wide range of clinical signs from snoring and exercise intolerance, to life-threatening events such as syncope. In this study, conformational risk factors for BOAS that could potentially aid in breeding away from BOAS were sought. Six hundred and four pugs, French bulldogs, and bulldogs were included in the study. Soft tape measurements of the head and body were used and the inter-observer reproducibility was evaluated. Breed-specific models were developed to assess the associations between the conformational factors and BOAS status based on functional grading. The models were further validated by means of a BOAS index, which is an objective measurement of respiratory function using whole-body barometric plethysmography. The final models have good predictive power for discriminating BOAS (-) and BOAS (+) phenotypes indicated by the area under the curve values of >80% on the receiver operating curves. When other factors were controlled, stenotic nostrils were associated with BOAS in all three breeds; pugs and bulldogs with higher body condition scores (BCS) had a higher risk of developing BOAS. Among the standardized conformational measurements (i.e. craniofacial ratio (CFR), eye width ratio (EWR), skull index (SI), neck girth ratio (NGR), and neck length ratio (NLR)), for pugs EWR and SI, for French bulldogs NGR and NLR, and for bulldogs SI and NGR showed significant associations with BOAS status. However, the NGR in bulldogs was the only significant predictor that also had satisfactory inter-observer reproducibility. A NGR higher than 0.71 in male bulldogs was predictive of BOAS with approximately 70% sensitivity and specificity. In conclusion, stenotic nostrils, BCS, and NGR were found to be valid, easily applicable predictors for BOAS (+).
コメント1:604頭のパグ、フレンチブル、ブルドッグで、BASの構造的危険因子を調べた報告。3犬種すべてに共通する危険因子:外鼻孔狭窄の重症度。パグ、ブルドッグに共通する危険因子:BCS。NGR(胸郭に対する首の太さ)は、測定者間の誤差が少なく、オスのブルドッグで信頼できる危険因子である。ただし、これら構造的評価だけでなく、機能的評価を組み合わせることがとても重要である(まるふく動物病院 福田大介-2018.12.20)
コメント2:犬種特異的な解剖学的特徴とプレチスモグラフィを用いた呼吸機能評価によりBOASの特徴づけおよび罹患予測因子を検討した論文。種差はあるが、短頭種において外鼻腔狭窄、BCS、頚周囲長がBOAS罹患と有意に関連していた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Crane C, Rozanski EA, Abelson AL, et al. Severe brachycephalic obstructive airway syndrome is associated with hypercoagulability in dogs. J Vet Diagn Invest 2017;29:570-573.
重度短頭種気道症候群と凝固亢進は関連する
We evaluated whether dogs with severe brachycephalic obstructive airway syndrome (BOAS) developed a hypercoagulable state similar to people with obstructive sleep apnea. Five dogs with grade 3 BOAS were included as well as 5 healthy control Labrador Retrievers. Venous blood samples were collected from each dog for performance of thromboelastography and determination of hematocrit and platelet count. Groups were compared using a t-test, with p < 0.05 considered significant. Thromboelastography results identified that all BOAS dogs were hypercoagulable compared to the Labradors, having significantly shortened clotting time with increased angle, maximal amplitude, and clot rigidity. BOAS dogs also had evidence of delayed fibrinolysis. These results are consistent with, but more severe than, those previously documented in apparently healthy Bulldogs. Together, these findings support the presence of a hypercoagulable state in brachycephalic dogs, and suggest that this state is amplified by increasing severity of BOAS.
コメント1:重度短頭種気道症候群罹患犬(n=5)に対し、トロンボエラストグラフィーを用いて凝固線溶系を評価したところ、凝固亢進と線溶抑制が認められた(まるふく動物病院 福田大介-2019.2.5)
コメント2:トロンボエラストグラフィを用いて短頭種における凝固活性を検討した論文。非短頭種と比較して、凝固時間の短縮や繊維素溶解の遅延が認められた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Hostnik ET, Scansen BA, Zielinski R, et al. Quantification of nasal airflow resistance in English bulldogs using computed tomography and computational fluid dynamics. Vet Radiol Ultrasound 2017;58:542-551.
CTおよびコンピューター流体力学にてイングリッシュブルドッグにおける鼻腔内抵抗の定量化の試み
Stenotic nares, edematous intranasal turbinates, mucosal swelling, and an elongated, thickened soft palate are common sources of airflow resistance for dogs with brachycephalic airway syndrome. Surgery has focused on enlarging the nasal apertures and reducing tissue of the soft palate. However, objective measures of surgical efficacy are lacking. Twenty-one English bulldogs without previous surgery were recruited for this prospective, pilot study. Computed tomography was performed using conscious sedation and without endotracheal intubation using a 128 multidetector computed tomography scanner. Raw multidetector computed tomography data were rendered to create a three-dimensional surface mesh model by automatic segmentation of the air-filled nasal passage from the nares to the caudal soft palate. Three-dimensional surface models were used to construct computational fluid dynamics models of nasal airflow resistance from the nares to the caudal aspect of the soft palate. The computational fluid dynamics models were used to simulate airflow in each dog and airway resistance varied widely with a median 36.46 (Pa/mm)/(l/s) and an interquartile range of 19.84 to 90.74 (Pa/mm)/(/s). In 19/21 dogs, the rostral third of the nasal passage exhibited a larger airflow resistance than the caudal and middle regions of the nasal passage. In addition, computational fluid dynamics data indicated that overall measures of airflow resistance may significantly underestimate the maximum local resistance. We conclude that computational fluid dynamics models derived from nasal multidetector computed tomography can quantify airway resistance in brachycephalic dogs. This methodology represents a novel approach to noninvasively quantify airflow resistance and may have utility for objectively studying effects of surgical interventions in canine brachycephalic airway syndrome.
コメント:多検出器列CTを用いて数値流体力学から鼻腔の気道抵抗を客観的に評価した論文。計算上の気流抵抗値は個体差が激しいものの、中間部や尾側よりも頭側での気流抵抗が顕著に高かった(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Lilja-Maula L, Lappalainen AK, Hyytiainen HK, et al. Comparison of submaximal exercise test results and severity of brachycephalic obstructive airway syndrome in English bulldogs. Vet J 2017;219:22-26.
イングリッシュ・ブルドッグにおける短頭種気道症候群の重症度と運動負荷試験結果との比較
Canine brachycephalic obstructive airway syndrome (BOAS) is a complex respiratory disease related to congenitally flattened facial and skull anatomy. BOAS causes respiratory distress, heat and exercise intolerance, and gastrointestinal signs. English bulldogs (EB) have a high prevalence of BOAS. Currently, the severity of BOAS signs in veterinary practice is assessed subjectively. To reduce BOAS in brachycephalic breeds, an objective and easy-to-use tool could help breeders select healthier animals. Exercise tests, such as the 6 min walk test (distance walked measured) or the 1000 m walk test (duration measured), could be used to assess the severity of BOAS, as exercise intolerance and impaired recovery are key features of BOAS. This study evaluated the severity of signs and anatomic components of BOAS in a group of prospectively recruited young adult EBs (n = 28) and investigated the correlations of the 6 min walk test or the 1000 m walk test with a veterinary assessment of BOAS severity, using an ordinal 4 level scale of respiratory signs. EBs with more severe BOAS walked a shorter distance, more slowly and their recovery from exercise took longer than those with only mild signs of BOAS. Control dogs of different breeds (n = 10) performed the exercise tests significantly better (i.e. longer distance, faster time and recovery) than EBs. Increases in body temperature during exercise were significantly higher in EBs than in controls. The results of this study support the use of exercise tests for objective evaluation of the severity of BOAS in EBs.
コメント:イングリッシュブルドッグのBOASの重症度判定に運動負荷試験を用いることに関して提案している論文。重症度に比例して運動不耐性が認められる(ダクタリ動物病院 東京医療センター 田畑達彦-2019.2.3)
Shaver SL, Barbur LA, Jimenez DA, et al. Evaluation of Gastroesophageal Reflux in Anesthetized Dogs with Brachycephalic Syndrome. J Am Anim Hosp Assoc 2017;53:24-31.
BAS犬の麻酔下胃食道逆流の評価
Brachycephalic airway syndrome may predispose to gastroesophageal reflux (GER) because of the high negative intrathoracic pressures required to overcome conformational partial upper airway obstruction. To investigate this, 20 dogs presenting for elective correction of brachycephalic airway syndrome (cases) and 20 non-brachycephalic dogs (controls) undergoing other elective surgeries were prospectively enrolled. Dogs underwent a standardized anesthetic protocol, and esophageal pH was monitored. Signalment, body weight, historical gastrointestinal and respiratory disease, complete blood count, serum biochemical values, radiographic findings, and anesthetic and surgical time were compared between cases and controls, and dogs that did and did not have basic (pH > 7.5), acidic (pH < 4), or any GER. Controls had higher mean esophageal pH (6.3) compared to cases (5.6, P = .019), but there was no difference in % with GER (cases 60%, controls 40%, P = .34). When all dogs were evaluated, dogs with GER had increased creatinine (P = .01), % positive for esophageal fluid on radiographs (P = .05), and body weight (P = .04) compared to those without GER. GER was common in both cases and controls, and cases had lower esophageal pH; however, greater numbers are required to determine if a true difference exists in % GER.
コメント:全身麻酔時、短頭種ではGER(胃食道逆流)が発生しやすいのかを調べるため、前向き研究を実施(短頭種20頭と非短頭種20頭で比較)した。結果として、短頭種群では麻酔中の食道内pHは非短頭種群に比べ低かったが、GERの発生率に有意差を認められなかった(まるふく動物病院 福田大介-2019.1.5)
Rutherford L, Beever L, Bruce M, et al. Assessment of computed tomography derived cricoid cartilage and tracheal dimensions to evaluate degree of cricoid narrowing in brachycephalic dogs. Vet Radiol Ultrasound 2017;58:634-646. doi:10.1111/vru.12526
短頭犬種の輪状軟骨狭窄評価のための輪状軟骨と気管横断面のCT評価
The aims of this observational, analytical, retrospective study were to (i) obtain computed tomographic (CT) cricoid dimensions (height, width, and transverse-sectional area), (ii) compare the cricoid dimensions between brachycephalic and mesaticephalic breeds, and (iii) compare cricoid cartilage dimensions between dogs without and affected with brachycephalic airway syndrome. The study is important to help to further evaluate and understand the anatomical components of brachycephalic airway syndrome. Measurements were performed in 147 brachycephalic and 59 mesaticephalic dogs. The cricoid cartilage was found to be significantly more oval in Pugs and French Bulldogs compared to mesaticephalic breeds. The cricoid cartilage transverse-sectional area was smallest for the Pug and, after adjusting for weight, significantly smaller for Pugs (P < 0.001), Boston Terriers (P = 0.001), and French Bulldogs (P < 0.001) compared to Jack Russell Terriers. The tracheal transverse-sectional area at C4 of English Bulldogs was significantly smaller than for Jack Russell Terriers (P = 0.005) and Labradors (P < 0.001). The cricoid cartilage transverse-sectional area:weight ratio was significantly lower in brachycephalic breeds compared to mesaticephalic breeds (P < 0.001). The cricoid cartilage:trachea at C4 transverse-sectional area for brachycephalic dogs was significantly larger than for mesaticephalic dogs (<0.001), demonstrating that the trachea was the narrowest part of the airway. No significant differences were found for cricoid dimensions between dogs affected with and without brachycephalic airway syndrome. However, large individual variation was found among the brachycephalic breeds and further studies investigating the relationship between cricoid cartilage size, laryngeal collapse, concurrent tracheal hypoplasia, and/or severity of brachycephalic airway syndrome are warranted.
コメント:CTを用いて体重で標準化した輪状軟骨の横断径などを犬種別で比較した論文。パグ、フレンチブルドッグが特に喉頭の狭い犬種として挙げられている(ダクタリ動物病院 東京医療センター 田畑達彦-2018.12.30)
Reeve EJ, Sutton D, Friend EJ, Warren-Smith CMR. Documenting the prevalence of hiatal hernia and oesophageal abnormalities in brachycephalic dogs using fluoroscopy. J Small Anim Pract. 2017 Dec;58(12):703-708.
透視検査を用いた短頭種犬種における食道裂孔ヘルニアと食道異常の有病率の調査について
OBJECTIVES: To report the prevalence of abnormal fluoroscopic findings in brachycephalic dogs that were presented to a referral hospital for obstructive airway syndrome.
METHODS: Hospital records between May 2013 and November 2015 identified 36 brachycephalic dogs investigated for obstructive airway disease: 21 French bulldogs, six bulldogs, four Boston terriers, two pugs, two boxers and one shih-tzu. The presence or absence of hiatal hernia, delayed oesophageal transit, gastro-oesophageal reflux and redundant oesophagus were recorded.
RESULTS: Of the 36 dogs, 16 had hiatal hernia, all of which were French bulldogs; 31 dogs had delayed oesophageal transit time, 27 had gastro-oesophageal reflux, and four had redundant oesophagus.
CLINICAL SIGNIFICANCE: Clinical Significance: The prevalence of hiatal hernia is higher than expected in the French bulldog, and there was a high prevalence of oesophageal disease in this group in general. These results suggest a need to investigate similar cases for evidence of gastrointestinal disease that may also require attention.
コメント:単一施設において閉塞性気道疾患と診断された36頭の短頭種を用いた回顧的検討であり、食道裂孔ヘルニア、食道通過時間の遅延、胃食道逆流および食道過長の合併率を調査した。全体的に食道疾患の合併率は高く、特にFBは全例において食道裂孔ヘルニアを合併していた(ダクタリ動物病院 東京医療センター 田畑達彦-2018.11.29)。
Ellis J, Leece EA. Nebulized Adrenaline in the Postoperative Management of Brachycephalic Obstructive Airway Syndrome in a Pug. J Am Anim Hosp Assoc 2017;53:107-110. doi: 10.5326/JAAHA-MS-6466
短頭種気道症候群の術後管理にアドレナリンを配合したネブライザー療法が有効であった1例
Brachycephalic obstructive airway syndrome is a common problem in certain breeds, and may necessitate surgical procedures, such as rhinoplasty, palatoplasty, laryngeal sacculectomy, and/or arytenoid laryngoplasty, to improve the quality of life. However, laryngeal edema may necessitate the use of temporary tracheostomy tubes postoperatively to maintain a patent airway. This case demonstrates that administration of nebulized adrenaline in the immediate postoperative period where upper airway obstruction is life threatening can be used to reduce edema, therefore avoiding the need for tracheostomy.
コメント:パグにおいて短頭種気道症候群ope後の喉頭浮腫に対し、一時気管切開でなくアドレナリン噴霧の有用性を検討した論文(ダクタリ動物病院 東京医療センター 田畑達彦-2018.11.29)。
Schuenemann R, Pohl S, Oechtering GU. A novel approach to brachycephalic syndrome. 3. Isolated laser-assisted turbinectomy of caudal aberrant turbinates (CAT LATE). Vet Surg 2017;46:32-38.
短頭種症候群への新しいアプローチ 3.尾側異常鼻甲介の単独レーザー鼻甲介切除術
OBJECTIVE: To describe isolated laser-assisted turbinectomy of caudal aberrant turbinates (CAT LATE) as a new minimally invasive surgical procedure for the treatment of brachycephalic dogs with obstructing caudal aberrant turbinates (CAT). STUDY DESIGN: Prospective clinical study. ANIMALS: Brachycephalic dogs (24 Pugs, 1 English Bulldog) with CAT but adequate air spaces between the lamellae of the nonobstructing ventral nasal concha. METHODS: A rhinoscopically guided diode laser fiber introduced from anterior was used to dissect CAT within the nasopharyngeal meatus, while leaving the intranasal turbinates intact. Small grasping forceps were used to extract the dissected CAT from anterior or to push it through the nasopharyngeal meatus for extraction from posterior. RESULTS: Isolated CAT LATE was successfully performed on 32 CAT in 25 dogs. Intranasally applied xylometazoline helped shrink the ventral concha, making the approach and extraction easier. Minor bleeding was the only complication observed. CONCLUSION: It is possible to remove CAT with endoscopically applied diode-laser energy while leaving the nonobstructing ventral nasal concha intact.
コメント:鼻腔内に閉塞がなく、鼻咽道内の尾側異常鼻甲介に対して単独のレーザー鼻甲介切除術を実施した前向き臨床研究。合併症は最小の出血のみであったが、マルチレベル手術の一つとして実施しているため、臨床症状の改善との関連性は不明。対象犬種はほぼパグで占められている(いいのペットクリニック 飯野亮太-2020.12.29)。
2016
Pohl S, Roedler FS, Oechtering GU. How does multilevel upper airway surgery influence the lives of dogs with severe brachycephaly? Results of a structured pre- and postoperative owner questionnaire. Vet J 2016;210:39-45.
同時複数部位上気道外科手術は重度短頭の生活にどのような影響を与えるのか? 飼い主への術前・術後のおける問診表記載の集計結果
Brachycephalic airway syndrome in dogs is typified by a variety of anatomical abnormalities causing a diverse spectrum of clinical signs of varying intensity. This variability makes the assessment of the surgical outcome after upper airway surgery difficult. Using a structured questionnaire, the present study investigated the dog owner-perceived severity and frequency of a broad spectrum of welfare-relevant impairments 2 weeks before and 6 months after brachycephalic dogs underwent a recently developed multi-level upper airway surgery. All dogs underwent surgical treatment of stenotic nares (ala-vestibuloplasty), the nasal cavity (laser-assisted turbinectomy, LATE), the pharynx (palatoplasty and tonsillotomy), and if indicated, laryngeal surgery (laser-assisted ablation of everted ventricles and partial cuneiformectomy). Owners of brachycephalic dogs (n = 102) referred for upper airway surgery were eligible to participate. Questionnaire data from owners of 37 Pugs and 25 French bulldogs were evaluated. In all dogs, the clinical signs associated with brachycephaly improved markedly after surgery. Most encouraging was the striking reduction in life-threatening events by 90% (choking fits decreased from 60% to 5% and collapse from 27% to 3%). The incidence of sleeping problems decreased from 55% to 3%, and the occurrence of breathing sounds declined by approximately 50%. There was a marked improvement in exercise tolerance and a modest improvement in heat tolerance. Dogs with severe brachycephaly benefitted substantially from multi-level surgery, and there were particular improvements in the incidences of severe impairment and life-threatening events. However, despite the marked improvement perceived by dog owners, these dogs remained clinically affected and continued to show welfare-relevant impairments caused by these hereditary disorders.
コメント:短頭種のオーナーに種々の手技を組み合わせた上気道外科整復術前後での症状の変化について、一定の問診票を作成しアンケート結果を集計した。全ての犬で症状は軽減し、約半数の犬で窒息や睡眠障害の顕著な減少も認められた。飼い主主観では症状は改善したという結果が得られたが、臨床症状は残存していた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Oechtering GU, Pohl S, Schlueter C, et al. A Novel Approach to Brachycephalic Syndrome. 1. Evaluation of Anatomical Intranasal Airway Obstruction. Vet Surg 2016;45:165-172.
短頭種気道症候群に対する新しいアプローチ1:解剖学的鼻道閉塞の評価
OBJECTIVE: To evaluate airway obstruction due to abnormal intranasal anatomy in 3 brachycephalic dog breeds using computed tomography and rhinoscopy. STUDY DESIGN: Prospective clinical study. ANIMALS: A total of 132 brachycephalic dogs (66 Pugs, 55 French Bulldogs, and 11 English Bulldogs) with severe respiratory distress due to brachycephalic syndrome. METHODS: Computed tomography and anterior and posterior rhinoscopy were performed to evaluate endonasal obstruction. RESULTS: All dogs had abnormal conchal growth that obstructed the intranasal airways. Rostral aberrant turbinates (RAT) were common in Pugs (90.9%) but less frequent in French (56.4%) and English (36.4%) Bulldogs. Caudal aberrant turbinates (CAT) obstructing the nasopharyngeal meatus were commonly found in all breeds (66.7%). Deviation of the nasal septum was an almost consistent finding in Pugs (98.5%) but was less common in bulldogs. Obstructing turbinates had multiple points of mucosal contact responsible for obstruction of the intranasal airway. Interconchal and intraconchal mucosal contacts were evident in 91.7% of dogs. CONCLUSION: Selective breeding for short head conformation reduces the size of the nasal cavities to such an extent that intranasal structures grow aberrantly and malformed, leading to obstructed air conducting spaces. Intranasal airway obstruction of brachycephalic dogs may contribute to their exercise and heat intolerance because of impaired pulmonary ventilation and compromised thermoregulatory functions of the canine nose. Failure to address intranasal obstruction might be an explanation for lack of therapeutic success after conventional surgery for brachycephalic syndrome. Future consideration should be given to the diagnosis, management, and treatment of this newly described aspect of airway obstruction.
コメント1:重度上気道閉塞を示したパグ、フレンチブルドッグ、イングリッシュブルドッグの鼻道閉塞の構造的評価を、CT検査、前方および後方鼻鏡検査にて前向き臨床研究にておこなった。全ての犬で鼻甲介軟骨の異常形成にて鼻道が閉塞していた。鼻甲介前部の形成異常はパグで90.9%認められ、鼻甲介後部の形成異常による後鼻孔閉塞は3犬種とも67%に認められた。鼻中隔変位がほとんどのパグ(98.5%)で認められた。従来の上気道外科整復術で十分な成果が得られなかった一つの説明として鼻腔内閉塞に対する処置を行っていなかったことがあるかもしれない(犬・猫の呼吸器科 城下幸仁−2019.3.13)。
コメント2:短頭種の鼻腔を鼻鏡にて評価した論文。頭側および尾側鼻甲介異常、鼻中隔の変位および鼻粘膜の異常が認められたが、特に頭側鼻甲介異常および鼻中隔の変位はほとんど全てのパグにおいて認められた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
コメント3:重度呼吸窮迫状態のパグ、フレンチブルドック、イングリッシュブルドックでは、CT検査、前部及び後部鼻鏡検査において全頭で異常な鼻甲介をもっていた。特に、パグではほぼ全例で鼻中隔変位があり、その凹部と吻側異常鼻甲介の発生と関連性がみられた。短頭種の鼻腔内閉塞を引き起こす解剖学的要因として、1)腹及び中鼻甲介から発生する異常鼻甲介と、2)狭小化した鼻腔による相対的な鼻甲介肥厚と続く鼻腔内粘膜接触、及び鼻甲介の成長停止不全が挙げられる(いいのペットクリニック 飯野亮太-2020.12.29)。
Oechtering GU, Pohl S, Schlueter C, et al. A Novel Approach to Brachycephalic Syndrome. 2. Laser-Assisted Turbinectomy (LATE). Vet Surg 2016;45:173-181.
短頭種気道症候群に対する新しいアプローチ2:レーザー焼灼補助下鼻甲介切除術(LATE)
OBJECTIVE: To introduce a new surgical procedure based on interventional, laser-assisted removal of obstructing turbinate tissue to improve endonasal airway patency in brachycephalic dogs and to confirm the short and long term results using computed tomography (CT) and rhinoscopy. STUDY DESIGN: Prospective clinical study. ANIMALS: Brachycephalic dogs (n = 158; 70 Pugs, 77 French Bulldogs, 11 English Bulldogs) referred for treatment of severe respiratory distress because of brachycephalic syndrome. METHODS: Computed tomography and anterior and posterior rhinoscopy were performed to evaluate endonasal obstruction. Laser-assisted turbinectomy (LATE) using a diode laser was performed as part of a multilevel surgery. Nasal conchae that were causing airway obstruction were removed. RESULTS: The obstructing parts of the conchae were safely and efficiently removed by LATE, shaping a patent nasal airway in all dogs. The newly developed surgical procedure involved 3 steps: turbinectomy of the (1) concha nasalis ventralis; (2) rostral aberrantly growing turbinates (RAT); and (3) caudal aberrantly growing turbinates (CAT). Complications of the procedure included transient intraoperative hemorrhage in 51 of 158 dogs (32.3%); however, a temporary tamponade was necessary in only 2/158 dogs (1.3%). After 6 months, regrowth of turbinates required resection of possibly re-obstructing tissue in 25/158 dogs (15.8%; 1 Pug and 24 French Bulldogs). CONCLUSION: LATE is an effective method for creating a patent nasal airway in brachycephalic dogs with intranasal obstruction.
コメント1:前の報告を受けてBOAS犬種における鼻腔狭窄をレーザー焼灼により矯正した論文。術中合併症として術中出血が認められたが程度は軽く、術後の再発率は約16%であった(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
コメント2:腹側鼻甲介、吻側異常鼻甲介、尾側異常鼻甲介に対して、レーザーによる鼻甲介切除術を実施した前向き臨床試験。鼻腔狭窄の有無は、CTおよび鼻鏡検査における形態的評価されている。BASに対するマルチレベル手術の一つとして実施しているため、単独の効果は不明。合併症として、腹側鼻甲介切除時の蝶口蓋動脈の切除による術中出血が挙げられる(いいのペットクリニック 飯野亮太-2020.12.29)。
Liu NC, Adams VJ, Kalmar L, et al. Whole-Body Barometric Plethysmography Characterizes Upper Airway Obstruction in 3 Brachycephalic Breeds of Dogs. J Vet Intern Med 2016;30:853-865.
短頭種3犬種におけるボディプレチスモグラフィにおける上気道閉塞の特徴
BACKGROUND: A novel test using whole-body barometric plethysmography (WBBP) was developed recently to diagnose brachycephalic obstructive airway syndrome (BOAS) in unsedated French bulldogs. HYPOTHESIS/OBJECTIVES: The hypotheses of this study were: (1) respiratory characteristics are different between healthy nonbrachycephalic dogs and brachycephalic dogs; and among pugs, French bulldogs, and bulldogs; and (2) obesity and stenotic nares are risk factors for BOAS. The main objective was to establish a diagnostic test for BOAS in these 3 breeds. ANIMALS: A total of 266 brachycephalic dogs (100 pugs, 100 French bulldogs, and 66 bulldogs) and 28 nonbrachycephalic dogs. METHODS: Prospective study. Exercise tolerance tests with respiratory functional grading, and WBBP were performed on all dogs. Data from WBBP were associated with functional grades to train quadratic discriminant analysis tools to assign dogs to BOAS+ and BOAS- groups. A BOAS index (0-100%) was calculated for each dog. Receiver operating characteristic (ROC) curves were used to evaluate classification ability. RESULTS: Minute volume was decreased significantly in asymptomatic pugs (P = .009), French bulldogs (P = .026), and bulldogs (P < .0001) when compared to nonbrachycephalic controls. Respiratory characteristics were different among breeds and affected dogs had a significant increase in trace variation. The BOAS index predicted BOAS status for each breed with 94-97% (95% confidence interval [CI], 88.9-100%) accuracy (area under the ROC curve). Both obesity (P = .04) and stenotic nares (P = .004) were significantly associated with BOAS. CONCLUSIONS AND CLINICAL IMPORTANCE: The WBBP can be used as a clinical tool to diagnose BOAS noninvasively and objectively.
コメント:BOASの診断検査の創出を目的とした論文。ボディプレチスモグラフィを用いた呼吸特性検査は短頭種および非短頭種で有意に異なり、これに基づくBOAS指数は感度、特異度ともに高かった。また、肥満および外鼻腔狭窄はBOASと有意に関連していた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Heidenreich D, Gradner G, Kneissl S, et al. Nasopharyngeal Dimensions From Computed Tomography of Pugs and French Bulldogs With Brachycephalic Airway Syndrome. Vet Surg 2016;45:83-90.
短頭種気道症候群を示すパグとフレンチブルのCT検査での鼻咽頭腔の形状
OBJECTIVE: To describe the nasopharyngeal airway dimensions of two brachycephalic breeds and to localize the area of smallest airway dimensions. STUDY DESIGN: Prospective, descriptive, computed tomographic imaging study. ANIMALS: Thirty pugs and 30 French bulldogs with brachycephalic upper airway syndrome. METHODS: The thickness and length of the soft palate, cross-sectional area of the airway passage dorsal to the soft and hard palates, and cross-sectional area of the frontal sinus were measured and normalized to each dog’s skull index and body weight before statistical comparison between breeds. Nasopharyngeal turbinates and surrounding airway space, and a possible relationship between the canine tooth angulation and the severity of airway obstruction were assessed. RESULTS: Pugs had significantly smaller cross-sectional areas of the airway dorsal to the soft and hard palates than French bulldogs. In both breeds, the smallest nasopharyngeal cross-sectional areas were located dorsal to the caudal end of the soft palate. The soft palate of pugs was significantly shorter than that of French bulldogs and also significantly thinner when normalized to each dog’s skull index. Pugs more commonly exhibited nasopharyngeal turbinates. Pugs had significantly smaller air-filled cavities at the location of the frontal sinus. No correlation between the nasopharyngeal dimensions and canine tooth angulation was observed. CONCLUSION: Computed tomographic assessment of the upper airway morphology showed the smallest nasopharyngeal cross-sectional areas were located dorsal to the caudal end of the soft palate in both breeds. Pugs had a smaller nasopharyngeal cross-sectional area despite smaller soft palate dimensions than French bulldogs.
コメント:CTを用いてパグとFBの鼻腔内形態を評価した論文。両犬種とも軟口蓋尾側端背側部の鼻咽頭の横断面が最も小さかったが、どのレベルにおいてもパグはFBよりも鼻咽頭の横断面が小さく、軟口蓋自体も薄かった(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
2015
Liu NC, Sargan DR, Adams VJ, et al. Characterisation of Brachycephalic Obstructive Airway Syndrome in French Bulldogs Using Whole-Body Barometric Plethysmography. PLoS One 2015;10:e0130741.
Brachycephalic obstructive airway syndrome (BOAS) is an important health and welfare problem in several popular dog breeds. Whole-body barometric plethysmography (WBBP) is a non-invasive method that allows safe and repeated quantitative measurements of respiratory cycles on unsedated dogs. Here respiratory flow traces in French bulldogs from the pet population were characterised using WBBP, and a computational application was developed to recognise affected animals. Eighty-nine French bulldogs and twenty non-brachycephalic controls underwent WBBP testing. A respiratory functional grading system was used on each dog based on respiratory signs (i.e. respiratory noise, effort, etc.) before and after exercise. For development of an objective BOAS classifier, functional Grades 0 and I were considered to have insignificant clinical signs (termed here BOAS-) and Grades II and III to have significant signs (termed here BOAS+). A comparison between owner-perception of BOAS and functional grading revealed that 60 % of owners failed to recognise BOAS in dogs that graded BOAS+ in this study.WBBP flow traces were found to be significantly different between non-brachycephalic controls and Grade 0 French bulldogs; BOAS- and BOAS+ French bulldogs. A classifier was developed using quadratic discriminant analysis of the respiratory parameters to distinguish BOAS- and BOAS + French bulldogs, and a BOAS Index was calculated for each dog. A cut-off value of the BOAS Index was selected based on a receiver operating characteristic (ROC) curve. Sensitivity, specificity, positive predictive value, and negative predictive value of the classifier on the training group (n=69) were 0.97, 0.93, 0.95, and 0.97, respectively. The classifier was validated using a test group of French bulldogs (n=20) with an accuracy of 0.95. WBBP offers objective screening for the diagnosis of BOAS in French Bulldogs. The technique may be applied to other brachycephalic breeds affected by BOAS, and possibly to other respiratory disease in dogs.
コメント:「ボディプレチスモグラフィ(WBBP)を用いて、フレンブルのBAOS指標を求めた。BAOSの臨床グレーディングシステムと3分間運動負荷試験評価を組み合わせて、89頭のフレンチブルのBAOS指標を算出し、飼い主がBAOSと認識するレベルと、臨床グレードは進んでいても60%の飼い主はBAOSと認識しない指標値を比較した。この指標にて、感度、特異度、陽性予測値、陰性予測値は、それぞれ0.97、0.93、0.697、0.95であった。WBBPはフレンチブルのBAOS指標として非侵襲的な客観指標として利用可能である。」BAOSの客観指標のひとつとして今後研究に多用されそうです(犬・猫の呼吸器科 城下幸仁-2020.11.24)。
Cook DA, Moses PA, Mackie JT. Clinical effects of the use of a bipolar vessel sealing device for soft palate resection and tonsillectomy in dogs, with histological assessment of resected tonsillar tissue. Aust Vet J 2015;93:445-451.
バイポーラ血管シーリングシステムの軟口蓋過長と扁桃腺切除術への臨床効果
OBJECTIVE: To investigate whether soft palate resection and tonsillectomy with a bipolar vessel sealing device (BVSD) improves clinical respiratory score. To document histopathological changes to tonsillar tissue following removal with a BVSD. METHODS & RESULTS: Case series of 22 dogs with clinical signs of upper respiratory obstruction related to brachycephalic airway syndrome. Soft palate and tonsils were removed using a BVSD. Alarplasty and saccullectomy were also performed if indicated. A clinical respiratory score was assigned preoperatively, 24-h postoperatively and 5 weeks postoperatively. Excised tonsillar samples were measured and then assessed histologically for depth of tissue damage deemed to be caused by the device. Depth of tissue damage was compared between two power settings of the device. Soft palate resection and tonsillectomy with a BVSD lead to a significant improvement in respiratory scores following surgery. Depth of tissue damage was significantly less for power setting 1 compared with power setting 2. Using power setting 1, median calculated depth of tonsillar tissue damage was 3.4 mm (range 1.2-8.0). One dog experienced major complications. CONCLUSION: Soft palate resection and tonsillectomy with a BVSD led to significant improvement in clinical respiratory score.
コメント:軟口蓋過長、扁桃腺切除に関する論文。バイポーラ血管シーリングシステムを使うことで組織障害を抑えつつ、臨床症状の改善が得られた(ダクタリ動物病院東京医療センター 田畑達彦-2019.5.1)。
Haimel G, Dupre G. Brachycephalic airway syndrome: a comparative study between pugs and French bulldogs. J Small Anim Pract 2015;56:714-719
BOASのパグおよびフレンチブルの比較
OBJECTIVE: To compare clinical features of brachycephalic airway syndrome and long-term surgical outcomes between pugs and French bulldogs and evaluate the influence of laryngeal collapse. METHODS: This retrospective study included 72 dogs that underwent wedge rhinoplasty and folded flap palatoplasty for brachycephalic airway syndrome. Epidemiological data, clinical signs, postoperative complications and owners’ responses to a questionnaire at least six months after surgery were compared between pugs and French bulldogs. Spearman’s rank correlation tests were used for associating laryngeal collapse with age and respiratory signs before and after surgery. RESULTS: On the basis of the results of the owners’ questionnaires (available in 52/72 dogs), French bulldogs presented with lower activity levels and more severe digestive signs than pugs. Owners perceived clinical improvement in 88 . 5% of all dogs. The grades of respiratory and digestive signs were not different between the breeds in the long-term follow-up, and the grade of laryngeal collapse did not influence the grade of respiratory signs or surgical outcome. CLINICAL SIGNIFICANCE: Surgical treatment resulted in improved clinical signs in pugs and French bulldogs with brachycephalic airway syndrome, with a high owner satisfaction rate. There were no correlations between the severity of laryngeal collapse and overall respiratory signs or prognosis.
コメント:BOASのパグおよびフレンチブルの比較論文。フレンチブルのほうが活動性の低下や消化器症状が多かった。術後約9割の飼い主が臨床症状の改善を実感した。また、喉頭虚脱のグレードは呼吸器兆候のグレードや術後の転帰に影響しなかった(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Planellas M, Cuenca R, Tabar MD, et al. Clinical assessment and C-reactive protein (CRP), haptoglobin (Hp), and cardiac troponin I (cTnI) values of brachycephalic dogs with upper airway obstruction before and after surgery. Can J Vet Res 2015;79:58-63.
上気道閉塞を伴う短頭犬種における外科手術前後での臨床的評価とC-反応性蛋白(CRP)、ハプトグロブリン(Hb)、心筋トロポニンI(cTnI)値
Brachycephalic dogs have unique upper respiratory anatomy with abnormal breathing patterns that are similar to those in humans with obstructive sleep apnea syndrome (OSAS). The objectives of this multicenter prospective study were to assess the effects of surgical correction on clinical signs in dogs with brachycephalic airway obstructive syndrome (BAOS) and to evaluate the levels of several biomarkers [C-reactive protein (CRP); haptoglobin (Hp), and cardiac troponin I (cTnI)] used to determine systemic inflammation and myocardial damage. This study was conducted on 33 dogs with BAOS that were evaluated before and 1 to 2 mo after surgical correction. Palatoplasty was carried out by means of 2 different surgical techniques: carbon dioxide (CO2) laser (n = 12) and electrical scalpel (n = 21). Biomarker levels (CRP, Hp, and cTnI) were determined before and after surgery. There was a significant reduction in respiratory and gastrointestinal signs in dogs with BAOS after surgical treatment (P < 0.001). A greater reduction in respiratory signs (P < 0.002) was obtained using the CO2 laser. No statistical differences were found between CRP and cTnI levels, either before or after surgical correction. Haptoglobin concentration did increase significantly in the postsurgical period (P < 0.008). Surgical treatment in dogs with BAOS reduces clinical signs, regardless of the anatomical components present. Surgical treatment for BAOS is not useful to reduce CRP and Hp levels, probably because BAOS does not induce as obvious an inflammatory process in dogs as in human patients with OSAS. No reduction in cTnI levels was observed 1 mo after surgery in dogs with BAOS, which suggests that some degree of myocardial damage remains.
コメント;ヒトの閉塞性睡眠時無呼吸症候群では炎症反応と心血管疾患の関連が確立されているが、犬の短頭種閉塞性気道症候群では元々明らかな炎症は誘発されておらず、軟口蓋切除などの外科的な治療前後でも変化は認められない。一方、なんらかの心筋障害は引き起こされているかもしれないが、外科治療により臨床症状が緩和しても改善はみられない(いいのペットクリニック 飯野 亮太-2019.2.7)。
Kaye BM, Boroffka SA, Haagsman AN, et al. Computed Tomographic, Radiographic, and Endoscopic Tracheal Dimensions in English Bulldogs with Grade 1 Clinical Signs of Brachycephalic Airway Syndrome. Vet Radiol Ultrasound 2015;56:609-616.
CT、X線検査、内視鏡によるグレード1のBAS臨床徴候を示すイングリッシュ・ブルドッグの気管径の比較
Tracheal hypoplasia is commonly seen in English Bulldogs affected with brachycephalic airway syndrome. Previously published diagnostic criteria for tracheal hypoplasia in this breed have been a radiographic tracheal diameter:tracheal inlet ratio (TD:TI) < 0.12 or a tracheal diameter:third rib diameter ratio (TD:3R) < 2.0. Computed tomography has become increasingly used for airway evaluation, however published information is lacking regarding CT tracheal dimensions in English Bulldogs. Objectives of this prospective cross-sectional study were to describe radiographic and CT tracheal dimensions in a sample of clinically normal English Bulldogs and compare these values with tracheoscopy scores. Computed tomography (n = 40), radiography (n = 38), and tracheoscopy (n = 40) studies were performed during a single general anesthesia session for each included dog. Tracheal measurements were recorded at three locations: cervical, thoracic inlet, and thorax. Tracheal diameters were narrowest at the thoracic inlet with all techniques. Computed tomographic measurements averaged 19% greater than radiographic measurements. All included dogs had radiographic tracheal measurements greater than the previously published criteria for tracheal hypoplasia. Mean CT TD:TI was 0.26 (+/- 0.03, 0.20-0.33), and mean CT TT:3R was 2.27 (+/- 0.24, 1.71-2.74). Radiographic TD:TI and CT TD:TI were significantly correlated (P = 0.00); however radiographic TT:3R and CT TT:3R were not significantly correlated (P = 0.25). Tracheoscopy identified hypoplastic changes in all dogs and tracheoscopy scores were not correlated with CT or radiography diameter measurements. In conclusion, findings indicated that some CT and radiographic tracheal diameter measurements were comparable in English Bulldogs however diameters for both imaging techniques were not comparable with tracheoscopy scores.
コメント:短頭種における気管低形成の診断においてレントゲンとCTは同等、CTと比較して気管支鏡がより有用である可能性を示唆する論文(ダクタリ動物病院 東京医療センター 田畑達彦-2019.2.3)
Vilaplana Grosso F, Haar GT, Boroffka SA. Gender, Weight, and Age Effects on Prevalence of Caudal Aberrant Nasal Turbinates in Clinically Healthy English Bulldogs: A Computed Tomographic Study and Classification. Vet Radiol Ultrasound 2015;56:486-493.
健常なイングリッシュブルドッグにおける尾側鼻甲介異常所見の有病率に対する性別、体重、年齢の影響:CT検査での調査と分類
English Bulldogs have been reported to demonstrate abnormal growth and development of the nasal turbinates, which contribute to an increase in airway resistance and hence clinical signs of brachycephalic airway syndrome. The purpose of this prospective, cross-sectional study was to assess the prevalence and severity of caudal aberrant turbinate protrusion via CT studies of English Bulldogs with, according to the owners, none or minimal clinical signs of brachycephalic airway syndrome. An additional objective was to propose a classification scheme for describing the degree of caudal aberrant turbinate protrusion in English Bulldogs and to apply this scheme in assessing the effect of gender, weight, and age on prevalence and severity of turbinate protrusion. The nasal cavities of 40 clinically healthy English Bulldogs were examined. The prevalence of caudal aberrant turbinates in this group was 100%. Using our proposed classification scheme, Grade 1 (minimal) was detected in 7 of 40 (17.5%), Grade 2 (mild) in 28 of 40 (70%), and Grade 3 (moderate) in 5 of 40 (12.5%) English Bulldogs. No significant effect of gender, weight, and age on degree of protrusion was found. In conclusion, this study identified minimal to moderate protrusion of caudal aberrant turbinates toward the nasopharynx in all the sampled English Bulldogs, despite the absence of clinical signs of brachycephalic airway syndrome.
コメント:イングリッシュブルドッグにおける尾側鼻甲介の異常所見の有病率と重症度分類を、CTを用いて検討した論文。異常所見に対する性別、体重、年齢の影響は認められなかった(ダクタリ動物病院 東京医療センター 田畑達彦-2019.2.3)。
Haimel G, Dupre G. Brachycephalic airway syndrome: a comparative study between pugs and French bulldogs. J Small Anim Pract 2015;56:714-719.
短頭種気道症候群:パグとフレンチブルの比較研究
OBJECTIVE: To compare clinical features of brachycephalic airway syndrome and long-term surgical outcomes between pugs and French bulldogs and evaluate the influence of laryngeal collapse.
METHODS: This retrospective study included 72 dogs that underwent wedge rhinoplasty and folded flap palatoplasty for brachycephalic airway syndrome. Epidemiological data, clinical signs, postoperative complications and owners’ responses to a questionnaire at least six months after surgery were compared between pugs and French bulldogs. Spearman’s rank correlation tests were used for associating laryngeal collapse with age and respiratory signs before and after surgery.
RESULTS: On the basis of the results of the owners’ questionnaires (available in 52/72 dogs), French bulldogs presented with lower activity levels and more severe digestive signs than pugs. Owners perceived clinical improvement in 88 . 5% of all dogs. The grades of respiratory and digestive signs were not different between the breeds in the long-term follow-up, and the grade of laryngeal collapse did not influence the grade of respiratory signs or surgical outcome.
CLINICAL SIGNIFICANCE: Surgical treatment resulted in improved clinical signs in pugs and French bulldogs with brachycephalic airway syndrome, with a high owner satisfaction rate. There were no correlations between the severity of laryngeal collapse and overall respiratory signs or prognosis.
コメント:外鼻孔狭窄・軟口蓋過長整復術を行ったフレンチ・ブルドッグとパグ72頭について比較した後ろ向き研究。両犬種とも術後経過はおおむね良好で、オーナーの満足度も高かった。喉頭虚脱の重症度は、臨床症状や予後と相関が認められなかった(まるふく動物病院 福田大介-2018.12.20)。
Packer RM, Hendricks A, Tivers MS, Burn CC. Impact of Facial Conformation on Canine Health: Brachycephalic Obstructive Airway Syndrome. PLoS One. 2015 Oct 28;10(10):e0137496.(Free full text)
短頭種気道閉塞症候群(BOAS)-頭蓋構造が犬の健康に与える影響
The domestic dog may be the most morphologically diverse terrestrial mammalian species known to man; pedigree dogs are artificially selected for extreme aesthetics dictated by formal Breed Standards, and breed-related disorders linked to conformation are ubiquitous and diverse. Brachycephaly–foreshortening of the facial skeleton–is a discrete mutation that has been selected for in many popular dog breeds e.g. the Bulldog, Pug, and French Bulldog. A chronic, debilitating respiratory syndrome, whereby soft tissue blocks the airways, predominantly affects dogs with this conformation, and thus is labelled Brachycephalic Obstructive Airway Syndrome (BOAS). Despite the name of the syndrome, scientific evidence quantitatively linking brachycephaly with BOAS is lacking, but it could aid efforts to select for healthier conformations. Here we show, in (1) an exploratory study of 700 dogs of diverse breeds and conformations, and (2) a confirmatory study of 154 brachycephalic dogs, that BOAS risk increases sharply in a non-linear manner as relative muzzle length shortens. BOAS only occurred in dogs whose muzzles comprised less than half their cranial lengths. Thicker neck girths also increased BOAS risk in both populations: a risk factor for human sleep apnoea and not previously realised in dogs; and obesity was found to further increase BOAS risk. This study provides evidence that breeding for brachycephaly leads to an increased risk of BOAS in dogs, with risk increasing as the morphology becomes more exaggerated. As such, dog breeders and buyers should be aware of this risk when selecting dogs, and breeding organisations should actively discourage exaggeration of this high-risk conformation in breed standards and the show ring.
コメント:解剖学的な構造によって特徴づけられるBASは定量的な診断指標がない。今回、回顧的な検討により、マズル長が短縮する程にBAS発症のリスクが増加すること、BASは頭蓋長の半分以下のマズル長の犬のみで発症すること、頚囲の増大や肥満がBASの発症リスクを増加させることを発見した(ダクタリ動物病院 東京医療センター 田畑達彦-2018.11.29)。
Packer RM, Tivers MS. Strategies for the management and prevention of conformation-related respiratory disorders in brachycephalic dogs. Vet Med(Auckl). 2015 Jun 4;6:219-232. (Free full text)
短頭犬種における構造異常関連呼吸器障害の管理や予防法について
Brachycephalic (short-muzzled) dogs are increasingly popular pets worldwide, with marked increases in registrations of breeds such as the Pug and French Bulldog over the past decade in the UK. Despite their popularity, many brachycephalic breeds are affected by an early-onset, lifelong respiratory disorder, brachycephalic obstructive airway syndrome (BOAS). This disorder arises due to a mismatch in the proportions of the skull and the soft tissues held within the nose and pharynx, resulting in obstruction of the airway during respiration. Increased airway resistance encourages secondary changes such as eversion of the laryngeal saccules and collapse of the larynx. Clinical signs of BOAS are often early onset and chronic, including dyspnea, exercise intolerance, heat intolerance, and abnormal and increased respiratory noise. Episodes of severe dyspnea can also occur, leading to cyanosis, syncope, and death. BOAS may have a severe impact upon the welfare of affected dogs, compromising their ability to exercise, play, eat, and sleep. Although a well-described condition, with surgical treatments for the palliation of this disorder published since the 1920s, many dogs still experience airway restrictions postsurgically and a compromised quality of life. In addition, the prevalence of this disorder does not appear to have substantially reduced in this time, and may have increased. Ultimately, strategies to improve the breeding of these dogs to prevent BOAS are required to improve brachycephalic health and welfare. Recent studies have revealed conformational risk factors associated with BOAS, such as short muzzles and thick necks, which should be discouraged to avoid perpetuating this serious disorder. Positive changes to brachycephalic health may be impeded by a perception of BOAS being “normal for the breed”. This perception must be avoided by owners, breeders, and vets alike to prevent undertreatment of individuals and the perpetuation of this serious disorder to future generations of dogs.
コメント:短頭種の飼養頭数は増加しており、これらの犬種で認められる頭蓋骨と軟部組織比率のミスマッチによって生じるBASは、気道抵抗を上昇させることで喉頭小嚢の反転や喉頭虚脱、ひいてはチアノーゼや失神、死を引き起こしうる。BASに対する外科的治療は1920年代頃より文献が認められるが、いまだに術後の気流制限や不完全なQOLを経験している短頭種は多い。さらに、その罹患率は減るどころか、おそらく増加している。’その犬種では普通の構造である’という感覚が短頭種のQOLや健康を制限している(ダクタリ動物病院 東京医療センター 田畑達彦-2018.11.29)。
2014
Caccamo R, Buracco P, La Rosa G, et al. Glottic and skull indices in canine brachycephalic airway obstructive syndrome. BMC Vet Res 2014;10:12.
犬のBAOS3犬種間における声門および頭蓋形態
BACKGROUND: Forty dogs presented for brachycephalic airway obstructive syndrome with laryngeal collapse not over 1st degree (saccule eversion) underwent glottis endoscopic and radiographic skull measurements before surgery. Fifteen Pugs, fifteen French and ten English Bulldogs were included. The goals were prospectively to compare three common brachycephalic breeds for anatomical differences regarding glottis and skull measurements, and to assess if any correlation between glottis and skull measurements was present. Linear measurements were used to obtain glottis and skull indices. Correlations between glottis and skull indices and glottic measurements were evaluated. Finally, glottis indices were compared among the three breeds. RESULTS: No correlation was found for glottis and skull indices. The glottic index differed among the three breeds (smaller in Pugs and higher in English Bulldogs), ultimately representing a morphologic indicator of the different larynx shape in the three breeds (more rounded in English Bulldogs, more elliptical in Pugs and in-between in French Bulldogs). CONCLUSIONS: The lack of correlation between skull/glottic indices does not support skull morphology as predictor of glottic morphology. As Pugs had the lowest glottic index, it may be speculated that Pugs’ original narrow glottic width may predispose to further progressive respiratory deterioration more easily than in the other two breeds.
コメント:3つの短頭種間における声門および頭蓋の差異を比較した論文。残念ながら有意に相関する指標は得られなかったが、声門の形態がイングリッシュブルドッグでより円形、パグおよびフレンチブルドッグで楕円形であることが示された(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Ingman J, Naslund V, Hansson K. Comparison between tracheal ratio methods used by three observers at three occasions in English Bulldogs. Acta Vet Scand 2014;56:79.
doi: 10.1186/s13028-014-0079-6
イングリッシュブルドッグの気管低形成のレントゲン上の診断基準に対する3人の観察者間誤差
BACKGROUND: Tracheal hypoplasia is a congenital condition described in mainly brachycephalic breeds and is one component of the brachycephalic obstructive airway syndrome (BOAS). Two radiographic methods have been described to evaluate the dimensions of the tracheal diameter in dogs and to distinguish between hypoplastic and non-hypoplastic tracheas: the tracheal lumen diameter to thoracic inlet distance ratio (TD/TI) and the ratio between the thoracic tracheal luminal diameter and the width of the proximal third of the third rib (TT/3R). The purpose of this study was to compare these two published radiographic methods between observers, different measuring occasions and to investigate the effect on classification of dogs as having hypoplastic or non-hypoplastic tracheas using four previously published mean ratios as cut-offs (<0.11, <0.127 and <0.144 for the TD/TI and <2.0 for the TT/3R method). Three observers evaluated right and left lateral recumbent radiographs from 56 adult English Bulldogs independently on three different occasions. TD/TI and TT/3R ratios were calculated and correlated between measuring occasions. Kappa, observed, positive, and negative agreements were calculated between observers and measuring occasions. Number of hypoplastic and non-hypoplastic dogs for each method and occasion was determined using <0.11, <0.127 and <0.144 as cut-offs for TD/TI and <2.0 for TT/3R. RESULTS: Intraobserver agreement varied with kappa between 0.45-0.94 for the TD/TI and 0.20-0.86 for the TT/3R method. Interobserver kappa varied between 0.27-0.70 for the TD/TI method and between 0.05-0.57 for the TT/3R method. There was poor agreement in classifying English Bulldogs as tracheal hypoplastic or non-hypoplastic, depending on measuring method, cut-off value and observer. CONCLUSIONS: The diagnostic value of both the TD/TI and TT/3R methods with such poor agreement is questionable, and significantly impacts their reliability for both clinical evaluation of dogs and use in health screening programs.
コメント:イングリッシュブルドッグの気管低形成のレントゲン上の診断性能検査に関する論文。従来の2種類のレントゲン指標を用いて観察者間誤差を検討した結果、変動が激しく、従来の指標の有用性に疑問を投げかけている(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Schuenemann R, Oechtering GU. Inside the brachycephalic nose: intranasal mucosal contact points. J Am Anim Hosp Assoc 2014;50:149-158.
短頭種の鼻の内部:鼻腔内粘膜の接触点
The purpose of this study was to evaluate the prevalence of intranasal mucosal contact points in brachycephalic and normocephalic dogs. In total, 82 brachycephalic dogs (42 pugs and 40 French bulldogs) were evaluated by rhinoscopy for their intranasal mucosal contact and 25 normocephalic dogs were evaluated as a control group. Of those, 162 brachycephalic nasal cavities were evaluable and 140 had contact between intranasal structures (87%). Intraconchal and septoconchal mucosal contact points were the most commonly detected sites of contact. French bulldogs had a significantly higher prevalence of mucosal contact and had 3 mean contact points compared with 1.7 mean contact points per nasal cavity in pugs. Septal deviations were present in 62% of brachycephalic dogs. In the control group, mucosal contact points were present in only 7 of 50 nasal cavities (14%), and septal deviations occurred in 16% of those cases. Contact point average was 0.1 in large and 0.3 in small normocephalic dogs. Intranasal mucosal contact was identified as a common and previously unreported problem in brachycephalic dogs. Numerous contact points reduce the lumen of the intranasal passageways and indicate potential intranasal obstruction. Affected dogs might benefit from removal of obstructing conchae, potentially using laser-assisted turbinectomy.
コメント:鼻腔吻側からの鼻鏡検査所見。鼻腔内粘膜の接触は、正常な頭蓋をもつ犬種より短頭犬種で有意に多くみられる。フレンチブルドックは、パグに比べて鼻腔内粘膜の高い接触率を示した。多くの短頭種で直ヒダの肥大がみられたが、それにより、バグではしばしば鼻中隔と翼ヒダに接触し鼻前庭で閉塞する一方、鼻腔内はフレンチブルドックより閉塞していないようである(いいのペットクリニック 飯野亮太-2020.12.29)。
2013
Johnson LR, Mayhew PD, Steffey MA, et al. Upper airway obstruction in Norwich Terriers: 16 cases. J Vet Intern Med 2013;27:1409-1415.
ノーリッチテリアにおける上気道閉塞:16症例
BACKGROUND: Norwich Terriers have grown increasingly popular as show animals and pets, and awareness of respiratory problems within the breed is growing. OBJECTIVE: To describe components of obstructive upper airway syndrome in a nonbrachycephalic terrier breed. ANIMALS: Sixteen Norwich Terriers; 12 with and 4 without clinical signs of respiratory disease. METHODS: Prospective case series. Physical and laryngoscopic examinations were performed by 1 investigator in all dogs. Medical and surgical interventions were summarized and results of follow-up examination or owner reports were recorded. RESULTS: The study population was comprised of 9 females (6 intact) and 7 males (5 intact). Median age was 3.0 years (range, 0.5-11 years). Of 12 dogs presented for a respiratory complaint, physical examination was normal in 4 dogs. Laryngoscopic examination was abnormal in 11/12 dogs with redundant supra-arytenoid folds, laryngeal collapse, everted laryngeal saccules, and a narrowed laryngeal opening in most. Of 4 dogs lacking clinical signs, all had normal physical examination; however, 3/4 dogs had similar appearance of the larynx to dogs with clinical signs. Response to surgical intervention was minimal to moderate in all dogs. CONCLUSIONS AND CLINICAL IMPORTANCE: Norwich Terriers suffer from an upper airway obstructive syndrome that differs from that encountered in brachycephalic breeds. Affected dogs are difficult to identify without laryngoscopic examination because of the lack of clinical signs and abnormalities in physical examination findings, despite severe airway obstruction. Care is warranted when anesthetizing Norwich Terriers because of the small size of the laryngeal opening.
コメント1:ノーリッチテリアは、短頭犬種とは異なる上気道閉塞症候群(余剰な披裂軟骨上ヒダ、喉頭虚脱、反転喉頭小嚢、狭窄した喉頭開口部)に罹患していることがあり、重度の狭窄にもかかわらず臨床徴候や身体検査に異常がないことがある(いいのペットクリニック 飯野亮太-181228)。
コメント2:ノーリッチテリアの喉頭異常についての論文。披裂軟骨の粘膜ヒダ過長、喉頭虚脱、反転喉頭小嚢および喉頭開口の狭小化が認められ、これらは臨床症状を伴わず喉頭鏡で発覚することが多い(ダクタリ動物病院東京医療センター 田畑達彦-190502)。
2012
Hoareau GL, Jourdan G, Mellema M, et al. Evaluation of arterial blood gases and arterial blood pressures in brachycephalic dogs. J Vet Intern Med 2012;26:897-904.
短頭犬種の動脈血ガスと血圧の評価
BACKGROUND: Brachycephalic dogs (BD) are prone to congenital upper airway obstruction (brachycephalic syndrome, BS). In humans suffering from sleep apnea, upper airway obstruction is known to cause hypertension. There is no information regarding the influence of BS in dogs on cardiorespiratory physiology.
HYPOTHESIS: BD are prone to lower P(a) O(2), higher P(a) CO (2), and hypertension compared with meso- or dolicocephalic dogs (MDD). ANIMALS: Eleven BD and 11 MDD.
METHODS: After a questionnaire was completed by the owner, a physical examination was performed. Height and thoracic circumferences were measured. Arterial blood gases, electrolyte concentrations, and packed cell volume (PCV) were measured. Systolic (SAP), mean (MAP), and diastolic (DAP) arterial blood pressure recordings were performed.
RESULTS: A total of 7 French and 4 English bulldogs met the inclusion criteria. The control group consisted in 6 Beagles, 2 mixed breed dogs, 1 Staffordshire Bull Terrier, 1 Parson Russell Terrier, and 1 Australian Cattle Dog. Statistically, BD had lower P(a) O(2), higher P(a) CO2, and higher PCV when compared with controls (86.2 +/- 15.9 versus 100.2 +/- 12.6 mmHg, P = .017; 36.3 +/- 4.6 versus 32.7 +/- 2.6 mmHg, P = .019; 48.2 +/- 3.5 versus 44.2 +/- 5.4%, P = .026, respectively). Also, they had significantly higher SAP (177.6 +/- 25.0 versus 153.5 +/- 21.7 mmHg, P = .013), MAP (123.3 +/- 17.1 versus 108.3 +/- 12.2 mmHg, P = .014), and DAP (95.3 +/- 19.2 versus 83.0 +/- 11.5 mmHg, P = .042). BD with a P(a) CO (2) >35 mmHg were significantly older than those with a P(a) CO (2) </=35 mmHg (58 +/- 16 and 30 +/- 11 months, P = .004).
CONCLUSION: Results of this study suggest that some BD are prone to lower P(a) O(2), higher P(a) CO (2), and hypertension when compared with MDD. Age may be a contributing factor.
コメント1:短頭種では、非短頭種に比べ低O2血症、高CO2血症、高血圧が認められることを示し、それらの機序を考察した文献(まるふく動物病院 福田大介-2019.1.5)。
コメント2:短頭種と中長頭種間で血液ガス、血圧を比較した論文。短頭種において有意にPaO2は低く、PaCO2および血圧は有意に高かった。また、年齢で比較した時、短頭種におけるPaO2の低下は高齢で有意に低かった(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
White RN. Surgical management of laryngeal collapse associated with brachycephalic airway obstruction syndrome in dogs. J Small Anim Pract 2012;53:44-50.
短頭種気道閉塞症候群の犬に関連した喉頭虚脱の外科的治療
OBJECTIVE: To describe the use of cricoarytenoid lateralisation combined with thyroarytenoid caudo- lateralisation (arytenoid laryngoplasty) for the management of stage II and III laryngeal collapse in dogs. METHODS: A retrospective study of a consecutive series of 12 dogs suffering from life-threatening stage II or III laryngeal collapse associated with brachycephalic airway obstruction syndrome. RESULTS: Pre-operatively, either stage II collapse (2/12) or stage III collapse (10/12) was confirmed on visual examination. In all cases, a left-sided arytenoid laryngoplasty was performed. Two dogs were euthanased postoperatively as a result of persistent life-threatening respiratory compromise. The procedure resulted in subjective enlargement of the rima glottidis and an associated improvement in respiratory function in the remaining 10 dogs. Follow-up, long-term outcome (median, 3.5 years) in these dogs indicated that all owners considered that the surgery had resulted in marked improvements in their dog’s respiratory function, tolerance to exercise, and quality of life. CLINICAL SIGNIFICANCE: Combined cricoarytenoid and thyroarytenoid caudo-lateralisation may be a useful procedure for treatment of stage II and III laryngeal collapse in the dog.
コメント:短頭種気道閉塞症候群に関連したステージⅡもしくはⅢの喉頭虚脱を呈する犬12頭に対して輪状-披裂軟骨側方化術に甲状-披裂軟骨尾側‐側方化術を組み合わせた外科的治療を実施した後ろ向き研究。10頭においては、軽度のBAOS症状は残存したものの全例で呼吸状態は改善し長期予後も良好。術後に呼吸困難により安楽死となった1例では輪状軟骨の脆弱性による喉頭虚脱が疑われた(いいのペットクリニック 飯野亮太-2019.3.3)。
2011
Grand JG, Bureau S. Structural characteristics of the soft palate and meatus nasopharyngeus in brachycephalic and non-brachycephalic dogs analysed by CT. J Small Anim Pract 2011;52:232-239.
CTを用いた短頭種および非短頭種の軟口蓋および鼻咽頭領域の構造比較
OBJECTIVES: The goal of this study was to compare the dimensions of the soft palate and cross-sectional area of the meatus nasopharyngeus in non-brachycephalic dogs and brachycephalic dogs with different degrees of severity of brachycephalic airway syndrome using computed tomography. METHODS: A total of 26 brachycephalic dogs that had at least one of four major symptoms of snoring, inspiratory effort, stress or exercise intolerance, and syncope were included in this prospective study. The dogs were grouped by the frequency of different clinical signs into absent/minimal brachycephalic airway syndrome and severe brachycephalic airway syndrome groups. Five non-brachycephalic dogs were studied as control animals. All dogs underwent pharyngeal area computed tomography. Seven measurements were made on the transverse and midsagittal reconstructions. All parameters were compared between controls, absent/minimal and severe brachycephalic airway syndrome groups. RESULTS: The dogs with severe brachycephalic airway syndrome had significantly thicker soft palates compared to absent/minimal brachycephalic airway syndrome (P<0.05) and control (P<0.05) dogs. There were no significant differences among groups with regard to the length of the soft palate or the cross-sectional area of the airway at the level of the meatus nasopharyngeus. CLINICAL RELEVANCE: These results support the thickening of the soft palate as a component of severe brachycephalic airway syndrome. Further studies are required to confirm the association between this anatomical characteristic and functional impairment.
コメント:CTを用いた短頭種および非短頭種の軟口蓋および鼻咽頭領域の大きさを比較した論文。重度の短頭種気道症候群の群では他の群と比較して、鼻咽頭レベルの横断径や軟口蓋の長さは同等だが軟口蓋の厚さは有意に大きかった(ダクタリ動物病院東京医療センター 田畑達彦-190502)。
Senn D, Sigrist N, Forterre F, et al. Retrospective evaluation of postoperative nasotracheal tubes for oxygen supplementation in dogs following surgery for brachycephalic syndrome: 36 cases (2003-2007). J Vet Emerg Crit Care (San Antonio) 2011;21:261-267.
短頭種症候群の犬における術後の経鼻気管チューブを介した酸素投与に対する後ろ向き評価
OBJECTIVE: To assess the utility of nasotracheal tubes in postoperative oxygen supplementation in dogs following corrective surgery for brachycephalic syndrome. DESIGN: Retrospective study 2003-2007. SETTING: University teaching hospital. ANIMALS: Thirty-six client-owned dogs that underwent corrective surgery for brachycephalic syndrome. INTERVENTIONS: None. MEASUREMENTS AND MAIN RESULTS: Medical records were reviewed for animals that underwent surgical interventions for brachycephalic syndrome including palatoplasty, ventriculectomy, and rhinoplasty. Data collected included signalment, presenting complaints, analgesic and surgical interventions, type of supplemental oxygen therapy, complications and mortality occurring during hospitalization. A nasotracheal tube (NTT) was placed in 20 dogs at the end of surgery; 16 dogs received other forms of oxygen supplementation (8) or no oxygen supplementation (8) during recovery. The total number of postoperative complications was similar in both groups (8/20 dogs with NTTs and 7/16 in those without NTTs). However, respiratory distress was observed in 5 dogs without NTTs but was not observed in any dog while an NTT was in place. One dog in each group died postoperatively. CONCLUSION: Placement of an NTT was found to be easy and may offer benefit in dogs with brachycephalic syndrome as a noninvasive means of delivering oxygen. The use of NTT may minimize severe postoperative morbidity, in particular by reducing postoperative respiratory distress.
コメント:短頭種気道症候群である様々な犬種に対して、外科的整復の術後に経鼻気管チューブを設置した後ろ向き研究。全例でチューブ設置とともに不安緩和と鎮咳目的でオピオイドを同時投与。各グループの術前の呼吸状態のグレード分類などは明記されず。チューブ設置例では4例で咳、吐き戻し、嘔吐で設置断念。チューブ不設置例での呼吸困難2例は、気管切開チューブの位置異常(いいのペットクリニック 飯野亮太-2019.3.3)。
2006〜2010
Findji L, Dupre G. Folded flap palatoplasty for treatment of elongated soft palates in 55 dogs. Vet Med Austria 2008;95:56-63.
軟口蓋過長の犬55頭の治療に対する折り畳み弁口蓋形成術
It was the aim of the present study to evaluate the safety and efficacy of the folded flap palatoplasty (FFP), a new surgical technique addressing all components of the respiratory obstruction caused by elongated soft palates, and to evaluate the clinical outcomes associated with it. Medical records (2004-2005) of all dogs which underwent a FFP were reviewed and included in the study. Recorded information included breed, gender, age, body mass, duration of hospitalisation, and presence or absence of postoperative tracheostomy. Respiratory grading scores (1-3) were used to record the severity of the disease, before and after surgery, and at a minimum follow-up time of 180 days by detailed telephone interviews with the owners. No intraoperative complications were encountered. A temporary tracheostomy was performed in 6 cases (10.9.%). 2 dogs died postoperatively from tracheostomy complications and unknown cause after unremarkable recovery, respectively.Follow-up (379 ± 142 days) could be obtained for 40 dogs. 39 dogs (97.5 %) showed improvement of respiratory clinical signs after surgery. Improvement of respiratory clinical signs was observed within 15 days after surgery in 85 % of the cases. The FFP can be recommended as a safe and efficient technique, particularly valuable for excessively thick elongated soft palates.
コメント1:軟口蓋を短縮および減量する、折り畳み弁口蓋形成術(FFP)は、術後に呼吸器症状の評価スコアを有意に改善させた(いいのペットクリニック 飯野亮太-2020.6.22)。
BASの臨床評価は、Poncet CM, Dupre GP, Freiche VG, et al. Prevalence of gastrointestinal tract lesions in 73 brachycephalic dogs with upper respiratory syndrome. J Small Anim Pract 2005;46:273-279.の分類(いびき、吸気努力、運動不耐性、失神の各呼吸器症状の頻度からグレード1-3と設定)を用いている。
Poncet CM, Dupre GP, Freiche VG, et al. Long-term results of upper respiratory syndrome surgery and gastrointestinal tract medical treatment in 51 brachycephalic dogs. J Small Anim Pract 2006;47:137-142.
短頭種犬51頭における上部呼吸器症候群手術と胃腸管内科治療の長期結果
OBJECTIVES: After a first clinical study showing a high prevalence of gastrointestinal tract diseases in brachycephalic dogs presented for upper respiratory syndrome, a prospective study was performed to determine the influence of medical treatment for gastrointestinal tract disorders associated with upper respiratory syndrome surgery. METHODS: The gastrointestinal tract and respiratory disorders of 61 brachycephalic dogs presented for upper respiratory syndrome were evaluated. Together with surgery of the upper respiratory tract, a specific gastrointestinal medical treatment was administered. A minimal follow-up of six months was required for inclusion. RESULTS: Palatoplasty with rhinoplasty was the most common surgical correction (88.5 per cent). The mortality rate in the perioperative period was 3.3 per cent. Minor complications accounted for 26.2 per cent of cases. No aspiration pneumonia was encountered. A sufficient follow-up was obtained in 51 dogs. The improvement was judged by the owners as excellent or good in 88.3 per cent of the respiratory disorders and in 91.4 per cent of the gastrointestinal disorders. Clinically, a statistically significant improvement was obtained for both respiratory and gastrointestinal disorders. CLINICAL SIGNIFICANCE: In comparison with other studies, digestive tract medical treatment combined with upper respiratory surgery seems to decrease the complication rate and improve the prognosis of dogs presented for upper respiratory syndrome.
コメント:上部呼吸器症状を示す短頭種犬では様々な胃腸疾患を併発していることが多く、上部呼吸器手術とともに胃腸疾患の内科治療を併用すれば、術後の死亡率や合併症を減少することができる。また、上部呼吸器手術を実施すれば、併発している胃腸疾患の改善も期待できる(いいのペットクリニック 飯野亮太-2020.5.5)。
Ginn JA, Kumar MS, McKiernan BC, et al. Nasopharyngeal turbinates in brachycephalic dogs and cats. J Am Anim Hosp Assoc 2008;44:243-249.
短頭犬種と短頭猫における鼻甲介の鼻咽頭突出
This retrospective study reports the presence and incidence of nasal turbinates in the nasopharynx (nasopharyngeal turbinates) in a population of brachycephalic dogs and cats exhibiting signs of upper respiratory disease. Medical records were reviewed for 53 brachycephalic dogs and 10 brachycephalic cats undergoing upper airway endoscopy. Nasopharyngeal turbinates were identified in 21% of brachycephalic animals, including 21% of dogs and 20% of cats. Pugs accounted for 32% of all dogs in the study population and 82% of dogs with nasopharyngeal turbinates. The presence of nasopharyngeal turbinates may play a role in upper airway obstruction in the brachycephalic airway syndrome.
コメント:短頭種における鼻甲介の鼻咽頭への突出の罹患率に関する論文。パグで最も多く32%で認められ、80%の犬で認められた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
De Lorenzi D, Bertoncello D, Drigo M. Bronchial abnormalities found in a consecutive series of 40 brachycephalic dogs. J Am Vet Med Assoc 2009;235:835-840.
連続サンプリング短頭種40例で認められた気管支の異常所見
OBJECTIVE: To detect abnormalities of the lower respiratory tract (trachea, principal bronchi, and lobar bronchi) in brachycephalic dogs by use of endoscopy, evaluate the correlation between laryngeal collapse and bronchial abnormalities, and determine whether dogs with bronchial abnormalities have a less favorable postsurgical long-term outcome following correction of brachycephalic syndrome. DESIGN: Prospective case series study. ANIMALS: 40 client-owned brachycephalic dogs with stertorous breathing and clinical signs of respiratory distress. PROCEDURES: Brachycephalic dogs anesthetized for pharyngoscopy and laryngoscopy between January 2007 and June 2008 underwent flexible bronchoscopy for systematic evaluation of the principal and lobar bronchi. For dogs that underwent surgical correction of any component of brachycephalic syndrome, owners rated surgical outcome during a follow-up telephone survey. Correlation between laryngeal collapse and bronchial abnormalities and association between bronchial abnormalities and long-term outcome were assessed. RESULTS: Pugs (n = 20), English Bulldogs (13), and French Bulldogs (7) were affected. A fixed bronchial collapse was recognized in 35 of 40 dogs with a total of 94 bronchial stenoses. Abnormalities were irregularly distributed between hemithoraces; 15 of 94 bronchial abnormalities were detected in the right bronchial system, and 79 of 94 were detected in the left. The left cranial bronchus was the most commonly affected structure, and Pugs were the most severely affected breed. Laryngeal collapse was significantly correlated with severe bronchial collapse; no significant correlation was found between severity of bronchial abnormalities and postsurgical outcome. CONCLUSIONS AND CLINICAL RELEVANCE: Bronchial collapse was a common finding in brachycephalic dogs, and long-term postsurgical outcome was not affected by bronchial stenosis.
コメント:BOASに気管支鏡を用いた観察研究。約9割の症例で気管支狭窄が認められ、罹患気管支の約9割は左側に集中していた。なかでも左頭側気管支の罹患率が高かった。また、喉頭虚脱と気管支虚脱の重症度は相関したが、気管支虚脱の重症度と術後の予後とは関連しなかった(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Fasanella FJ, Shivley JM, Wardlaw JL, et al. Brachycephalic airway obstructive syndrome in dogs: 90 cases (1991-2008). J Am Vet Med Assoc 2010;237:1048-1051.
短頭種気道症候群90例(1991-2008)
OBJECTIVE: To determine the prevalence of individual anatomic components of brachycephalic airway obstructive syndrome (BAOS), including everted tonsils, and analyze the frequency with which each component occurs with 1 or more other components of BAOS in brachycephalic dogs. DESIGN: Retrospective case series. ANIMALS: 90 dogs with BAOS. PROCEDURES: Medical records were reviewed for signalment, clinical signs at time of admission, historical and physical examination findings, BAOS components found on laryngoscopic examination of the pharynx and larynx, surgical procedures performed, and perioperative complications. RESULTS: English Bulldogs (55/90 [61%]), Pugs (19/90 [21%]), and Boston Terriers (8/90 [9%]) were the most common breeds with BAOS. The most common components of BAOS were elongated soft palate (85/90 [94%]), stenotic nares (69/90 [77%]), everted laryngeal saccules (59/90 [66%]), and everted tonsils (50/90 [56%]). Dogs most commonly had 3 or 4 components of BAOS, with the most common combination being stenotic nares, elongated soft palate, everted laryngeal saccules, and everted tonsils. Dogs with stenotic nares were significantly more likely to have everted laryngeal saccules (50/69 [72%]), and dogs with everted laryngeal saccules were significantly more likely to have everted tonsils (39/59 [66%]). Postoperative surgical complications occurred in 12% (10/83) of dogs that received corrective surgery. No specific BAOS component made dogs more likely to have complications. CONCLUSIONS AND CLINICAL RELEVANCE: The prevalence of components of BAOS in brachycephalic dogs of this study differed from that reported previously, especially for everted tonsils. Thorough examination of the pharynx and larynx is necessary for detection of BAOS components.
コメント:短頭種の気道異常の併発割合に関する論文。約95%の犬は軟口蓋過長があり、次いで外鼻腔狭窄、反転喉頭小嚢、反転扁桃?であった。これらの罹患率は過去の報告と相違なく、本研究における術後合併症は12%でみられた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Bernaerts F, Talavera J, Leemans J, et al. Description of original endoscopic findings and respiratory functional assessment using barometric whole-body plethysmography in dogs suffering from brachycephalic airway obstruction syndrome. Vet J 2010;183:95-102.
短頭種気道症候群に罹患した犬における全身プレチスモグラフィによる呼吸機能評価と気管支鏡所見
The clinical features of brachycephalic airway obstructive disease in 11 brachycephalic dogs are described in this study. The respiratory strategy was assessed before (n=11) and after (n=6) surgery using barometric whole-body plethysmography (BWBP), with the relationship between BWBP variables and the severity of the clinical signs assessed by the use of a respiratory score based on clinical, radiographic and endoscopic findings. Partial collapse of the left main bronchus was a common finding not previously described as part of the brachycephalic airway obstructive disease syndrome. Epiglottic cysts, laryngeal granulomas and nasopharyngeal turbinates in English Bulldogs were other previously unreported findings. No significant correlation between the respiratory score and any of the BWBP variables was detected. Compared to healthy dogs, brachycephalic dogs had a significantly lower Te/Ti ratio (expiratory time over inspiratory time), peak inspiratory flow (PIF) per kg bodyweight (BW), significantly higher peak expiratory flow (PEF) per kgBW, PEF/PIF, and enhanced pause. These variations are compatible with upper airway obstructions primarily in the extrathoracic airways. Following surgery, a significant decrease in PEF/PIF was detected. The study showed that BWBP could be used to characterise the respiratory strategy in brachycephalic dogs before and after surgery.
コメント:内視鏡やプレチスモグラフィを用いてブルドッグにおけるBOASの特徴づけを試みた論文。左主気管支の虚脱が多くで認められた。また、非短頭種と比べて、短頭種ではTe/Ti ratioと吸気のピークフローが有意に低く、呼気のピークフローが有意に高くなっていた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
Torrez CV, Hunt GB. Results of surgical correction of abnormalities associated with brachycephalic airway obstruction syndrome in dogs in Australia. J Small Anim Pract 2006;47:150-154.
オーストラリアにおける短頭種気道症候群に関する上気道疾患の外科整復の結果
OBJECTIVES: To describe clinical features of brachycephalic airway obstructive disease in dogs, the incidence of laryngeal collapse in dogs presenting for surgery and the outcome after surgery in dogs with laryngeal collapse. METHODS: Basic clinical details were reviewed retrospectively in 73 dogs. Presence of laryngeal collapse and short-term outcomes after surgery were determined for 64 dogs with complete medical records. Long-term outcomes were reviewed for 46 dogs by telephone survey between 19 and 77 months following surgery. RESULTS: Stenotic nares were present in 31 dogs (42.5 per cent), elongated soft palate in 63 (86.3 per cent) and everted laryngeal saccules in 43 (58.9 per cent). The most common breeds were the pug (19 dogs, 26 per cent), Cavalier King Charles spaniel (15 dogs, 20.5 per cent), British bulldog (14 dogs, 19.2 per cent) and Staffordshire bull terrier (4 dogs, 5.5 per cent). Laryngeal collapse was present in 34 of 64 (53 per cent) dogs. No dogs died perioperatively and only one dog was euthanased as a result of its respiratory disease three years after surgery. Telephone interviews indicated that 26 dogs (56.5 per cent) were much improved after surgery, 15 (32.6 per cent) had some improvement and 5 (10.9 per cent) showed no improvement. Signs that persisted after surgery were snoring during sleep (34 dogs, 73.9 per cent), stertor/stridor while conscious (23 dogs, 50 per cent), excessive panting (13 dogs, 28.3 per cent) and dyspnoea (10 dogs, 21.7 per cent). Long-term outcome was considered good, even in dogs with laryngeal collapse. CLINICAL SIGNIFICANCE: Laryngeal collapse is relatively common in dogs presented for surgical correction of brachycephalic airway obstructive disease. Dogs with severe laryngeal collapse often respond well to surgery. Clinical signs rarely resolve completely following surgery.
コメント:BOASを外科的に治療した転帰に関する論文。この研究において最も有病率の高い疾患は軟口蓋過長であり、喉頭虚脱の合併も多く認められた。周術期死亡はなく、約50%の症例において術後の長期予後も良好であったが、睡眠時のいびきやストライダーは残存する傾向にあった(ダクタリ動物病院 東京医療センター 田畑達彦-2019.2.3)。
Riecks TW, Birchard SJ, Stephens JA. Surgical correction of brachycephalic syndrome in dogs: 62 cases (1991-2004). J Am Vet Med Assoc 2007;230:1324-1328.
短頭種気道症候群の整復術62例(1991−2004)の転帰
OBJECTIVE: To assess results of surgical correction of brachycephalic syndrome (including stenotic nares, elongated soft palate, and everted laryngeal saccules) in dogs and determine whether dogs with hypoplastic trachea have a less favorable long-term outcome. DESIGN: Retrospective case series. ANIMALS: 62 dogs with brachycephalic syndrome. PROCEDURES: Medical records from 1991 to 2004 were reviewed for information regarding signalment, clinical signs, diagnosis, surgery, and long-term outcome. Surgical outcome was rated by owners as excellent, good, fair, or poor. Common abnormalities, treatments, and long-term outcomes among the 62 dogs were assessed. RESULTS: Predominantly affected breeds included English Bulldog, Pug, and Boston Terrier. Elongated soft palate was the most common abnormality (54/62 [87.1%] dogs); the most common combination of abnormalities was elongated soft palate, stenotic nares, and everted saccules (16/62 [25.8%] dogs). The English Bulldog was the most common breed for all abnormalities, including elongated soft palate (27/54 [50%] dogs), stenotic nares (14/36 [38.9%] dogs), everted saccules (20/36 [55.6%] dogs), hypoplastic trachea (7/13 [53.9%] dogs), and laryngeal collapse (2/5 [40%]). No dogs had everted saccules alone. Outcome did not differ between dogs under-going staphylectomy by use of laser or scissor resection. Follow-up information was obtained for 34 dogs; 16 (47.1%) had an excellent outcome, and 16 (47.1%) had a good outcome. Overall treatment success rate was 94.2%, and overall mortality rate was 3.2%. CONCLUSIONS AND CLINICAL RELEVANCE: Surgical treatment of brachycephalic syndrome in dogs appeared to be associated with a favorable long-term outcome, regardless of age, breed, specific diagnoses, or number and combinations of diagnoses.
コメント:BOASを外科的に治療した転帰に関する論文。この研究において最も有病率の高い疾患は軟口蓋過長であり、イングリッシュブルドッグは多くの種類のBOAS関連疾患を有する傾向にあった。また、軟口蓋過長に対する手術後の症状の改善率は約95%であった(ダクタリ動物病院 東京医療センター 田畑達彦-2019.2.3)。
2001〜2005
Poncet CM, Dupre GP, Freiche VG, et al. Prevalence of gastrointestinal tract lesions in 73 brachycephalic dogs with upper respiratory syndrome. J Small Anim Pract 2005;46:273-279.
短頭種気道症候群73例における消化器疾患の有病率
OBJECTIVES: To determine the prevalence of gastrointestinal tract lesions in brachycephalic dogs with upper respiratory tract disease. METHODS: The gastrointestinal tract and respiratory disorders of 73 brachycephalic dogs presented with upper respiratory signs were evaluated. Clinical signs and endoscopic and histological anomalies of the upper digestive tract were analysed. RESULTS: A very high prevalence of gastrointestinal tract problems in brachycephalic dogs presented with upper respiratory problems was observed clinically, endoscopically and histologically. Endoscopic anomalies of the upper digestive tract were present even in dogs without digestive clinical signs. Furthermore, histological evaluation of the digestive tract sometimes showed inflammatory lesions not macroscopically visible at endoscopy. Statistical analysis showed a relationship between the severity of the respiratory and digestive signs. This was significant in French bulldogs, males and heavy brachycephalic dogs. CLINICAL SIGNIFICANCE: These observations show a correlation between upper respiratory and gastrointestinal tract problems in brachycephalic breeds with upper respiratory disease. Surgical treatment of respiratory disease could improve the digestive clinical signs, and/or gastro-oesophageal medical treatment could improve the outcome for surgically treated brachycephalic dogs.
コメント:短頭種における消化器疾患の併発率に関する論文。消化器疾患の併発率は非常に高く、内視鏡を用いた消化管粘膜の病理検査上も炎症性疾患の有病率は高かった。また、この病理学的変化はBOASを罹患していない短頭種においても認められた(ダクタリ動物病院東京医療センター 田畑達彦-2019.3.10)。
コメント:良著。とくに咽頭気道の代償不全に関して詳細に記述しています。BASを語るのなら本書を少なくとも3回は熟読していただきたいと思います(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
2000〜
Lorinson D, Bright JM, White RAS. Brachycepharic Airway Obstruction Syndrome – A Review of 118 Cases. Canine Practice 1997;22:18-21.
短頭種気道閉塞症候群118例の調査
The medical records of 118 dogs with brachycephalic airway obstruction syndrome (BAOS) were analyzed for clinical features common to dogs presented with this disease. Questionnaires from 56 owners describing their dog’s response to surgery were studied in detail. The clinical signs ranged from mild signs such as stertous breathing and snoring to acute collapse. The mean age of all dogs presented for BAOS was 3.2 years. The breed most commonly seen was the English Bulldog (EB) followed by the Pug, Boston Terrier and the Cavalier King Charles Spaniel. Soft palate elongation was seen in 101 dogs., 56 of which had concurrent stenotic nares. Everted saccules were seen in 54 dogs. Aspiration pneumonia was diagnosed preoperaltively and the remaining 10 were postoperative events. The response to surgery in 56 dogs was classified as excellent in 17 dogs, good in 16 dogs and poor in 23. The number of EB that had a poor response to surgery was 55% compared to all other breeds combined (33%). Dogs having stenotic nares as part of the BAOS responded better than those dogs with soft palate elongation alone. Only 40% of dogs with everted saccules as part of the BAOS did well following surgery. Eight of 56 dogs undergoing surgery died postoperatively with an overall mortality rate of 14 %. Aspiration pneumonia was the cause of death in six of these dogs. Five of these were the EB breed. This represents a twofold increase in mortality rates in this breed when compared to all other breeds dying of aspiration pneumonia. Risk of aspiration pneumonia may be reduced in the EB by placing these dogs on weight-reducing diets before surgery, carefull evaluaion of esophageal function, fasting for 24 hours before surgery and the use of prokinetic agents and systemic antacids prior to surgery.
コメント:誤嚥性肺炎は118頭中15頭に認められ、このうちほとんどの犬において術後にも誤嚥性肺炎が生じた。イングリッシュ・ブルドッグでは特に成績が悪く、他犬種での成績は33%が不良とされたのに対し、55%にあたる犬で不良であった。最終的に56頭中8頭が死亡し(14%)、そのうち6頭は誤嚥性肺炎のためであった。誤嚥性肺炎で死亡した6頭のうち5頭はイングリッシュ・ブルドッグであった(犬・猫の呼吸器科 城下幸仁-2020.11.23)。
豊住頼一. 哺乳動物における嗅覚,呼吸,嚥下に関する比較解剖学的研究. 耳鼻と臨床 1979;25:29-37.
On the basis of anatomical investigations in some selected mammals and of the report by Negus and other investigations, the author discussed olfaction, respiration and deglutition from a evolutional point of view. These functions were related to anatomy and physiology of the larynx in various species. Relation between olfactory function and location of the epiglottis, changes in pattern of deglutition according to the descent of the larynx, and relation between respiration and deglutition are of spacial interest when one looks at the comprehensive mechanism of olfaction, respiration and deglutition.
コメント:犬、猫、兎、牛、馬、豚、山羊の8種各3例の喉頭の比較解剖から考察されている。本文内容より「犬は人より喉頭蓋が相対的に大きく、可動性が少ない。喉頭の機能的役割の観点から比較解剖学的考察すると、犬、猫などは嗅覚鋭敏な動物(macrosmatic animal)であり、喉頭蓋が鼻咽頭から喉頭の間の気道を確保するために軟口蓋尾側縁の上にしっかりと重なるような咽喉頭の構造を成しているためである。人は、他の動物に比べ嗅覚の重要性が減少し(microsmatic animal)、喉頭蓋が退化し、その代わりに舌の発達によって嚥下機能を発達させたり、言語を獲得した。結果として喉頭下降が生じ、軟口蓋と喉頭蓋の距離が生じるようになった(図1)。また、人では発声機能の進化のため喉頭を収縮させる喉頭固有筋が他の動物にくらべ発達し、それまでの動物の軟骨を主体とする構造から、筋成分が主体となり、特に披裂軟骨が小さくなっていった。」
さらに、本文中では、犬の舌骨喉頭蓋筋(m.hypoepiglotticus)について「犬には喉頭蓋と舌骨との間にm.hypoepiglotticusと称する小さい筋組織が観察されるが、その機能についてはいまだつまびらかでない。本筋の位置からその機能を推測すると、本筋は嚥下時、喉頭の挙上と同時に喉頭蓋を軟口蓋へわずかに反転させる作用があることが考えられている。喉頭閉鎖はまずary-epiglottic sphincterで開始され–(略)–喉頭入口部をcoverする状態になる。このとき、–(略)–その中央部がm.hypoepiglotticusによってわずかに軟口蓋側にそるような動きをみせる–(略)、犬ではとくに嚥下時にもなお鼻腔、鼻咽頭、喉頭を結ぶair streamを獲得し、十分な嗅覚を維持せんとするためにきわめて合目的な特殊な動きをする筋、m.hypoepiglotticusを保有するでのはないかと思われる。」とある。ary-epiglottic sphincterに相当する喉頭固有筋である、披裂軟骨喉頭蓋筋が犬にあるか成書を調べたが見当たらなかった。でも、嚥下時喉頭閉鎖の際、舌骨喉頭蓋筋は舌筋によって喉頭が前方に牽引されたときの喉頭蓋後傾に反する動きを調整する役割があるかもしれない。
したがって、人為的交配によって、本来の「犬」種の咽喉頭の構造から頭蓋骨を「短頭化」させたことにより、短頭犬種の軟口蓋過長/肥厚は、軟口蓋と喉頭蓋の過度の重複を形成する。本文献では、舌骨喉頭蓋筋は、嚥下時の呼吸を維持する役割があると記載されている。別文献では、犬の舌骨喉頭蓋筋は、吸気時に喉頭蓋を前方に牽引する役割があるという(Amis TC, O’Neill N, Van der Touw T, et al. Control of epiglottic position in dogs: role of negative upper airway pressure. Respir Physiol 1996;105:187-194.)。もし、本来犬では喉頭蓋の可動性が少ない構造ならば、短頭種気道症候群では気道確保維持のため、通常犬より舌骨喉頭蓋筋の負荷が大きいかもしれない。短頭種気道症候群では透視検査にて喉頭蓋の後傾をよく観察する。短頭犬種では咽頭閉塞があったり、口呼吸やパンティングが多かったりするので喉頭蓋を舌根に引き寄せる力は気道確保の上で重要な作用となる。そのとき、過剰な軟口蓋が喉頭蓋の前傾の障害にならないように咽頭拡張筋群の負荷を余儀なくされるし、また舌骨喉頭蓋筋の過剰負荷があることも推測される。舌骨喉頭蓋筋の負荷が咽頭拡張筋群の経年負荷と同様に線維化や変性を生じ不可逆的変化に至るとすれば、その段階で軟口蓋の整復だけ行なっても、喉頭蓋の後傾は残存し吸気時ストライダーが持続するかもしれない。また、犬では喉頭入口部が軟骨性(主に披裂軟骨)であるのに対し、人では筋肉性であることは、犬の後天的喉頭虚脱と同じ病態は人では生じない理由のひとつになると考えらえる。人では幼小児期の喉頭形成不全期に生じる喉頭軟化症が犬の後天的喉頭虚脱とは異なる機序で生じ、幼小児の喉頭軟化症の80%は成長とともに改善されるという(犬・猫の呼吸器科 城下幸仁-2021.1.1)。
犬などでは常に嗅覚を鋭敏に維持するため、喉頭蓋は軟口蓋の上にしっかりと重なるようになっており、喉頭蓋が発達している。一方、人では嗅覚が重要でなくなり、喉頭蓋が短くなり、軟口蓋との距離が大きくなった。豊住頼一. 哺乳動物における嗅覚,呼吸,嚥下に関する比較解剖学的研究. 耳鼻と臨床 1979;25:29-37. p30 図1より転載(耳鼻と臨床会より2021.1.5に転載許諾済み)
犬は他の動物に比べ披裂軟骨は小さいが、ヒトに比べると大きく、喉頭入口部は軟骨主体の構造をしている。ヒトは発声機能を高めるため喉頭入口部は筋肉主体となり披裂軟骨は縮小した。豊住頼一. 哺乳動物における嗅覚,呼吸,嚥下に関する比較解剖学的研究. 耳鼻と臨床 1979;25:29-37.p34 図5より転載(耳鼻と臨床会より2021.1.5に転載許諾済み)
短頭種気道症候群、症例報告
Schabbing KJ, Seaman JA. Resection and Primary Closure of Edematous Glossoepiglottic Mucosa in a Dog Causing Laryngeal Obstruction. J Am Anim Hosp Assoc 2017;53:180-184.
喉頭閉塞を生じた犬に認められた舌喉頭蓋粘膜腫脹を切除および閉鎖した1例
An approximately 22 mo old male neutered English bulldog was evaluated for acute onset of dyspnea with suspected brachycephalic obstructive airway syndrome (BOAS). Laryngoscopic exam revealed diffuse, severe edema and static displacement of redundant glossoepiglottic (GE) mucosa causing complete obstruction of the larynx and epiglottic entrapment. Static displacement of the GE mucosa was observed and determined to be the overriding component of dyspnea in this patient with BOAS. Resection and primary closure with two separate, simple continuous sutures of the GE mucosa were performed. Resection and primary closure of the GE mucosa resolved the acute onset of dyspnea in this patient. Surgical correction of the stenotic nares, elongated soft palate, and everted laryngeal saccules were performed under the same anesthetic procedure. Static displacement of the GE mucosa may occur in patients with BOAS. Surgical resection and closure of the GE mucosa resolved this patient’s dyspnea and is recommended in airway obstruction. It remains to be determined if primary closure and subsequent tensioning or scar tissue of the GE mucosa results in further complications related to restricted epiglottic movement.
コメント:BOASのブルドッグにおいて認められた舌喉頭蓋粘膜の浮腫を外科的に切除した報告(ダクタリ動物病院 東京医療センター 田畑達彦-2019.2.3)。
Sabino CV, Holowaychuk M, Bateman S. Management of acute respiratory distress syndrome in a French Bulldog using airway pressure release ventilation.J Vet Emerg Crit Care(San Antonio). 2013 Jul-Aug;23(4):447-54.
フレンチブルドッグに生じた ARDSに対し気道圧開放換気(APRV)で管理した1例
OBJECTIVE: To describe the successful clinical management of a dog with acute respiratory distress syndrome (ARDS) using airway pressure release ventilation (APRV).
CASE SUMMARY: An 18-month-old female French Bulldog was presented for routine ovariohysterectomy and correction of brachycephalic airway obstruction syndrome. Following the surgical procedures, the dog developed aspiration pneumonia and ARDS. Her clinical condition failed to improve with conventional pressure-support mechanical ventilation and she was subsequently managed with APRV. She recovered fully and exhibited no clinical or radiographic abnormalities during follow-up examinations.
NEW OR UNIQUE INFORMATION PROVIDED: This is the first reported use of APRV to manage refractory hypoxemia associated with ARDS in a dog. This alternative mode of mechanical ventilation can be considered a feasible alternative in canine patients with ARDS.
コメント:18か月雌FBの不妊およびBAS整復手術後に生じた吸引性肺炎に続発するARDSの管理において気道圧開放換気(APRV)が奏功した症例報告(ダクタリ動物病院 東京医療センター 田畑達彦-2018.11.29)
Shaw TE, Harkin KR, Nietfeld J, et al. Aortic body tumor in full-sibling English bulldogs. J Am Anim Hosp Assoc 2010;46:366-370.
イングリッシュブルドッグの同腹犬に認められた大動脈小体腫瘍の2例
A 10-year-old, neutered male English bulldog died acutely from respiratory distress after a short history of progressive dyspnea. Less than 2 months later, a spayed female full sibling of that dog died suddenly during a nail trim. An aortic body tumor was the cause of death in both dogs based on postmortem and histological examinations. A pheochromocytoma was also diagnosed in the neutered male. Neither dog had a history of brachycephalic airway syndrome, and the implication for a genetic predisposition toward the development of paraganglioma is discussed. This is the first case report of aortic body tumors in sibling dogs, although the condition may not be an uncommon phenomenon.
コメント:大動脈小体腫瘍により別々の時期に急死した2頭のイングリッシュブルドッグ(同腹仔)に関するケースレポート(ダクタリ動物病院 東京医療センター 田畑達彦-2019.2.3)。
犬の咽頭閉塞の病態
Pollard RE, Johnson LR, Marks SL. The prevalence of dynamic pharyngeal collapse is high in brachycephalic dogs undergoing videofluoroscopy. Vet Radiol Ultrasound 2018;59:529-534. https://www.ncbi.nlm.nih.gov/pubmed/25673910
ビデオ透視検査を実施した短頭犬種での動的咽頭虚脱の高い有病率
The aim of this retrospective study was to determine the frequency of pharyngeal collapse in a large group of brachycephalic dogs undergoing videofluoroscopic assessment of swallowing or airway diameter. We hypothesized that brachycephalic dogs would have pharyngeal collapse more frequently than dolichocephalic or mesocephalic dogs with or without airway collapse. The medical records database was searched for brachycephalic dogs undergoing videofluoroscopy of swallowing or airway diameter between January 1, 2006 and December 31, 2015. A cohort of dolichocephalic/mesocephalic dogs with videofluoroscopically confirmed airway collapse was age and time matched for comparison. A control group of dolichocephalic/mesocephalic dogs that did not have documented airway collapse was also evaluated. All fluoroscopic studies were assessed by a board certified veterinary radiologist for the presence and degree of pharyngeal collapse. Results demonstrate that pharyngeal collapse was significantly more common in brachycephalic dogs (58/82; 72%) than in nonbrachycephalic dogs with (7/25; 28%) and without (2/30; 7%) airway collapse. Pharyngeal collapse is more prevalent in brachycephalic dogs undergoing videofluoroscopy than in dolichocephalic/mesocephalic dogs with or without airway collapse.
コメント:長頭/中頭犬種を比較対照とした、短頭犬種大規模グループでの透視検査による咽頭虚脱の回顧的研究。気道虚脱の有無にかかわらず、短頭犬種は長頭/中頭犬種より咽頭虚脱が多くみられる(いいのペットクリニック 飯野亮太-181228)。
城下幸仁. 【子どものいびき・睡眠時無呼吸症候群を探求する】 犬の短頭種気道症候群の病態から学ぶもの. 小児歯科臨床 2016;21:25-32.
コメント:分野の違う歯科医や小児科医にも分かりやすいように記述しました(犬・猫の呼吸器科 城下-2018.11.28)。
Rubin JA, Holt DE, Reetz JA, et al. Signalment, clinical presentation, concurrent diseases, and diagnostic findings in 28 dogs with dynamic pharyngeal collapse (2008-2013). J Vet Intern Med 2015;29:815-821.
動的咽頭虚脱をもつ犬28頭のシグナルメント、臨床症状、併発疾患、および診断所見
BACKGROUND: Most information about pharyngeal collapse in dogs is anecdotal and extrapolated from human medicine. A single case report describing dynamic pharyngeal collapse in a cat has been published, but there is no literature describing this disease process in dogs. OBJECTIVE: To describe the signalment, clinical presentation, concurrent disease processes, and imaging findings of a population of client-owned dogs with pharyngeal collapse. ANIMALS: Twenty-eight client-owned dogs with pharyngeal collapse. METHODS: Radiology reports of dogs for which fluoroscopy of the respiratory system was performed were reviewed retrospectively. Patients with a fluoroscopic diagnosis of pharyngeal collapse were included in the study population. Data regarding clinical signs, diagnostic, and pathologic findings were evaluated. RESULTS: Twenty-eight dogs met the inclusion criteria. The median age of affected patients was 6.6 years, whereas median body condition score was 7/9. The most common clinical signs were coughing (n = 20) and stertor (n = 5). In 27 of 28 cases, a concurrent or previously diagnosed cardiopulmonary disorder was detected. The most common concurrent disease processes were mainstem bronchi collapse (n = 18), tracheal collapse (n = 17), and brachycephalic airway syndrome (n = 8). Fluoroscopy identified complete pharyngeal collapse in 20 of 28 dogs. CONCLUSIONS: Pharyngeal collapse is a complex disease process that likely is secondary to long-term negative pressure gradients and anatomic and functional abnormalities. Based on the findings of this study, pharyngeal fluoroscopy may be useful diagnostic test in patients with suspected tracheal and mainstem bronchial collapse to identify concurrent pharyngeal collapse.
コメント1:気管および主気管支の虚脱のある犬では、透視検査にて咽頭虚脱の併発が確認されるかもしれない。また、肥満も素因もしくは悪化因子として関連しているかもしれない。8頭が短頭種、残り20頭のうち12頭はヨークシャーテリアであった(いいのペットクリニック 飯野亮太-181228)。
コメント2:咽頭虚脱の特徴づけの論文。28頭の咽頭虚脱の犬の年齢中央値は6.6歳、BCS中央値は7/9で最も多い臨床症状は咳とスターター、最も多い併発疾患は主気管支の虚脱、気管虚脱、短頭種気道症候群であった(ダクタリ動物病院東京医療センター 田畑達彦-2019.5.1)。
Petrof BJ, Pack AI, Kelly AM, et al. Pharyngeal myopathy of loaded upper airway in dogs with sleep apnea. J Appl Physiol (1985) 1994;76:1746-1752.
睡眠時無呼吸を示すイングリッシュ・ブルドッグにおける上気道負荷による咽頭筋傷害
Recent work indicates that upper airway dilator muscles of individuals with obstructive sleep apnea syndrome (OSAS) demonstrate an increased level of activity during wakefulness compared with normal subjects. In addition, massive bursts of pharyngeal dilator activity are associated with the termination of upper airway occlusive events during sleep. This complex pattern of altered pharyngeal dilator activation is also observed in the English bulldog, an animal model of OSAS. In the present study, it was hypothesized that such alterations in activity level might lead to changes in the structure of pharyngeal muscles in the bulldog. Full-thickness biopsies were obtained from two pharyngeal dilator muscles, the sternohyoid (SH) and geniohyoid, as well as a limb muscle, the anterior tibialis, in bulldogs (n = 5) and control dogs (n = 7). Immunohistochemical analysis of myosin heavy chain expression revealed an increased contribution of fast type II myosin heavy-chain fibers to SH in bulldogs. The bulldog SH also demonstrated increased connective tissue content compared with control dogs, consistent with the presence of fibrosis. Both pharyngeal dilators in the bulldog exhibited an elevated proportion of morphologically abnormal fibers indicative of ongoing or prior injury. No differences in any of the above parameters were seen between bulldogs and control dogs in the anterior tibialis limb muscle. We conclude that the chronic load and altered pattern of usage imposed on the upper airway dilators in OSAS lead to myopathic changes that may ultimately impair the ability of these muscles to maintain pharyngeal patency.
コメント:ヒトOSAS患者では、上気道拡張筋群が覚醒期に活動亢進していることがわかってきた。睡眠時にも同様に上気道の閉塞とともに咽頭拡張筋群が急激に活動開始する。この研究では、睡眠時無呼吸を示すイングリッシュブルドッグの咽頭拡張筋群でありオトガイ舌骨筋と胸骨舌骨筋、睡眠にかかわらない姿勢筋の前脛骨筋を全層生検し病理組織学的変化を比較し、さらに睡眠時無呼吸を示さない対照群の犬にも同様の生検を実施し比較対照とした。イングリッシュブルドッグの咽頭拡張筋群では筋線維の変性が優位に増加していた。OSASでは上気道筋の慢性負荷は筋変性を引き起こし、その結果として咽頭気道開存性を損なうかもしれない(犬・猫の呼吸器科 城下幸仁-2019.2.27)。
Suratt PM, Dee P, Atkinson RL, et al. Fluoroscopic and computed tomographic features of the pharyngeal airway in obstructive sleep apnea. Am Rev Respir Dis 1983;127:487-492.
OSA患者における透視下睡眠時咽頭気道および覚醒下CT検査所見
Because it has been suggested that patients with obstructive sleep apnea have a narrower pharyngeal airway than normal persons, we performed lateral fluoroscopy and computed tomographic (CT) scans of the pharynx in patients with this syndrome. Fluoroscopy in 6 sleeping patients showed that the obstruction always began during inspiration when the soft palate touched the tongue and posterior pharyngeal wall. The CT scans in 9 awake subjects demonstrated that the narrowest section of the airway in patients and in control subjects was the region posterior to the soft palate. The cross-sectional area of this region was significantly narrower in patients than it was in control subjects (p less than 0.001). Because a narrow airway would be more likely to collapse during inspiration than a normal one would (Bernoulli’s Principle), we conclude that the narrow airways we observed in awake patients may be an important contributing factor in the pathogenesis of obstructive sleep apnea.
コメント:6名のOSA患者の睡眠時側臥位咽頭気道所見から、吸気時に軟口蓋が舌と咽頭後壁に接触した。9名のOSA患者と非OSA者の対照群の覚醒下CT検査所見ではともに軟口蓋の後部でもっとも気道は狭窄しており、OSA 患者の方が対照群より優位にこの部位が狭窄していた。覚醒期に正常より気道が狭窄していることはOSAの病態において重要な因子であると結論された。咽頭気道の透視検査は動物の横臥に相当する体位で評価されていた(犬・猫の呼吸器科 城下幸仁-2019.2.27)。
睡眠時無呼吸
医学領域における咽頭閉塞や咽頭虚脱の病態生理
Veasey SC, Chachkes J, Fenik P, et al. The effects of ondansetron on sleep-disordered breathing in the English bulldog. Sleep 2001;24:155-160.
イングリッシュブルドッグにおける睡眠呼吸障害におけるオンダンセトロンの効果
Serotonin and serotoninergic drugs have significant effects on respiration, at many sites throughout the nervous system, and serotonin has been implicated in the pathogenesis of obstructive sleep apnea. Thus, understanding the serotoninergic mechanisms underlying respiratory control may help discover novel pharmacotherapies for sleep-disordered breathing. Ondansetron, a serotonin (5-HT) antagonist selective for the 5-HT3 receptor subtype has recently been shown to suppress sleep-related central apneas in rats, particularly in rapid-eye-movement (REM) sleep. To evaluate the potential of ondansetron in the treatment of obstructive sleep-disordered breathing, we have performed randomized trials of two doses of ondansetron (20 and 40 mg orally) and placebo (4 studies for each of the 3 conditions) in our animal model of obstructive sleep apnea, the English Bulldog. Ondansetron significantly reduced the respiratory disturbance index (RDI) in REM sleep from 24.15+/-4.85 events/hour at placebo to 11.01+/-1.56 events/hour with high dose treatment, n=4, p<0.05. In contrast, the effects of drug on the RDI in non-rapid-eye-movement (NREM) sleep (5.23+/-1.30 events/hour, placebo; 4.31+/-1.36, with 20 mg ondansetron and 2.89+/-1.30 with 40 mg ondansetron, n=4) were not significant. Ondansetron, however, had no effect on either sleep efficiency or sleep architecture, and there were no effects on either oxyhemoglobin saturation nadirs or on the sleep time with saturations <90%. Although a trend towards reduction in the latter measure of oxygenation was seen at the higher dose of ondansetron. These data suggest a therapeutic potential for ondansetron in obstructive sleep-disordered breathing, particularly REM sleep apnea.
コメント:イングリッシュ・ブルドッグにおいて、オンダンセトロンがREM睡眠期の無呼吸を減少させる効果があるとした文献(まるふく動物病院 福田大介-2019.6.3)
Schwartz AR, Eisele DW, Smith PL. Pharyngeal airway obstruction in obstructive sleep apnea: pathophysiology and clinical implications. Otolaryngol Clin North Am 1998;31:911-918.
閉塞性無呼吸における咽頭気道閉塞:病態生理と臨床的意義
In obstructive sleep apnea, airflow obstruction is caused by pharyngeal collapse. Current evidence suggests that anatomic alterations predispose to pharyngeal collapse. This article examines the role of structures that elongate and dilate the pharynx in maintaining pharyngeal patency. Their influence on pharyngeal collapsibility is considered. Insights gained are then presented within a conceptual framework that can be used for treating patients.
コメント:閉塞性睡眠時無呼吸の気道閉塞は睡眠時に咽頭気道が虚脱することによって生じる。この虚脱は、構造的問題と神経筋機能障害の両者のバランスによって生じると考えられているが、詳細機序は解明されていない。睡眠時の咽頭虚脱は、咽頭周囲圧で予測される。したがって、睡眠時に気流が生じ始める外鼻孔部での気道内圧でその程度を計測できる。終夜ポリソノグラフィーで持続陽圧呼吸(CPAP)を行ながら、その圧を測定することをCPAPタイトレーションと呼び、そのときの気道内圧は咽頭開存最小圧?(Pharyngeal critical pressure, Pcrit)と呼ばれる。この論文では、このPcrit計測を基準に睡眠時咽頭閉塞の病態について動物実験や臨床知見からレビューしている。Pcritは、咽頭気道を伸展させると低下する。これは、猫の分離した上気道の実験で、気管を後方に牽引して確認された。頚を伸展させると同様の効果が得られる。また、同様の実験で舌を前方に牽引すると咽頭気道が拡大した。しかしこの場合、Pcritはあまり低下しなかった。人では、仰臥位に比べ立位や横向き寝でPcirtが4〜5cmH2O低下した。逆の理論で、小下顎症での睡眠時無呼吸はこれで説明できる。 Pcritの治療目標は初期値の-5cmH2Oとするとおおよそ効果が得られる。Pcritがあまり高くなければ、15-20%の体重減量でこの治療目標をおおよそ達成できる。イングリッシュブルドッグをモデルとした研究では、構造的咽頭閉塞を代償するために咽頭筋の機能亢進が認められ、経年的に筋変性が生じていたことが確認された。人でも、無呼吸患者ではオトガイ舌筋の活動過剰が覚醒期に認められた。したがって現在では、構造的問題が咽頭虚脱性の主要因であり、さらにそれを代償するため神経筋活動の亢進を引き起こしていると推測されている。閉塞性無呼吸では、咽頭気道を伸展させたり、咽頭気道を広げたりするような治療を考案すればよいということになるが、未だ効果的な決定打はない(犬・猫の呼吸器科 城下幸仁-2018.2.27)。
Suto Y, Inoue Y. Sleep apnea syndrome. Examination of pharyngeal obstruction with high-speed MR and polysomnography. Acta Radiol 1996;37:315-320.
睡眠時無呼吸症候群:高速MRおよびポリソノグラフィーによる咽頭閉塞の検査
PURPOSE: We attempted to determine the usefulness of high-speed MR imaging for evaluating the severity of sleep apnea syndrome (SAS) by comparing findings of pharyngeal obstruction obtained with high-speed MR with those of all-night polysomnography (PSG). SUBJECTS AND METHODS: A total of 33 patients with SAS underwent turbo-FLASH MR examination, while awake and after i.v. injection of hydroxyzine hydrochloride. Serial images were examined by cinemode. Pharyngeal findings on MR were divided into single-site obstruction (SO) at the velopharynx, multiple-site obstruction (MO), and no obstruction (NO). PSG findings were analyzed to determine the predominant type of apnea, severity as evaluated by an apnea index (AI), and the lowest SaO2 value during sleep. RESULTS: Seventy-five percent of the central apnea group had SO, and 70% of the mixed apneas had MO, while only 15% of the obstructed apneas had MO. The percentage of patients with severe SAS (AI of 20% or higher) was 48% for the SO, and 70% for the MO. The lowest SaO2 value tended to be low in the mixed apnea in the case of PSG, and tended to be low in the MO at MR examination. CONCLUSION: Analysis of pharyngeal dynamics using high-speed MR may provide some useful information for evaluating the severity of SAS.
コメント:ポリソノグラフィー(PSG)で睡眠時無呼吸症候群(SAS)と診断した33例に、覚醒時と塩酸ヒドロキシラジン静注によって誘起した睡眠時にて、高速MR撮影にて咽頭気道の画像研究を行なった臨床研究。覚醒期には咽頭閉塞は認められなかったが、誘起された睡眠では33例中31例(94%)にて認められた。画像での咽頭閉塞部位のパターンを、口蓋帆咽頭部(いわゆる鼻咽頭後部)のみ(SO)、口蓋帆咽頭部と舌根など他の咽頭部を含む(MO)、閉塞なし(NO)の3つに分類した。重度SASではSOは56%、MOは39%で認められた。閉塞性無呼吸(19/33)ではSOは78%、MOは16%で認められた。中枢/閉塞混合性無呼吸(10/33)ではSOは30%、MO は70%で認められた。PSGは終夜患者を拘束するが、本研究のような高速MR撮影では、覚醒時および睡眠時検査を通じ、45-100分(平均80分)で終えることができ、睡眠呼吸障害のひとつの検査法として有用であると著者は主張している。
人では犬の咽頭のように咽頭背壁余剰が存在しないようです(下図)。閉塞部位は鼻咽頭後部と舌根であり、肥満SAS症例では舌根部位に脂肪沈着が優位であることが報告されています(犬・猫の呼吸器科 城下幸仁-2019.2.27)。
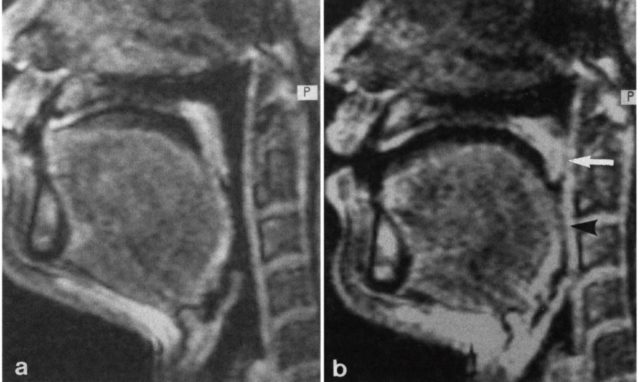
Fig. 2. Patient 2, a 65-year-old man with MO. a) Sagittal image when awake. b) Sagittal image with the subject asleep. During wakefulness, no obstruction was observed in the pharynx, but during sleep, obstructions were observed at the velopharynx (white arrow) and the tongue (black arrow head).
ヒトの睡眠時無呼吸
一般
American Academy of Sleep Medicine : The international classification of sleep disorders, 2nded : Diagnostic and coding manual. American Academy of Sleep Medicine, Westchester, 2005
榊原博樹. 睡眠時無呼吸症候群 診療ハンドブック. 東京:医学書院, 2010
人の睡眠時無呼吸の概要について
用語解説
- 無呼吸(apnea):成人では呼吸気流の停止〜基準振幅の10%未満が10秒以上持続したイベント。乳幼児、小児では持続時間を2呼吸サイクル分の時間とする。
- 低呼吸(hypopnea):換気量が規定以上に減少した状態。人ではresearch definitionおよびclinical definitionと呼ばれる2つの診断基準がある。research definitionでは3%以上の酸素飽和度低下あるいは覚醒反応を伴う呼吸気流の減少を低呼吸とする(ほとんどの施設がこの基準を採用)。clinical definitionでは呼吸気流の30%以上の減少に、4%以上の酸素飽和度低下を伴うイベントを低呼吸とする。
- 無呼吸指数(apnea index AI):全睡眠時間(total sleep time TST)1時間当たりの無呼吸の回数
- 無呼吸低呼吸指数(apnea hypopnea index AHI):TST1時間当たりの無呼吸+低呼吸の回数
- 睡眠呼吸障害(sleep disordered breathing SDB):睡眠時の無呼吸および低呼吸、あるいは酸素飽和度の低下を伴う呼吸異常のことで、症状の有無は問わない。
- 睡眠時無呼吸(sleep apnea SA)
- 閉塞型睡眠時無呼吸(obstructive sleep apnea OSA):上気道閉塞による睡眠時無呼吸。呼吸気流の停止は見られるが、胸腹部の呼吸運動は残存している。
- 中枢型睡眠時無呼吸(central sleep apnea CSA):呼吸中枢からの呼吸刺激出力の停止による睡眠無呼吸。呼吸気流の停止とともに、胸腹部の呼吸運動も停止する。
- 混合型睡眠時無呼吸(mixed sleep apnea MSA):CSAに続いてOSAが生じる無呼吸
- 閉塞型睡眠時無呼吸症候群(obstructive sleep apnea syndrome OSAS):1時間に5〜10以上のOSA主体のSDBが見られるSAS
- 中枢型睡眠時無呼吸症候群(central sleep apnea syndrome CSA):1時間に5〜10以上のCSA主体のSDBが見られるSAS
- 睡眠呼吸異常症(sleep breathing disorder SBD):SASに加えて、上気道抵抗症候群、いびき、肥満低換気症候群など睡眠時の呼吸異常を広く組み入れた概念のこと
OSASの概念
1時間に5〜10以上のOSA主体のSDBが見られるSAS。長時間継続すると徐々にPaCO2が上昇するが、覚醒によってほとんどが終了する。
OSASの診断基準は以下の二つである。(AASM 2005)
1 A+B+D
2 C+D
A 少なくとも以下の1項目を満たす
- 覚醒時の睡眠発作、昼間の眠気、熟睡感欠如、倦怠感、不眠
- 呼吸停止、喘ぎあるいは窒息館とともに覚醒
- ベッドパートナーによる大きないびきや呼吸停止の報告
B 終夜睡眠ポリグラフ検査による以下の所見を満たす
- AHI ≧ 5
- 各呼吸イベントの全てあるいは一部で呼吸努力が確認される
C 終夜睡眠ポリグラフ検査による以下の所見を満たす
- AHI ≧ 15
- 各呼吸イベントの全てあるいは一部で呼吸努力が確認される
D 他の睡眠障害、医学的あるいは神経学的異常、治療薬や薬物と関連した異常では説明できない
コメント:人では睡眠時無呼吸は特殊なモニター機器を終夜装着し、睡眠状態を記録して上記のような指標を算出して診断される。低呼吸については診断基準が2つあり、目的によって使い分けられている(乙訓どうぶつ病院 中森正也-2018.11.27)
閉塞性睡眠時無呼吸症候群(OSAS)
Corso R, Russotto V, Gregoretti C, et al. Perioperative management of obstructive sleep apnea: a systematic review. Minerva Anestesiol 2018;84:81-93.
doi: 10.23736/S0375-9393.17.11688-3
OSAの周術期管理
INTRODUCTION: Obstructive sleep apnea (OSA) is the leading sleep disordered breathing condition, with a prevalence rate of moderate to severe OSA of approximately 10-17% in the general population. EVIDENCE ACQUISITION: We performed an Ovid-Medline search of all articles published up to August 2016. We included all articles providing updated evidence on epidemiology, pathophysiologic mechanisms and perioperative interventions. EVIDENCE SYNTHESIS: OSA is associated with a number of comorbidities and increased perioperative risks. Although in-laboratory polysomnography represents the gold-standard for diagnosis of OSA, it is costly and time-consuming. Anesthesiologists may screen patients for OSA through one of the available questionnaires, of which the snoring, tiredness, observed apnea, high blood pressure (STOP)-Body Mass Index, age, neck circumference and gender (Bang), STOP-bang questionnaire is the most externally validated. Although its sensitivity for the identification of mild OSA patients is 83.6%, its specificity is only 56.4%. OSA patients are associated with a higher risk of both difficult ventilation and intubation. However, practice guidelines refer to available guidelines for difficult airway management. Perioperative continuous positive airway pressure use may be of benefit since it has been reported to be associated with a reduction of both respiratory and cardiovascular complications and symptom relief. When feasible, regional anesthesia techniques and a multimodal analgesia approach should be adopted to reduce intraoperative and postoperative exposure to opioids. CONCLUSIONS: Preoperative screening of OSA patients is of relevance given the increased perioperative morbidity of these patients. Further studies are needed to provide conclusive data on which perioperative interventions are most effective at reducing this risk.
コメント:中等度~重度のOSAを合併した外科患者の60%が術前にOSAの診断・治療を受けていない可能性がある(まるふく動物病院 福田大介-2019.2.5)
Faruqi S, Fahim A, Morice AH. Chronic cough and obstructive sleep apnoea: reflux-associated cough hypersensitivity? Eur Respir J 2012;40:1049-1050. doi:10.1183/09031936.00025012
OSAと慢性咳嗽: 胃食道逆流関連性咳感受性性亢進か?
Obstructive sleep apnoea (OSA) is being increasingly recognised as a cause of chronic cough. The impact of continuous positive airway pressure (CPAP) therapy and the mechanism of this association are not well understood. We describe a patient with OSA and chronic cough who responded well to CPAP. Objective and subjective assessments of cough on treatment with CPAP, off CPAP and on follow-up as well as pharyngeal pH monitoring suggest a possible mechanism for this association.
コメント:OSAは慢性咳嗽の原因になりうる。その場合、CPAP治療の是非はよくわかっていない。今回、慢性咳嗽をともなったOSASに遭遇し、CPAP療法によく反応した1例を経験した。両者の関連は、咽頭内pHをモニタすることによって考察できる(犬・猫の呼吸器科 城下幸仁-2019.2.27)
Chang SJ, Chae KY. Obstructive sleep apnea syndrome in children: Epidemiology, pathophysiology, diagnosis and sequelae. Korean J Pediatr 2010;53:863-871. (PDFあり)
小児における閉塞性睡眠時無呼吸症候群(OSAS):疫学、病態生理学、診断および後遺症について
The prevalence of pediatric obstructive sleep apnea syndrome (OSAS) is approximately 3% in children. Adenotonsillar hypertrophy is the most common cause of OSAS in children, and obesity, hypotonic neuromuscular diseases, and craniofacial anomalies are other major risk factors. Snoring is the most common presenting complaint in children with OSAS, but the clinical presentation varies according to age. Agitated sleep with frequent postural changes, excessive sweating, or abnormal sleep positions such as hyperextension of neck or abnormal prone position may suggest a sleep-disordered breathing. Night terror, sleepwalking, and enuresis are frequently associated, during slow-wave sleep, with sleep-disordered breathing. Excessive daytime sleepiness becomes apparent in older children, whereas hyperactivity or inattention is usually predominant in younger children. Morning headache and poor appetite may also be present. As the cortical arousal threshold is higher in children, arousals are not easily developed and their sleep architectures are usually more conserved than those of adults. Untreated OSAS in children may result in various problems such as cognitive deficits, attention deficit/hyperactivity disorder, poor academic achievement, and emotional instability. Mild pulmonary hypertension is not uncommon. Rarely, cardiovascular complications such as cor pulmonale, heart failure, and systemic hypertension may develop in untreated cases. Failure to thrive and delayed development are serious problems in younger children with OSAS. Diagnosis of pediatric OSAS should be based on snoring, relevant history of sleep disruption, findings of any narrow or collapsible portions of upper airway, and confirmed by polysomnography. Early diagnosis of pediatric OSAS is critical to prevent complications with appropriate interventions.
コメント:小児のOSASでは認知障害、注意欠陥/多動性障害、学業成績不良、および情緒不安定などのさまざまな問題を引き起こす可能性がある。またまれに、肺性心、心不全、全身性高血圧などの心血管合併症が発症することがある。動物でも同様に問題行動や、心血管系の異常をきたす可能性があるかもしれない(2019.4.1 乙訓どうぶつ病院 中森正也)
磯野史朗. 【睡眠時無呼吸 最近の進歩と展望】 睡眠時無呼吸の病態生理と呼吸調節 閉塞型睡眠時無呼吸 咽頭閉塞とその周期性のメカニズム. 最新医学 2009;64:14-21.
閉塞型睡眠時無呼吸(OSA)の病態は,依然としてすべてが解明されたわけではない.肥満あるいは顎顔面形態異常による咽頭周囲の解剖学的アンバランスが,咽頭閉塞性を増加させることは確かなようである.さらに,特に肥満OSA患者では,肺容量減少が咽頭閉塞性増加に大きく寄与しているようである.呼吸器系の不安定性が高い患者では,OSAを周期的に繰り返し重症化しやすいと考えられている.(著者抄録)
コメント:
Guglielminotti J, Tesniere A, Rackelboom T, et al. Cough reflex sensitivity is decreased in female obese patients with obstructive sleep apnea. Respir Physiol Neurobiol 2007;158:83-87.
閉塞性睡眠時無呼吸の女性肥満患者における咳反射感受性が低下する
Obstructive sleep apnea (OSA) is associated with impaired airway reflexes. Cough is the main airway defense mechanism but the effect of OSA on cough is unknown. Thirty-two female obese patients scheduled to undergo bariatric surgery were studied. They were classified as presenting OSA (20 patients) when the apnea-hypopnea index (AHI) was greater than 5h. Cough sensitivity was measured with citric acid. Increasing concentrations of nebulized citric acid were delivered until cough was elicited. The concentrations eliciting one (C1) and two coughs (C2) were recorded and log transformed (log C1 and log C2). log C1 and log C2 (median (interquartile)) were 1.90 mg/mL (0.90) and 2.2mg/mL (0.30) in OSA patients and 1.60 mg/mL (0.45) and 1.60 mg/mL (0.45) in non-OSA patients, respectively (comparison between groups: p=0.0372 for log C1 and p=0.0227 for log C2). A significant relationship was observed between AHI and log C1 and log C2. Cough sensitivity is therefore, decreased in female obese OSA patients and this decreased sensitivity is positively correlated with disease severity.
コメント:閉塞性睡眠時無呼吸症候群(OSAS)の肥満患者では咳嗽が生じにくいことを示した文献。また疾患の重症度と比例して、咳の感受性は低下した。(乙訓どうぶつ病院 中森正也-2019.4.1 )
Birring SS, Ing AJ, Chan K, et al. Obstructive sleep apnoea: a cause of chronic cough. Cough 2007;3:7.
睡眠時無呼吸:慢性咳嗽の原因
Chronic cough is a common reason for presentation to both general practice and respiratory clinics. In up to 25% of cases, the cause remains unclear after extensive investigations. We report 4 patients presenting with an isolated chronic cough who were subsequently found to have obstructive sleep apnoea. The cough improved rapidly with nocturnal continuous positive airway pressure therapy. Further studies are required to investigate the prevalence of coexistence of these common conditions.
コメント:OSAに合併した慢性咳嗽4例を経験した。すべて夜間のCPAP療法にてただちに改善した(犬・猫の呼吸器科 城下幸仁-2019.2.27)
Rosenow F, McCarthy V, Caruso AC. Sleep apnoea in endocrine diseases. J Sleep Res 1998;7:3-11.
内分泌疾患における睡眠時無呼吸
The pertinent literature on the prevalence, clinical manifestations and pathogenic mechanisms of sleep apnoea (SA) in endocrine diseases, namely acromegaly, Cushing syndrome, hypothyroidism and diabetes mellitus was reviewed. An increased prevalence is well documented in patients with active and treated acromegaly. While most authors report peripheral obstruction, due to hypertrophy of tongue and pharyngeal tissues, to be the cause of SA in acromegaly, some findings argue for a role of hormone-induced changes of central respiratory control. SA is also more common in hypothyroidism, especially when myxedema is present. The associated edema and myopathy appear to be of pathogenic importance. Thyroxin substitution is frequently effective for the treatment of SA but nCPAP can be necessary initially and in some patients even after remission of clinical signs of hypothyroidism. In Cushing disease and syndrome, parapharyngeal fat accumulation can cause SA, but no epidemiological information is available. In non insulin dependent diabetes (NIDDM), obesity is the common risk factor for both, nocturnal hypoxia and insulin resistance. In IDDM, the development of autonomic neuropathy may predispose to SA. Where treatment of the underlying endocrine disease is unable cure the associated SA, nCPAP is usually the treatment of first choice. More prospective studies are clearly needed to establish prevalences and resolve the controversies regarding pathogenesis.
コメント:先端肥大症、甲状腺機能低下症、クッシング症候群および糖尿病における睡眠時無呼吸の有病率、臨床症状および病原性機序に関する人の文献。先端肥大症は舌および咽頭組織の肥大がSA(睡眠時無呼吸)に起因する。甲状腺機能低下症は粘液水腫や浮腫、咽頭筋のミオパチーなどの症状があればSAとの関連性が示唆される。クッシング症候群においては、脂肪の蓄積がSAを引き起こし得るが、直接的な関連性は不明である。インスリン非依存型糖尿病では、肥満は低酸素症とインスリン抵抗性の両方に対する共通の危険因子ですが、直接的な関連性は不明である。インスリン依存型糖尿病では、自律神経障害の発症とSAとの関連性が示唆される(乙訓どうぶつ病院 中森正也-2019.2.2)。
Isono S, Remmers JE, Tanaka A, et al. Anatomy of pharynx in patients with obstructive sleep apnea and in normal subjects. J Appl Physiol (1985) 1997;82:1319-1326.
睡眠時無呼吸患者と健常成人における咽頭の形態
Anatomic abnormalities of the pharynx are thought to play a role in the pathogenesis of obstructive sleep apnea (OSA), but their contribution has never been conclusively proven. The present study tested this anatomic hypothesis by comparing the mechanics of the paralyzed pharynx in OSA patients and in normal subjects. According to evaluation of sleep-disordered breathing (SDB) by nocturnal oximetry, subjects were divided into three groups: normal group (n = 17), SDB-1 (n = 18), and SDB-2 (n = 22). The static pressure-area relationship of the passive pharynx was quantified under general anesthesia with complete paralysis. Age and body mass index were matched among the three groups. The site of the primary closure was the velopharynx in 49 subjects and the oropharynx in only 8 subjects. Distribution of the location of the primary closure did not differ among the groups. Closing pressure (PC) of the velopharynx for SDB-1 and SDB-2 groups (0.90 +/- 1.34 and 2.78 +/- 2.78 cmH2O, respectively) was significantly higher than that for the normal group (-3.77 +/- 3.44 cmH2O; P < 0.01). Maximal velopharyngeal area for the normal group (2.10 +/- 0.85 cm2) was significantly greater than for SDB-1 and SDB-2 groups (1.15 +/- 0.46 and 1.06 +/- 0.75 cm2, respectively). The shape of the pressure-area curve for the velopharynx differed between normal subjects and patients with SDB, being steeper in slope near Pc in patients with SDB. Multivariate analysis of mechanical parameters and oxygen desaturation index (ODI) revealed that velopharyngeal Pc was the only variable highly correlated with ODI. Velopharyngeal Pc was associated with oropharyngeal Pc, suggesting mechanical interdependence of these segments. We conclude that the passive pharynx is more narrow and collapsible in sleep-apneic patients than in matched controls and that velopharyngeal Pc is the principal correlate of the frequency of nocturnal desaturations.
コメント:咽頭の神経性調節を完全に排除した状態で、年齢・性別・BMIをマッチングした健常成人とOSA患者を比較した論文。OSA患者は健常成人に比較して、咽頭気道の最大断面積が小さく、より高い閉塞性を有する(まるふく動物病院 福田大介-2019.6.3)。
中枢性睡眠時無呼吸症候群(CSAS)
掲載準備中
乳幼児突然死症候群(SIDS)
Thach BT. The Role of the Upper Airway in SIDS and Sudden Unexpected Infant Deaths and the Importance of External Airway-Protective Behaviors Future. 2018. (PDFあり)
Upper airway obstruction causing sudden death is well recognized. Examples include food aspiration, infectious disease such as diphtheria, and intentional or accidental suffocation. Obstructive sleep apnea (OSA) has often been suggested as a cause of sudden and unexpected infant death (SUID). The fact that sudden infant death syndrome (SIDS)/SUID is believed to occur during sleep lends support for this theory. The cause of death in such a case would not be evident at post-mortem examination and so would be consistent with a SUID death. The severity of OSA increases with viral infections of the upper airway which increase nasal resistance. Additionally, epidemiological studies have found that a family history of OSA is a risk factor for SUID (1). However, were OSA to be a major cause of infant deaths, it would not explain the beneficial effect of back sleeping in reducing SUID/SIDS deaths. Significantly, brief episodes of upper airway obstruction during sleep are more common in infants who ultimately died of SIDS/SUID than in infants who survived (2).
コメント:SIDSの一因としてOSASや上気道の感染が認められている。OSASの家族歴はSIDSの危険因子である。残念ながら、SIDSの全症例がOSASを呈しているわけではないため、他の要因も今後検討する必要がある(2019.4.1 乙訓どうぶつ病院 中森正也)。
磯野史朗. ピットフォール 乳幼児突然死症候群(SIDS)の病態生理 最近の概念. 呼吸(0286-9314) 2012;31:259-263.
乳幼児突然死症候群(SIDS)発症の病態は依然として解明されていないが、閉塞型睡眠時無呼吸(OSA)とSIDSとの関連性が強く支持されている。通常OSAは致死的な疾患ではないが、OSAから回復し呼吸を再開する生体防御過程が障害されることでSIDSへ進展する可能性がある。SIDS乳児は、巨舌・小顎などの咽頭閉塞性を高める解剖学的特徴を有し、事実SIDS乳児は生前OSAの頻度が正常乳児よりも多いことが判明した。このような解剖学的特徴を有しない場合でも、うつぶせによって咽頭閉塞性が増加し神経性代償が働かない状況ではOSAを発症する可能性もある。SIDSあるいはALTE乳児では、呼吸の化学調節系、覚醒反応、自律神経機能などの障害を示唆する報告も多い。今後の研究の進展が期待されるとともに、乳児におけるOSAの診断と治療の重要性が広く認識されるべきと考える。(著者抄録)
コメント:
犬の睡眠時無呼吸に関する臨床研究、実験的研究
Kopke MA, Wightman P, Ruaux CG. Obstructive sleep apnea in a Chihuahua successfully managed with ondansetron. Clin Case Rep 2019;7:872-876.
オンダンセトロンにて治療に成功したチワワの閉塞性睡眠時無呼吸の1例
While the persistence of clinical signs related to brachycephalic obstructive airway syndrome, particularly sleep-disordered breathing patterns following appropriate surgical management is likely to be relatively rare, this potential sequela needs to be considered, along with being aware of possible medical management options such as serotonin antagonists.
コメント:慢性鼻炎症状に伴う閉塞性睡眠時無呼吸を呈したチワワに対し、オンダンセトロン投与がSDB症状改善に有効であったという症例報告(まるふく動物病院 福田大介-2019.6.3 )。
Hinchliffe TA, Liu NC, Ladlow J. Sleep-disordered breathing in the Cavalier King Charles spaniel: A case series. Vet Surg 2018. http://doi org/10.1111/vsu.13148 (PDF)
キャバリア・キング・チャールズの睡眠呼吸障害の5例
OBJECTIVE: To describe sleep-disordered breathing (SDB) in the Cavalier King Charles spaniel (CKCS).
STUDY DESIGN: Retrospective case series.
ANIMALS: Five client-owned dogs referred for SDB.
METHODS: Medical records were reviewed including recheck appointments and routine preoperative and postoperative questionnaires. Whole-body barometric plethysmography was used to categorize SDB.
RESULTS: All dogs presented with multiple episodes of stertorous breathing, choking, and apnea during sleep. Severe nasal septal deviation, aberrant nasal turbinates, and soft palate elongation and thickening were noted on computed tomography and rhinoscopy of each dog. Whole-body barometric plethysmography measurements during sleep (in 3 dogs) documented periods of choking, snoring, and apnea. Treatment combined laser turbinectomy, folding flap palatoplasty, tonsillectomy, laryngeal sacculectomy, and cuneiform process resection. All dogs improved in terms of incidence and severity of sleep apnea within 1 week, with 4 of 5 dogs achieving complete resolution.
CONCLUSION: The objective measurements used to characterize SDB in this population of CKCS provided some evidence to support an obstructive cause for this condition, which improved with surgical treatment.
CLINICAL SIGNIFICANCE: Sleep-disordered breathing in the CKCS is a different clinical presentation of brachycephalic obstructive airway syndrome. Our finding of intranasal abnormalities in these 5 dogs with SDB provides justification for future research into its clinical significance.
コメント:(報告概要)睡眠時呼吸障害を示したキャバリア5例の後ろ向き記述研究。問診票で治療前後の主観評価、睡眠中の体プレチスモグラフィーをもちいて睡眠呼吸障害の客観的分類を試みた。5例全ての犬が睡眠中いびき呼吸、無呼吸、息がつまるといった経験を複数回経験していた。重度の鼻中隔の変位、鼻甲介の変形、軟口蓋の肥厚・過長がそれぞれの犬でCTや鼻鏡検査で明らかになった。3頭で睡眠中の体プレチスモグラフィーで息詰まり、いびき、無呼吸が計測された。治療はレーザーでの鼻甲介切除術、軟口蓋形成術、扁桃切除、喉頭小嚢切除、楔状突起の切除の組み合わせで行われた。1週間以内に無呼吸の重症度と頻度が改善され、5頭中4頭が完全に寛解した。
この犬種における睡眠時呼吸障害は外科的な治療によって寛解したため、上部気道閉塞が原因である可能性が高いと考えられる。キャバリアはキアリ奇形と心臓病の好発犬種であり、中枢性の睡眠時無呼吸との関連、心不全と睡眠時無呼吸との関連など今後の研究対象として興味深い(ぬのかわ犬猫病院 布川智範-2019.1.2)。
城下幸仁. 【犬と猫の睡眠】 睡眠時無呼吸症. MVM 2018;27:26-37.
コメント:6症例を提示した。上記報告の追跡を行なった。永久気管切開術を実施した3例はQOL良好を維持し長期生存した(1331、2761、2826日間)。犬の睡眠時無呼吸症の診断基準を以下のように定義した。
- 睡眠時に閉塞性無呼吸がある(2呼吸以上もしくは10秒以上)
- 無呼吸発作関連症状が認められる
- 覚醒時頭部X線または透視検査にて咽頭閉塞を認める
上記、全てを満たす。
(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
Meira C, Joerger FB, Kutter APN, et al. Comparison of three continuous positive airway pressure (CPAP) interfaces in healthy Beagle dogs during medetomidine-propofol constant rate infusions. Vet Anaesth Analg 2018;45:145-157. doi: 10.1016/j.vaa.2017.11.001
メデトミジン-プロポフォールCRIを行った健康なビーグル犬で、3種類のインターフェースを用いたCPAPを比較(全文あり)
OBJECTIVE: To compare the efficacy of three continuous positive airway pressure (CPAP) interfaces in dogs on gas exchange, lung volumes, amount of leak during CPAP and rebreathing in case of equipment failure or disconnection. STUDY DESIGN: Randomized, prospective, crossover, experimental trial. ANIMALS: Ten purpose-bred Beagle dogs. METHODS: Dogs were in dorsal recumbency during medetomidine-propofol constant rate infusions, breathing room air. Three interfaces were tested in each dog in a consecutive random order: custom-made mask (M), conical face mask (FM) and helmet (H). End-expiratory lung impedance (EELI) measured by electrical impedance tomography was assessed with no interface (baseline), with the interface only (No-CPAP for 3 minutes) and at 15 minutes of 7 cmH2O CPAP (CPAP-delivery). PaO2 was assessed at No-CPAP and CPAP-delivery, partial pressure of inspired carbon dioxide (PICO2; rebreathing assessment) at No-CPAP and the interface leak (DeltaPleak) at CPAP-delivery. Mixed-effects linear regression models were used for statistical analysis (p<0.05). RESULTS: During CPAP-delivery, all interfaces increased EELI by 7% (p<0.001). Higher DeltaPleak was observed with M and H (9 cmH2O) in comparison with FM (1 cmH2O) (p<0.001). At No-CPAP, less rebreathing occurred with M (0.5 kPa, 4 mmHg) than with FM (1.8 kPa, 14 mmHg) and with H (1.4 kPa, 11 mmHg), but also lower PaO2 was measured with M (9.3 kPa, 70 mmHg) than with H (11.9 kPa, 90 mmHg) and FM (10.8 kPa, 81 mmHg). CONCLUSIONS AND CLINICAL RELEVANCE: All three interfaces can be used to provide adequate CPAP in dogs. The leak during CPAP-delivery and the risk of rebreathing and hypoxaemia, when CPAP is not maintained, can be significant. Therefore, animals should always be supervised during administration of CPAP with any of the three interfaces. The performance of the custom-made M was not superior to the other interfaces.
コメント:10頭のビーグルで、比較的深い鎮静下で3種類のインターフェース(特注型、フェイスマスク型、ヘルメット型:それぞれ下図のa、b、c)を用いたCPAPを行った論文。それら3つのインターフェースについて、効果的にCPAPが行えるかどうか、また回路トラブル時の安全性はどうか、を比較検討している(まるふく動物病院 福田大介-2019.2.5)。
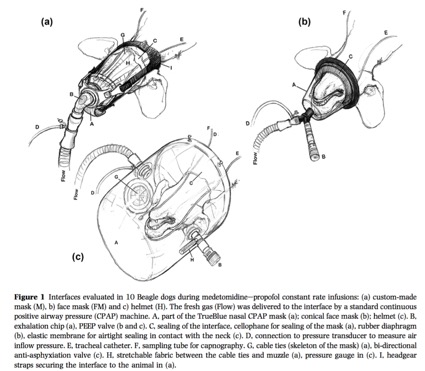
Staffieri F, Crovace A, De Monte V, et al. Noninvasive continuous positive airway pressure delivered using a pediatric helmet in dogs recovering from general anesthesia. J Vet Emerg Crit Care (San Antonio) 2014;24:578-585.
犬において全身麻酔からの覚醒時に小児用ヘルメット型マスクを用いたCPAP療法
OBJECTIVE: To evaluate the feasibility and efficacy of noninvasive continuous positive airway pressure (CPAP) administered with a pediatric helmet in healthy dogs recovering from general anesthesia. DESIGN: Randomized, cross-over, clinical study. SETTING: University teaching hospital. ANIMALS: Fifteen healthy female, client-owned dogs recovering from general anesthesia following elective ovariohysterectomy. INTERVENTIONS: All dogs received the same standardized anesthetic protocol (acepromazine, morphine, propofol, and isoflurane in oxygen). After extubation, a pediatric helmet was placed on all dogs and connected to a venturi valve supplied with medical air. In all patients, the gas flow was set to 50 L/minute and the FiO2 to 0.21. Dogs received the following sequence of treatments, each lasting 20 minutes: 0 CPAP (pre-CPAP), CPAP of 5 cm H2 O (CPAP), and again 0 CPAP (post-CPAP). MEASUREMENTS AND MAIN RESULTS: During the entire study, the following data were collected: pressure and FiO2 inside the helmet, mean arterial pressure, respiratory rate, heart rate, sedation score (0 = awake, 10 = deep sedation), and tolerance to the helmet (0 = excellent, 4 = poor). At the end of each phase, an arterial blood sample was sampled. As compared with the pre-CPAP and the post-CPAP periods, during the CPAP period, the PaCO2 , alveolar-arterial oxygen gradient (P[A-a]O2 ), and respiratory rate significantly decreased. The PaO2 was higher at CPAP (105.6 +/- 4.0 mm Hg) compared with pre-CPAP (80.6 +/- 6.9 mm Hg) and post-CPAP (86.7 +/- 5.8 mm Hg). Tolerance and sedation scores during the CPAP period were not different from those in the pre-CPAP and post-CPAP periods. CONCLUSIONS: Noninvasive CPAP applied through a helmet is a feasible and effective supportive technique in dogs recovering from general anesthesia.
コメント:卵巣子宮摘出術を受けた15頭の犬の覚醒時に対して、小児用ヘルメット型マスクを用いCPAPを行った文献。CPAPによってPaCO2、AaDO2、呼吸数は有意に減少し、PaO2は有意に増加した。また、CPAPによりtoleranceスコア、sedationスコアが上昇することはなかった(まるふく動物病院 福田大介-2019.3.4)。
Briganti A, Melanie P, Portela D, et al. Continuous positive airway pressure administered via face mask in tranquilized dogs. J Vet Emerg Crit Care (San Antonio) 2010;20:503-508.
鎮静下の犬にフェイスマスクを用いて行ったCPAP療法
OBJECTIVE: To evaluate the tolerance of a continuous positive airway pressure (CPAP) mask in tranquilized dogs and compare PaO(2) in arterial blood in dogs receiving oxygen with a regular face mask or CPAP mask set to maintain a pressure of 2.5 or 5 cm H(2)O. DESIGN: Prospective, randomized clinical study. SETTING: University teaching hospital. ANIMALS: Sixteen client-owned dogs without evidence of cardiopulmonary disease were studied. INTERVENTIONS: Eight animals were randomly assigned to each of 2 treatment groups: group A received 2.5 cm H(2)O CPAP and group B received 5 cm H(2)O CPAP after first receiving oxygen (5 L/min) by a regular face mask. Animals were tranquilized with acepromazine 0.05 mg/kg, i.v. and morphine 0.2 mg/kg, i.m.. An arterial catheter was then placed to facilitate blood sampling for pHa, PaO(2), and PaCO(2) determinations before and after treatments. Direct mean arterial pressure, heart rate, respiratory rate, and temperature were also recorded after each treatment. MEASUREMENTS AND MAIN RESULTS: CPAP administration was well tolerated by all animals. The mean arterial pressure, heart rate, respiratory rate, temperature, PaCO(2), and pHa, did not differ at any time point between groups. Differences were seen in oxygenation; in group A, PaO(2) significantly increased from a mean of 288.3 +/- 47.5 mm Hg with a standard mask to a mean of 390.3 +/- 65.5 mm Hg with the CPAP mask and in group B, PaO(2) increased similarly from 325.0 +/- 70.5 to 425.2 +/- 63.4 mm Hg (P<0.05); no differences were detected between the 2 CPAP treatments. CONCLUSIONS: In healthy tranquilized dogs noninvasive CPAP is well tolerated and increases PaO(2) above values obtained when using a regular face mask.
コメント:鎮静下の犬16頭において、フェイスマスクを用いてCPAPを行った文献。フェイスマスクを介した一般的な酸素投与と比較して、フェイスマスク+CPAPを実施した方が、有意に酸素化能が高かった(まるふく動物病院 福田大介-2019.3.4)。
城下幸仁, 山本洋史, 松田岳人ら. 犬の睡眠時無呼吸症と考えられた5例. 第30回動物臨床医学会年次大会プロシーディング 2009:159-160.
コメント:重度な無呼吸症状を呈した合計6例報告。4例が永久気管切開術にて治療しQOL改善をえられた。4例中3例は非短頭種であった(犬・猫の呼吸器科 城下幸仁-2018.11.29)
Hendricks JC, Kline LR, Kovalski RJ, et al. The English bulldog: a natural model of sleep-disordered breathing. J Appl Physiol 1987;63:1344-1350. (PDFあり)
睡眠呼吸障害の自然発症モデルとしてのイングリッシュ・ブルドッグ
To establish a natural model of sleep-disordered breathing, we investigated respiration during wakefulness and sleep in the English bulldog. This breed is characterized by an abnormal upper airway anatomy, with enlargement of the soft palate and narrowing of the oropharynx. During sleep, the animals had disordered respiration and episodes of O2 desaturation. These were worst in rapid-eye-movement (REM) sleep, with most bulldogs having O2 saturations of less than 90% for prolonged durations. In contrast, control dogs never desaturated. In REM sleep, the bulldogs had episodes of both central and obstructive apnea, the latter being associated with paradoxical movements of the rib cage and abdomen. During wakefulness, the bulldogs were hypersomnolent as evidenced by a shortened sleep latency (mean of 12 min compared with greater than 150 min for controls). This animal model should facilitate studies of the natural history of the sleep apnea syndrome and its complications.
コメント:イングリッシュ・ブルドッグで終夜ポリソノグラフィーを実施し、人の睡眠時無呼吸研究のモデルとして使用可能であることを実験的に初めて示した研究。イングリッシュ・ブルドッグでは、REM睡眠期に無呼吸が優位に認められ、閉塞性無呼吸と中枢性無呼吸の両方が認められた。睡眠中の酸素飽和度の低下、日中の傾眠など人の睡眠時無呼吸症候群と同様の所見が確認された(犬・猫の呼吸器科 城下幸仁-2019.2.27)
犬の咽頭閉塞と周術期リスク
Gruenheid M, Aarnes TK, McLoughlin MA, et al. Risk of anesthesia-related complications in brachycephalic dogs. J Am Vet Med Assoc 2018;253:301-306. (PDF)
短頭犬種における麻酔関連合併症のリスク
OBJECTIVE To determine whether brachycephalic dogs were at greater risk of anesthesia-related complications than nonbrachycephalic dogs and identify other risk factors for such complications. DESIGN Retrospective cohort study.
ANIMALS 223 client-owned brachycephalic dogs undergoing general anesthesia for routine surgery or diagnostic imaging during 2012 and 223 nonbrachycephalic client-owned dogs matched by surgical procedure and other characteristics.
PROCEDURES Data were obtained from the medical records regarding dog signalment, clinical signs, anesthetic variables, surgery characteristics, and complications noted during or following anesthesia (prior to discharge from the hospital). Risk of complications was compared between brachycephalic and nonbrachycephalic dogs, controlling for other factors.
RESULTS Perianesthetic (intra-anesthetic and postanesthetic) complications were recorded for 49.1% (n = 219) of all 446 dogs (49.8% [111/223] of brachycephalic and 48.4% [108/223] of nonbrachycephalic dogs), and postanesthetic complications were recorded for 8.7% (39/446; 13.9% [31/223] of brachycephalic and 3.6% [8/223] of nonbrachycephalic dogs). Factors associated with a higher perianesthetic complication rate included brachycephalic status and longer (vs shorter) duration of anesthesia; the risk of perianesthetic complications decreased with increasing body weight and with orthopedic or radiologic procedures (vs soft tissue procedures). Factors associated with a higher postanesthetic complication rate included brachycephalic status, increasing American Society of Anesthesiologists status, use of ketamine plus a benzodiazepine (vs propofol with or without lidocaine) for anesthetic induction, and invasive (vs noninvasive) procedures.
CONCLUSIONS AND CLINICAL RELEVANCE Controlling for other factors, brachycephalic dogs undergoing routine surgery or imaging were at higher risk of peri- and postanesthetic complications than nonbrachycephalic dogs. Careful monitoring is recommended for brachycephalic dogs in the perianesthetic period.
コメント:(論文概要)短頭種は他の犬種よりも麻酔の周術期リスクがあることを確認するため、オハイオ州立大学で2012年1月から12月まで手術や画像診断のために全身麻酔を受けた非短頭種と短頭種の診療記録をもとにしたマッチドケースコンロール研究。ASA分類のⅠ~ Ⅲを対象とし、麻酔前危険度評価の高いⅣ~Ⅴは除外した。多変量ロジスティック回帰分析にてリスクファクターを抽出した。本研究では非短頭種と比べ、短頭種の麻酔中の合併症は1.57倍で周術期では4.33倍であった。全体の周術期の合併症は49.1%(n=219/全446頭中)で麻酔中の合併症は40.4%(n=180)手術後の合併症は8.7%(n=39)だった。短頭種は上記の順に49.8%(n=111)49.3%(n=110)13.9%(n=31)で非短頭種では順に48.4%(n=108)48.9%(n=109)3.6%(n=8)だった。術後の合併症で最も一般的なのは誤嚥性肺炎で9頭の短頭種(4.0%)で非短頭種ではなかった。麻酔リスクの低い症例を選択したにもかかわらず、短頭犬種で2例の周術期死亡例があった。1例の短頭種は硝子体内ゲンタマイシン注入の為、プロポフォールで麻酔導入中に心停止を起こした。もう1例の短頭種はビルロート2型の手術後4日で死亡した。この症例は朝処置の間に呼吸が止まり、心停止を起こした。短頭種犬は非短頭種と比較して周術期に合併症のリスクが今回の研究では高く、特に麻酔後に顕著であった。抜管時に気道閉塞が起こり得るため、麻酔中よりもむしろ麻酔後に合併症がより起きやすい傾向にある。
短頭種は麻酔のリスクが高いということを論文で出したことに大きな意義がある。短頭種気道症候群の重症度に分類したオッズ比のデータがないことは残念。ASA分類Ⅱに分類している短頭種がASAⅡよりも麻酔の合併症のリスクが高いので、Ⅱ以上に分類すべきだと思う(ぬのかわ犬猫病院 布川智範-2019.1.2)。
城下幸仁. 時間軸で考える短頭種気道症候群. 中島尚志編集. 時間軸で考える獣医外科病態生理学. 東京: インターズー, 2018;24-37.
コメント:ある学会後のアンケートで全回答者の30%が短頭種の麻酔後死亡事故を経験していた(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Ree JJ, Milovancev M, MacIntyre LA, et al. Factors associated with major complications in the short-term postoperative period in dogs undergoing surgery for brachycephalic airway syndrome. Can Vet J 2016;57:976-980. https://www.ncbi.nlm.nih.gov/pubmed/27587891
短頭種気道症候群に対して外科的治療を行った犬において、重大な周術期合併症に関連する因子
Surgical correction of brachycephalic airway syndrome (BAS) in dogs has been reported to result in low complication rates and good long-term outcomes. Previous reports have not identified risk factors for the development of complications following BAS surgery. This retrospective study evaluated a wide variety of patient- and procedure-related, pre-operative, intra-operative, and post-operative factors for an association with the development of major postoperative complications in the short-term period following BAS surgery. The overall major complication rate, including death or euthanasia, was 4/55 (7%) dogs. Temporary tracheostomy was the only major surgical complication identified (n = 3). Multiple logistic regression identified postoperative radiographic evidence of pneumonia as associated with the development of any major complication overall, requirement of a temporary tracheostomy postoperatively, and death or euthanasia, within the short-term postoperative period. Future prospective studies should evaluate specific risk factors for an association with major complications following BAS surgery in dogs to improve patient outcomes.
コメント:BASの外科的治療(外鼻孔拡大術、軟口蓋過長整復術、喉頭小嚢切除術)を受けた犬のうち15%が、再度の外科治療(同術式)を必要とした。BASの外科的治療周術期における、BASに起因する消化器症状の治療のためのメトクロプラミドCRIが、誤嚥性肺炎などの重篤な合併症の重大なリスク因子になる(上大岡キルシェ動物病院 山下智之-2019.2.5)
コメント:BASに対する外科的矯正を行った犬55頭の回顧的調査。多重ロジスティック回帰で、術後短期間での重大な合併症(一時的気管切開、死亡、安楽死)に関連する因子は、術後のレントゲン検査上の肺炎像のみであった。この研究で吸引性肺炎の報告はないため、他の呼吸器疾患が関連しているかもしれない。ただし、以前の報告と同様に合併症率は低いため、大規模試験が必要(いいのペットクリニック 飯野亮太-2019.2.7)。
Dyson DH, Maxie MG, Schnurr D. Morbidity and mortality associated with anesthetic management in small animal veterinary practice in Ontario. J Am Anim Hosp Assoc 1998;34:325-335.
During 1993, 66 small animal practices participated in a prospective study to evaluate the incidence and details of anesthetic-related morbidity and mortality. Considering a total of 8,087 dogs and 8,702 cats undergoing anesthesia, the incidences of complications were 2.1% and 1.3%, respectively. Death occurred in 0.11% and 0.1% of cases, respectively. Logistic regression models were developed and showed that a significant odds ratio (OR) of complications in dogs was associated with xylazine (OR, 91.5); heart rate monitoring (OR, 3.2); American Society of Anesthesiologists (ASA) 3, 4, or 5 classification (OR, 2.5); isoflurane (OR, 2.4); butorphanol (OR, 0.35); technician presence (OR, 0.26); acepromazine (OR, 0.24); ketamine (OR, 0.21); and mask induction (OR, 0.2). Complications in cats were associated with ASA 3, 4, or 5 classification (OR, 5.3); diazepam (OR, 4.1); intubation (OR, 1.7); butorphanol (OR, 0.45); and ketamine (OR, 0.17). Cardiac arrest in dogs was associated with xylazine (OR, 43.6) and ASA 3, 4, or 5 classification (OR, 7.1). Cardiac arrest in cats was associated with ASA 3, 4, or 5 classification (OR, 21.6) and technician presence (OR, 0.19). This paper reports the incidences of complications and cardiac arrest in small animal practice and identifies common complications and factors that may influence anesthetic morbidity and mortality. This information may be useful in comparing anesthetic management practices.
コメント:イングリッシュブルドッグは犬種別では最も高い25%の確率で麻酔関連合併症が生じた。それらは呼吸器関連であった。その他の短頭種も含めると短頭種全体では4%の確率で麻酔関連合併症が生じた。ジャックラッセルは高い確率(10%)で麻酔関連合併症が生じた。著者は、1年間で9例の術中心停止を経験したが、そのうち3例が短頭種であり、さらにそのうち2例は上気道閉塞に関連したものであった(犬・猫の呼吸器科 城下幸仁-2019.7.30)。
非外科群の生存期間やQOL評価
掲載準備中
非短頭種の咽頭閉塞性疾患「咽頭気道閉塞症候群、Pharyngeal airway obstruction syndrome (PAOS)」
城下幸仁、稲葉健一:咽頭気道閉塞症候群89例. 第39回動物臨床医学会年次大会プロシーディングno.3 2018:18-22.
非短頭犬種では、頭部X線検査で短頭犬種とは異なる咽頭気道の構造異常があることに着目し、咽頭気道閉塞症候群を定義した。当院呼吸器科4年間の診療記録からこの画像所見を示す89例を抽出し、臨床像、治療、転帰について後向きに調査した。犬種では、ポメラニアン、ヨークシャー・テリア、チワワで好発し、発症年齢中央値は9歳であり、主訴では慢性咳嗽、徴候では肥満、最終診断では気管虚脱が最も多かった。治療は約半数で体重減量が処方され3ヶ月後にはその86.7%で初期症状は改善した。一方、進行例では睡眠時無呼吸や陰圧性肺水腫を発症し、特に後者では60日生存率が66.7%であった。早期に本疾患を認識し減量治療を開始すべきである。
コメント:2009.1~2013.10の犬・猫の呼吸器科(旧:相模が丘動物病院 呼吸器科)初診全例を対象とした。データ集計後、5年が経過しているが、本研究結果の矛盾する所見は未だに得られておらず、犬の上気道閉塞の一疾患としてのentityとして妥当であると考えられる(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
肥満と咽頭気道(ヒト)
Kim AM, Keenan BT, Jackson N, et al. Tongue fat and its relationship to obstructive sleep apnea. Sleep2014;37:1639-1648.
舌の脂肪はOSAと関連する
STUDY OBJECTIVES: The objective of this study was to determine whether tongue fat is increased in obese sleep apneics compared to obese subjects without sleep apnea. We hypothesized that excess fat is deposited in the tongue in obese patients with sleep apnea. DESIGN: Case-control design. SETTING: Academic medical center. PATIENTS: We examined tongue fat in 31 obese controls (apnea-hypopnea index, 4.1 +/- 2.7 events/h) and 90 obese apneics (apnea-hypopnea index, 43.2 +/- 27.3 events/h). Analyses were repeated in a subsample of 18 gender-, race-, age-, and BMI-matched case-control pairs. INTERVENTIONS: All subjects underwent a MRI with three-point Dixon magnetic resonance imaging. We used sophisticated volumetric reconstruction algorithms to study the size and distribution of upper airway fat deposits in the tongue and masseter muscles within apneics and obese controls. MEASUREMENTS AND RESULTS: The data supported our a priori hypotheses that after adjustment for age, BMI, gender, and race, the tongue in apneics was significantly larger (P = 0.001) and had an increased amount of fat (P = 0.002) compared to controls. Similar results were seen in our matched sample. Our data also demonstrate that within the apneic and normal tongue, there are regional differences in fat distribution, with larger fat deposits at the base of the tongue. CONCLUSIONS: There is increased tongue volume and deposition of fat at the base of tongue in apneics compared to controls. Increased tongue fat may begin to explain the relationship between obesity and obstructive sleep apnea.
コメント:SAがない肥満患者に比べ、SAがある肥満患者は舌の容積が脂肪沈着によって有意に増大していた。肥満とOSAの関連は、舌への脂肪沈着によって説明できるかもしれない(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
磯野史朗. 【睡眠時無呼吸 最近の進歩と展望】 睡眠時無呼吸の病態生理と呼吸調節 閉塞型睡眠時無呼吸 咽頭閉塞とその周期性のメカニズム. 最新医学2009;64:14-21.
閉塞型睡眠時無呼吸(OSA)の病態は,依然としてすべてが解明されたわけではない.肥満あるいは顎顔面形態異常による咽頭周囲の解剖学的アンバランスが,咽頭閉塞性を増加させることは確かなようである.さらに,特に肥満OSA患者では,肺容量減少が咽頭閉塞性増加に大きく寄与しているようである.呼吸器系の不安定性が高い患者では,OSAを周期的に繰り返し重症化しやすいと考えられている.(著者抄録)(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Brennick MJ, Pack AI, Ko K, et al. Altered upper airway and soft tissue structures in the New Zealand Obese mouse. Am J Respir Crit Care Med2009;179:158-169.
肥満マウスの上気道とその軟部組織構造の変化
RATIONALE: The effect of obesity on upper airway soft tissue structure and size was examined in the New Zealand Obese (NZO) mouse and in a control lean mouse, the New Zealand White (NZW). OBJECTIVES: We hypothesized that the NZO mouse has increased volume of neck fat and upper airway soft tissues and decreased pharyngeal airway caliber. METHODS: Pharyngeal airway size, volume of the upper airway soft tissue structures, and distribution of fat in the neck and body were measured using magnetic resonance imaging (MRI). Dynamic MRI was used to examine the differences in upper airway caliber between inspiration and expiration in NZO versus NZW mice. MEASUREMENTS AND MAIN RESULTS: The data support the hypothesis that, in obese NZO versus lean NZW mice,airway caliber was significantly smaller (P < 0.03), with greater parapharyngeal fat pad volumes (P < 0.0001) and a greater volume of other upper airway soft tissue structures (tongue, P = 0.003; lateral pharyngeal walls, P = 0.01; soft palate, P = 0.02).Dynamic MRI showed that the airway of the obese NZO mouse dilated during inspiration, whereas in the lean NZW mouse, the upper airway was reduced in size during inspiration. CONCLUSIONS: In addition to the increased volume of pharyngeal soft tissue structures, direct fat deposits within the tongue may contribute to airway compromise in obesity. Pharyngeal airway dilation during inspiration in NZO mice compared with narrowing in NZW mice suggests that airway compromise in obese mice may lead to muscle activation to defend upper airway patency during inspiration.
コメント: Dynamic MRI検査。正常マウスに比べ、肥満マウスでは、咽頭周囲脂肪組織が有意に増加した(P < 0.0001)。上気道内構造では、舌(P=0.003)と咽頭側壁(P=0.01)と軟口蓋(P=0.02)の容積が増加し、咽頭気道径が減少した。さらに、吸気時に、正常マウスの咽頭は咽頭気道径が縮小したのに対し、肥満マウスは咽頭気道が拡張した。肥満マウスでは、上気道開存を維持するため、上気道開大筋活動によって代償している(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
榊原博樹. 睡眠呼吸障害. 日本呼吸器学会肺生理専門委員会編集. 臨床呼吸機能検査 第7版. 東京: メディカルレビュー社, 2008;224-245.
文中引用 「肥満者の全てがOSASを発症する訳ではない。種々の要因によりもともと上気道の狭い者が肥満するとOSASを発症するのである。」
Namyslowski G, Scierski W, Mrowka-Kata K, et al. Sleep study in patients with overweight and obesity. J Physiol Pharmacol2005;56 Suppl 6:59-65.
肥満患者における睡眠研究パラメーター
Obstructive sleep apnea syndrome (OSAS) is a disorder characterized by repetitive collapse of the pharyngeal airway during sleep, which leads to oxygen desaturation, sleep fragmentation and daytime somnolence. Obesity is one of the most important risk factor for the development of OSAS. The exact mechanisms responsible for the relationship between obesity and OSAS are still unclear. The fat deposits in the pharynx region as well as the reduction in the lung volume have been considered as factors that might be responsible for the increase of the upper airway collapsibility. The aim of our study was to evaluate the correlation between the Body Mass Index (BMI) and sleep study parameters in overweight and obese patients suffering from breathing disturbances during sleep. In all cases, BMI and sleep studies (PolyMESAM) were examined. We evaluated relationship between the BMI and sleep study parameters such as Respiratory Disturbance Index (RDI), Apnea Index (AI), Desaturation Index (DI) and Average of Lowest Saturation (LSAT). The results showed the lack of significant statistical correlations between BMI and all the sleep parameters studied in the overweight patients and the statistical positive correlation between the BMI and RDI in the obese cases. We conclude that BMI determination may be considered as a simple, yet important predictor, of the OSAS in the group of obese patients.
コメント:BMI値は、肥満患者のOSAS評価として予測ほど重要な決定因子ではない(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
Peppard PE, Young T, Palta M, et al. Longitudinal study of moderate weight change and sleep-disordered breathing. JAMA2000;284:3015-3021.
体重変化と睡眠呼吸障害との関連についての縦断研究
CONTEXT: Excess body weight is positively associated with sleep-disordered breathing (SDB),a prevalent condition in the US general population. No large study has been conducted of the longitudinal association between SDB and change in weight. OBJECTIVE: To measure the independent longitudinal association between weight change and change in SDB severity. DESIGN: Population-based, prospective cohort study conducted from July 1989 to January 2000. SETTING AND PARTICIPANTS: Six hundred ninety randomly selected employed Wisconsin residents (mean age at baseline, 46 years; 56% male) who were evaluated twice at 4-year intervals for SDB. MAIN OUTCOME MEASURES: Percentage change in the apnea-hypopnea index (AHI; apnea events + hypopnea events per hour of sleep) and odds of developing moderate-to-severe SDB (defined by an AHI > or =15 events per hour of sleep), with respect to change in weight. RESULTS: Relative to stable weight, a 10% weight gain predicted an approximate 32% (95% confidence interval [CI], 20%-45%) increase in the AHI. A 10% weight loss predicted a 26% (95% CI, 18%-34%) decrease in the AHI. A 10% increase in weight predicted a 6-fold (95% CI, 2.2-17.0) increase in the odds of developing moderate-to-severe SDB. CONCLUSIONS: Our data indicate that clinical and public health programs that result in even modest weight control are likely to be effective in managing SDB and reducing new occurrence of SDB.
コメント:体重が10%増えるとAHI(無呼吸-低呼吸指数)>15/hになるオッズ比が6.0になり、20%増えると36.6にも増大する(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
Ryan CF, Love LL. Mechanical properties of the velopharynx in obese patients with obstructive sleep apnea. Am J Respir Crit Care Med1996;154:806-812.
OSAを示す肥満患者における後咽頭のメカニクス特性について
Epidemiologic data indicate that the relationship between obesity and obstructive sleep apnea (OSA) is largely explained by variation in neck size. Fat deposits in the neck may predispose to upper airway (UA) occlusion during sleep by altering the mechanical properties of the UA, particularly at the level of the velopharynx (VP). To determine whether effective compliance (CEFF) of the VP is related to obesity in the neck, we have performed anthropometrics, polysomnography, and dynamic UA videoendoscopy in 18 patients with OSA and eight nonapneic control subjects. Following topical anesthesia (cocaine 4%) to one nasal passage, subjects were examined with a thin fiberscope (outer diameter [OD] 3.8 mm) while awake, supine, breathing exclusively through the nose, during a maximal vital capacity (VC) maneuver against an unoccluded airway. UA cross-sectional area (CSA), anteroposterior (AP) and lateral (L) diameters were measured from stored images. CEFF was expressed as the ratio of CSAVP in expiration (E) to inspiration (I) during the maximal VC maneuver (expiratory CSAMAX/inspiratory CSAMIN), and airway shape as AP/L diameter. The OSA patients were divided into two groups based on median neck circumference (NC). CEFF of the VP was greater in OSA patients compared with control subjects (CEFF 2.0 +/- 0.8 versus 1.1 +/- 0.5; p < 0.001). CEFF was greater in the large NC group compared with both the small NC group (p < 0.05) and control subjects (p < 0.01), but the difference between the small NC group and control subjects was not significant. CEFF was related to NC (r = 0.63; p = 0.001; n = 26), body mass index (r = 0.54; p < 0.01, n = 26), and apnea-hypopnea index (r = 0.43; p < 0.05; n = 23). The change in CSAVP during the maximal VC maneuver was mainly due to inspiratory narrowing. Obese patients with large necks have a more collapsible velopharynx during wakefulness, which may predispose to upper airway obstruction during sleep.
コメント:首回りが太い肥満患者では、覚醒期でも後咽頭は虚脱しやすく、それは睡眠時の上気道閉塞を生じやすいことを示唆するものである(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
Horner RL, Mohiaddin RH, Lowell DG, et al. Sites and sizes of fat deposits around the pharynx in obese patients with obstructive sleep apnoea and weight matched controls. Eur Respir J1989;2:613-622.
OSAS肥満患者と非OSAS肥満患者における咽頭周囲の脂肪沈着の部位と量の比較
It has been suggested that deposition of fat in the soft tissues surrounding the upper airway may be an important factor in the pathogenesis of obstructive sleep apnoea (OSA) in obese subjects. We have used magnetic resonance imaging to determine the site(s) and size(s) of fat deposits around the upper airway in six obese patients with OSA (116-153% of ideal body weight) and five weight-matched controls without OSA (107-152% of ideal body weight). In all subjects, large deposits of fat were present postero-lateral to the oropharyngeal airspace at the level of the soft palate. Significantly more fat was present in these regions in the patients with OSA (p = 0.03). Fat deposits in the soft palate were observed in 4 of the 6 patients with OSA but none of the controls. Fatty streaks were observed in the tongue in 2 of the 5 controls and 3 of the 6 patients with OSA. Fat deposits were observed anterior to the laryngopharyngeal airspace, in submental regions, in all obese subjects. This study shows that more fat is present in those areas surrounding the collapsible segment of the pharynx in patients with OSA, compared to equally obese control subjects without OSA.
コメント:MRI検査にて、肥満でOSASと診断された患者(n=6)には、同じ肥満で非OSASの患者(n=5)に比べ上気道への脂肪沈着が高度であった。軟口蓋への脂肪沈着はOSASのみにみられ、喉頭咽頭より前の顎下領域への脂肪沈着はOSAS患者に特徴的であった(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
Lopata M, Onal E. Mass loading, sleep apnea, and the pathogenesis of obesity hypoventilation. Am Rev Respir Dis1982;126:640-645.
体脂肪、睡眠時無呼吸と、肥満低換気症候群の病因との関係
To define the roles of mechanical loading, respiratory neuromuscular control, and sleep apnea in the pathogenesis of obesity hypoventilation, respiratory muscle drive and output, assessed by diaphragmatic electromyogram (EMGdi) and mouth occlusion pressure (P 0.15), respectively, were determined during CO2 chemostimulation in nonobese volunteers who were subjected to abdominal mass loading, and in three groups of markedly obese patients: eucapnic obese without sleep apnea (O), eucapnic obese with sleep apnea (OSA), and hypercapnic obese with sleep apnea (OH). The P0.15 responses were decreased in OSA and OH, but the EMGdi responses were not significantly different from those in control subjects. In O patients EMGdi responses were significantly greater than those in control subjects as well as those in OSA and OH patients. EMGdi and P0.15 responses increased in all nonobese subjects when they were subjected to mass loading. We conclude that both OSA and OH patients were equally unable to develop the expected increase in respiratory muscle drive and output. The presence of sleep apnea, possibly by causing nocturnal hypoxemia and/or sleep fragmentation, may result in impaired mass load compensation and predispose obese patients to develop hypercapnia.
コメント:肥満低換気症候群(OHS)では、低O2換気応答、高CO2換気応答とも抑制されているが、気管切開やCPAPなどの治療により正常化することから、低酸素血症や高炭酸ガス血症、呼吸筋疲労などが関与して二次的に発生したものと考えられている(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
肥満と咽頭気道(犬)
Pereira-Neto GB, Brunetto MA, Oba PM, et al. Weight loss improves arterial blood gases and respiratory parameters in obese dogs. J Anim Physiol Anim Nutr (Berl) 2018;102:1743-1748.
肥満犬において減量は動脈血ガス分析と呼吸パラメーターを改善する
Canine obesity is a common medical disorder and a known risk factor for associated diseases; it can seriously influence various physiological functions, thereby limiting the longevity of the animal. In this study, we evaluated potential respiratory alterations in obese dogs before and after being subjected to caloric restriction to decrease their body weight by 20%, and compared those dogs with control dogs with ideal body condition score. The animals were divided into three experimental groups: GI (obese dogs; n = 11); GII (obese dogs after weight loss, same animals as in GI); GIII (control dogs; n = 11). We evaluated lung function by spirometry and arterial blood gases. Statistical analysis included paired or non-paired Student’s t test. Compared with dogs within an ideal body condition score (GIII), obese dogs (GI) had a low arterial partial pressure of oxygen (p < 0.05); decreased tidal volume (p < 0.005), inspiratory time and expiratory time (p < 0.05); and an increased respiratory rate (p < 0.005). After losing weight (GII), no differences with control dogs (GIII) were verified. The results suggested that obese dogs have an improvement in respiratory function with weight loss, but further investigations in a larger group of dogs are advised to confirm these findings.
コメント:11頭の肥満犬と11頭の理想体重犬についてスパイロメトリーと動脈血ガス分析値を比較したレトロスペクティブな調査。理想体重犬に比べ肥満犬ではPaO2と一回換気量の低下、吸気時間と呼気時間及び呼吸数の増加が認められた。肥満犬を-20%の体重減量を行うと、各パラメーターで理想体重犬との有意差は認められなくなった。肥満犬は体重減量により呼吸機能の改善が認められることが示唆される(犬・猫の呼吸器科 稲葉健一-2019.5.6)。
PubMed検索
Upper Airway, fat deposits: 12 refs
Upper Airway, fat deposits, dog: 0 refs
Upper Airway, fat deposits, veterinary: 0 refs
肥満犬の上気道への脂肪沈着との関連を示した学術論文は獣医学では見当たらなかった(検査日:2018.10.31)。以下、逸話的記述をまとめた。
Hendrick JC. Sleep Disorders In: Ettinger SJ,Feldman EC, eds. Textbook of Veterinary Internal Medicine. 6th ed. St. Louis, MO: Elsevier Saunders, 2005;176-181.
Similar signs as BAS associated sleep apnea have been described by owners of Shar Peis, pugs, beagles, and an obese, hypothyroid miniature poodle with obvious upper airway narrowing due to fat accumulation. This anecdotal evidence suggests that sleep apnea exists in several canine breeds.
コメント:脂肪沈着によって明らかに上気道の狭窄が生じている犬では、BASと同様に睡眠時無呼吸が生じることが飼い主たちからは確認されている。このようなまだ報告されていない情報ではあるが、いくつかの犬種では睡眠時無呼吸が生じるようである、と記載していた(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Remillard RL. Obesity In: Ettinger SJ,Feldman EC, eds. Textbook of Veterinary Internal Medicine. 6th ed. St. Louis, MO: Elsevier Saunders, 2005;76-78.
コメント:肥満動物では、呼吸困難やうっ血性心不全がよく認められる。BCS 4-5/9の犬は、同じように生活し同じ食事を食べているBCS 6-7/9の犬より、15%長生きした、と記載していた(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Kuehn NF. Chronic Bronchitis in Dogs In: King LG, ed. Textbook of Respiratory Disease in Dogs and Cats. St.Louis: SAUNDERS, 2004;379-387.
コメント:犬の慢性気管支炎では、肥満をよく伴い、その慢性咳のコントロールには体重管理を考慮すべきと考えられる、と記載していた(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Mason RA. Tracheal hypoplasia In: King LG, ed. Textbook of Respiratory Diseases in Dogs and Cats. St.Louis: SAUNDERS, 2004;356-359.
コメント:気管低形成の補助療法として肥満犬には減量が有効であるかもしれない、と記載していた(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Hawkins EC. Pulmonary parenchymal diseases In: Ettinger SJ,Feldman EC, eds. Textbok of Veterinary Internal Medicine. 5th ed. Philadelphia, 2000;1061-1091.
”The benefical effects of weight reduction in animals with chronic bronchial or pulmonary disease can be dramatic.”
コメント:人の「肥満低換気症候群(obesity-hypoventilation syndrome, OHS)=Pickwickian Syndrome」と関連付けて、肺実質疾患と肥満との関連について経験的に記載していた(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
Wolfsheimer KJ. Obesity In: Ettinger SJ,Feldman EC, eds. Textbok of Veterinary Internal Medicine. 5th ed. Philadelphia, 2000;70-72.
コメント:「肥満とは、ある動物種や性別や種類の適正体重より10-20%以上である場合をいう。肥満動物では、胸郭内脂肪沈着と腹部脂肪による横隔膜の前方変位によって肺の大きさが制限されるので、肺気量が減少する。さらに過度な脂肪は、酸素需要や心拍出量が増加し、これが既存の肺疾患を悪化させる。」と記載していた(犬・猫の呼吸器科 城下幸仁-2018.11.28)
短頭種気道症候群への外科療法 外科適応基準と術式選択、非外科適応の判断
Tarricone J, Hayes GM, Singh A, et al. Development and validation of a brachycephalic risk (BRisk) score to predict the risk of complications in dogs presenting for surgical treatment of brachycephalic obstructive airway syndrome. Vet Surg 2019;48:1253-1261. doi: 10.1111/vsu.13291
OBJECTIVE: To develop and validate a preoperative brachycephalic risk (BRisk) score that objectively and accurately predicts the risk of major complications or death in dogs undergoing corrective surgery for brachycephalic obstructive airway syndrome (BOAS). STUDY DESIGN: Retrospective multicenter cohort study. SAMPLE POPULATION: Score development n = 233 dogs, validation n = 50 dogs. METHODS: Data were collected on signalment, medical history, reason for presentation, physical examination, and preoperative diagnostic findings. The primary outcome measures included risk of major complications (requirement for postoperative oxygen support for >48 hours or postoperative temporary/permanent tracheostomy) or death within the hospitalization period. The score was developed by using data from two centers and was validated in a third center. The 10-point BRisk score was modeled on breed, history of previous surgery, concurrent procedures, body condition score, airway status, and admission rectal temperature. RESULTS: The score was associated with negative outcome (P < .0001) and discriminated well in both the construction (area under the receiver operator characteristic [AUROC] = 0.83) and validation groups (AUROC = 0.84). Dogs with scores >3 were 9.1 times more likely to have a negative outcome (95% CI = 3.9-21.2) compared with dogs with scores </=3. CONCLUSION: The BRisk score developed from admission data in this study accurately rated the risk of negative outcome of dogs undergoing corrective surgery for BOAS. CLINICAL SIGNIFICANCE: Preoperative determination of the BRisk score may assist triage, management of owner expectations, decision making regarding intervention selection, and characterization of populations in clinical research.
コメント1:2施設233例でBOASの手術成績の予後不良因子(術後48時間以上の酸素投与、気管切開、永久気管開口術実施)を解析し、BRiskスコアを作成した。その後1施設で50例でそのスコアを検証したところ、BRisk>3では<3と比較して、術後の合併症あるいは死亡が起こるリスクが9.1倍であった。BRiskは品種、今までの外科的上気道整復歴、手術時追加処置、BCS、来院時の呼吸状態、来院時の体温で10点満点で簡便にスコア化できるため(本文参照)、インフォームドコンセント等に有用なツールである(ぬのかわ犬猫病院 布川智範-2019.11.12)。
コメント2:短頭種閉塞性気道症候群の外科手術を行った犬において、術後の合併症を予測するために、同手術を行った233頭から6項目で構成されるBRisk スコアを作成し、他施設の50頭において検証を行った回顧的研究。負の転帰(主要な合併症および死亡)に対して、スコア4を超えるとハイリスクとしている(いいのペットクリニック 飯野亮太-2020.5.5)。
城下幸仁. 短頭種気道症候群の治療 病態生理に基づく周術期管理と術式選択. 日本獣医麻酔外科学雑誌 2016;47:104-107.
コメント:喉頭虚脱ステージ3は永久気管切開術選択の理由にはならない(犬・猫の呼吸器科 城下幸仁-2018.11.28)。
Findji L, Dupre G. Folded flap palatoplasty for treatment of elongated soft palates in 55 dogs. Vet Med Austria 2008;95:56-63.
軟口蓋過長の犬55頭の治療に対する折り畳み弁口蓋形成術
It was the aim of the present study to evaluate the safety and efficacy of the folded flap palatoplasty (FFP), a new surgical technique addressing all components of the respiratory obstruction caused by elongated soft palates, and to evaluate the clinical outcomes associated with it. Medical records (2004-2005) of all dogs which underwent a FFP were reviewed and included in the study. Recorded information included breed, gender, age, body mass, duration of hospitalisation, and presence or absence of postoperative tracheostomy. Respiratory grading scores (1-3) were used to record the severity of the disease, before and after surgery, and at a minimum follow-up time of 180 days by detailed telephone interviews with the owners. No intraoperative complications were encountered. A temporary tracheostomy was performed in 6 cases (10.9.%). 2 dogs died postoperatively from tracheostomy complications and unknown cause after unremarkable recovery, respectively.Follow-up (379 ± 142 days) could be obtained for 40 dogs. 39 dogs (97.5 %) showed improvement of respiratory clinical signs after surgery. Improvement of respiratory clinical signs was observed within 15 days after surgery in 85 % of the cases. The FFP can be recommended as a safe and efficient technique, particularly valuable for excessively thick elongated soft palates.
コメント1:軟口蓋を短縮および減量する、折り畳み弁口蓋形成術(FFP)は、術後に呼吸器症状の評価スコアを有意に改善させた(いいのペットクリニック 飯野亮太-2020.6.22)。
BASの臨床評価は、Poncet CM, Dupre GP, Freiche VG, et al. Prevalence of gastrointestinal tract lesions in 73 brachycephalic dogs with upper respiratory syndrome. J Small Anim Pract 2005;46:273-279.の分類(いびき、吸気努力、運動不耐性、失神の各呼吸器症状の頻度からグレード1-3と設定)を用いている。
非外科適応群に対する温存対処法としてのネブライザー療法の効果
掲載準備中
中耳炎との関連
「キャバリアの原発性分泌性中耳炎」あるいは「キャバリアの浸出性中耳炎」
青木忍. 外耳・中耳からみた短頭種気道症候群. 動物臨床医学会年次大会プロシーディングno.1. 2018 :23-26.
コメント:短頭犬種の骨格形態や努力呼吸時の咽頭閉塞は、耳管の走行障害や開口部閉塞と関連し浸出性中耳炎を生じやすいと考えられる。また、さらにそれが進行すると真珠腫性中耳炎となり、外科手術でも再発しやすく難治化するかもしれない。(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Harcourt-Brown TR, Parker JE, Granger N, et al. Effect of middle ear effusion on the brain-stem auditory evoked response of Cavalier King Charles Spaniels. Vet J2011;188:341-345.
キャバリアの中耳内浸出液の脳幹聴覚誘起反応に対する影響
Brain-stem auditory evoked responses (BAER) were assessed in 23 Cavalier King Charles Spaniels with and without middle ear effusion at sound intensities ranging from 10 to 100 dB nHL. Significant differences were found between the median BAER threshold for ears where effusions were present (60 dB nHL), compared to those without (30 dB nHL) (P=0.001). The slopes of latency-intensity functions from both groups did not differ, but the y-axis intercept when the x value was zero was greater in dogs with effusions (P=0.009), consistent with conductive hearing loss. Analysis of latency-intensity functions suggested the degree of hearing loss due to middle ear effusion was 21 dB (95% confidence between 10 and 33 dB). Waves I-V inter-wave latency at 90 dB nHL was not significantly different between the two groups. These findings demonstrate that middle ear effusion is associated with a conductive hearing loss of 10-33 dB in affected dogs despite the fact that all animals studied were considered to have normal hearing by their owners.
コメント:中耳内浸出液貯留が認められたキャバリアでは聴覚障害があるようだ(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Hayes GM, Friend EJ, Jeffery ND. Relationship between pharyngeal conformation and otitis media with effusion in Cavalier King Charles spaniels. Vet Rec2010;167:55-58.
キャバリア・キング・チャールズの咽頭構造と中耳内浸出液との関連
Otitis media with effusion (OME) is a common incidental finding in otherwise normal Cavalier King Charles spaniels (CKCS). In this study, measurements made on MRI were used to determine whether there was an association between OME and brachycephalic conformation. The results confirm that association and also demonstrate that, in CKCS, greater thickness of the soft palate and reduced nasopharyngeal aperture are significantly associated with OME. These results suggest that auditory tube dysfunction and OME may represent a previously overlooked consequence of brachycephalic conformation in dogs.
コメント:軟口蓋の著しく肥厚し、鼻咽頭が狭くなっているキャバリアに中耳内浸出液の増加があるようだ(犬・猫の呼吸器科 城下幸仁-2018.11.28)
Stern-Bertholtz W, Sjostrom L, Hakanson NW. Primary secretory otitis media in the Cavalier King Charles spaniel: a review of 61 cases. J Small Anim Pract2003;44:253-256.
キャバリア・キング・チャールズの原発性分泌性中耳炎61例
Sixty-one episodes of primary secretory otitis media (PSOM) were diagnosed in 43 Cavalier King Charles spaniels over a 10-year period. The principal findings were signs of moderate to severe pain localised to the head or cervical area, and/or neurological signs. Diagnosis was made by examination of the tympanic membrane and middle ear with the aid of an operating microscope under general anaesthesia. A bulging, but intact, tympanic membrane was found in most cases. Following myringotomy, a highly viscous mucus plug was found filling the middle ear. Treatment, consisting of removal of the mucus plug, flushing of the middle ear, and local and systemic medical therapy, had to be repeated between one and five times. The prognosis was good in all cases. PSOM is an important differential diagnosis in Cavalier King Charles spaniels with signs of pain involving the head and neck, and/or neurological signs.
コメント:キャバリアには特発性に中耳内に浸出液が貯留する疾患があるようです。痛みや神経症状と伴い、耳鏡手術を繰り返して治療します(犬・猫の呼吸器科 城下幸仁-2018.11.28)
気管切開
全般
掲載準備中
一時的気管切開(Temporary tracheotomy)
Stordalen MB, Silveira F, Fenner JVH, et al. Outcome of temporary tracheostomy tube-placement following surgery for brachycephalic obstructive airway syndrome in 42 dogs. J Small Anim Pract 2020;61:292-299.
犬の短頭種閉塞性気道症候群42頭に対する術後の一時的気管切開チューブ設置の結果
OBJECTIVES: To describe the use, complications and outcome of temporary tracheostomy tube placement as part of the management of acute upper airway obstruction in the postoperative period following multi-level airway surgery in patients with brachycephalic obstructive airway syndrome. MATERIALS AND METHODS: Retrospective review of records of dogs surgically treated for brachycephalic obstructive airway syndrome that had a temporary tracheostomy tube placed in the postoperative period. RESULTS: Forty-two dogs were included. Median duration of temporary tracheostomy tube placement was 2 days (range 1 to 7). The major complication rate was 83.3%, minor complication rate was 71.4%, resulting in an overall postoperative complication rate of 95.2%. The most common postoperative complications were tracheostomy tube obstruction (32/42), cough (25/42) and tracheostomy tube dislodgement (16/42). Temporary tracheostomy tube management was classified as successful in 97.6%. Dyspnoea was the most common clinical sign in the short-term postoperative follow-up period, while dyspnoea and increased upper respiratory tract noise were the most common clinical sign in the long term. The median duration of follow-up was 251 days. CLINICAL SIGNIFICANCE: In an appropriate clinical setting, placement of temporary tracheostomy tubes following multi-level airway surgery for brachycephalic obstructive airway syndrome is a useful strategy to manage postoperative airway obstruction, carrying a low mortality rate, and with a complication rate similar to that found in previous reports.
コメント1:BAOS術後の一時的気管切開チューブ(TTT)設置の合併症率は高く、最も一般的なものとしてチューブの閉塞や滑落が挙げられるが、死亡率は低く術後の気道閉塞を管理する方法として有用である。イングリッシュブルドックにおいても、他犬種と同等の結果であった。(いいのペットクリニック 飯野亮太-2020.6.22)
コメント2:CLINICAL SIGNIFICANCEの和訳「適切な臨床環境であれば、短頭種気道症候群に対する複数手技を組み合わせた上気道整復術後に(ルーチーンとして行う)一時的気管切開チューブ設置は有用な治療手段である。なぜなら、合併症率は既報と同等であり、低い死亡率で術後気道閉塞を管理できるからである(術後生存率が高めると考えられる)。」(犬・猫の呼吸器科 城下幸仁-2020.6.23)
コメント3:一時的気管切開チューブ設置は術後気道閉塞の発生リスクを軽減するのに有効であったと結論付けている(大樹どうぶつ病院 福田大介-2020.2.23)。
Worth DB, Grimes JA, Jimenez DA, et al. Risk factors for temporary tracheostomy tube placement following surgery to alleviate signs of brachycephalic obstructive airway syndrome in dogs. J Am Vet Med Assoc 2018;253:1158-1163.
短頭種気道症候群における一時的気管切開術のリスクファクター
OBJECTIVE To identify risk factors for temporary tracheostomy tube placement (TTTP) following surgery for alleviation of signs associated with brachycephalic obstructive airway syndrome (BOAS) in dogs. DESIGN Retrospective case-control study. ANIMALS 122 client-owned dogs with BOAS that underwent surgery to alleviate clinical signs (BOAS surgery). PROCEDURES The medical records database of a veterinary teaching hospital was searched to identify dogs that underwent BOAS surgery from January 2007 through March 2016. Of the 198 dogs identified, 12 required postoperative TTTP (cases); 110 of the remaining 186 dogs were randomly selected as controls. Data regarding signalment and select preoperative, intraoperative, and postoperative variables were extracted from the medical record of each dog. Variables were compared between cases and controls and evaluated for an association with the odds of postoperative TTTP. RESULTS Body condition score, tracheal diameter-to-thoracic inlet ratio, staphylectomy technique, and mortality rate did not differ significantly between cases and controls. The odds of postoperative TTTP increased approximately 30% (OR, 1.3) for each 1-year increase in patient age. Postoperative administration of corticosteroids and presence of pneumonia were also positively associated with the odds of postoperative TTTP. Median duration of hospitalization was significantly longer for cases than controls. CONCLUSIONS AND CLINICAL RELEVANCE Age was positively associated with the odds of TTTP in dogs after BOAS surgery, and TTTP led to prolonged hospitalization. Thus, early identification and intervention may be beneficial for dogs with BOAS. The associations between TTTP and postoperative corticosteroid use or pneumonia were likely not causal, but reflective of patient disease severity.
コメント:短頭種気道症候群の犬に対して、症状緩和のための手術(軟口蓋切除、鼻孔狭窄の矯正、喉頭小嚢の切除)を実施後、一時的気管切開が必要となった群とコントロール群の危険因子を検討した後ろ向き研究。患者の年齢が増加するごとに気管切開のオッズは上昇し、気管切開群はコントロール群と比べて入院も延長した。年齢とともに上気道の軟部組織の弾性低下が示唆されているが、術前の評価はなし。(いいのペットクリニック 飯野亮太-2019.6.21)
コメント:BAS整復手術時に一時的気管切開術(TTTP)を受けた短頭種12頭と、受けていない110頭を後ろ向きに比較した論文。TTTP群における肺炎の合併は、リスクファクターとなると考察している(まるふく動物病院 福田大介-2020.1.14)。
Bird FG, Vallefuoco R, Dupre G, et al. A modified temporary tracheostomy in dogs: outcome and complications in 21 dogs (2012 to 2017). J Small Anim Pract 2018;59:769-776.
OBJECTIVES: To describe a modified temporary tracheostomy that included placing a Penrose drain sling dorsal to the trachea. To report outcomes and complications in brachycephalic versus non-brachycephalic breeds. MATERIALS AND METHODS: Retrospective review of signalment, diagnosis, outcome, complications and management of dogs that underwent modified temporary tracheostomy. RESULTS: Twenty-one dogs were included. Tracheostomy tubes were maintained for periods ranging from 1 to 21 days (median 4 days). There were no intraoperative complications or complications related to the placement of the Penrose drain. Postoperative complications occurred in eight dogs, including dislodgement of the tracheostomy tube (n=6), obstruction of the tracheostomy tube (n=1), subcutaneous emphysema and pneumomediastinum (n=1). Twenty dogs survived until discharge; one was euthanised due to persistence of primary disease. The complication rate in brachycephalic breeds and non-brachycephalic was 375 and 40%, respectively. Tube dwell duration of 4 days or longer was associated with a higher complication rate. CLINICAL SIGNIFICANCE: The modified temporary tracheostomy appears to simplify tracheostomy care, improve tracheostomy outcome and reduce tube-associated mortality compared with standard tracheostomy. In this study, brachycephalic dogs did not have a higher complication rate than non-brachycephalic dogs.
コメント:21頭(短頭種16、非短頭種5)において変更型一時的気管切開術を行った前向き研究である。従来の一時的気管切開術との変更点は二点で、ペンローズドレーンを気管背側に設置することにより、気管の腹側挙上効果を得ることと、気管瘻孔部の前後気管輪を垂直方向切開を加えることによりフラップ形成する、H字型気管切開である。本研究では周術期合併症(皮膚による瘻孔狭窄、気管低形成による気道狭窄、チューブ脱落、気腫)が21頭中8頭(38%)で発生し、短頭種6/16頭(37.5%)、非短頭種 2/5頭(40%)であった。変更型一次的気管切開術により、非短頭犬種に比べ、短頭犬種において高率に発生する合併症発生率を有意に減らすことができたと報告している。これは、ドレーンによる気管の腹側化により、皮膚のたるみが起きにくい。H字型気管切開による近位、遠位フラップによりチューブ脱落をおこしたあとも気道閉塞が起きにくいのではと考察されている(上大岡キルシェ動物病院 山下智之-2019.8.27)。
関瀬利, 関真美子, 萩原聡子ら. 頸部オンコサイトーマによる陰圧性肺水腫が示唆され、陽圧換気と永久気管開口術で救命した犬の一例(Positive Pressure Ventilation and Permanent Tracheostomy to Treat Suspected Negative Pressure Pulmonary Edema Related to Cervical Oncocytoma in a Dog). 日本獣医麻酔外科学雑誌 2015;46:1-5.
頸部のオンコサイトーマと診断された10歳齢の避妊雌のスピッツが腫瘤再発の精査のために紹介来院した。胸部X線検査で肺水腫が確認され、症例はその検査時に重度の呼吸困難を呈し始めた。挿管し、陽圧換気と呼気終末陽圧を実施したところ、第2病日後に肺野の浸潤陰影が消失した。頸部腫瘤に関連した陰圧性肺水腫が示唆され、切除不可能な腫瘤によって生じた上部気道狭窄を緩和するために永久気管開口術が実施された。犬は第13病日に退院し、術後312日まで生存した。
コメント:経口気管内挿管後PPV管理を行い、肺水腫改善後に永久気管切開術が実施された症例の報告(まるふく動物病院 福田大介-2020.1.14)。
Hansen IK, Eriksen T. Cricothyrotomy: possible first-choice emergency airway access for treatment of acute upper airway obstruction in dogs and cats. Vet Rec 2014;174:17.
輪状甲状靭帯切開:犬と猫の急性上気道閉塞の治療に対する緊急気道アクセスの第一選択の可能性
犬猫における輪状甲状靭帯切開のレビュー。ニードル輪状甲状靭帯切開と外科的輪状甲状靭帯切開の手技、合併症について紹介しており、早くて簡便、安全な点において気管切開に変わる方法として提案されている(いいのペットクリニック 飯野亮太-2020.1.27)
Trinterud T, Nelissen P, White RA. Use of silicone tracheal stoma stents for temporary tracheostomy in dogs with upper airway obstruction. J Small Anim Pract 2014;55:551-559.
犬の上気道閉塞に対する、シリコン製の気管ストーマを用いた一時気管切開術
OBJECTIVES: To report the use of silicone tracheal stoma stents for temporary tracheostomy in dogs with upper airway obstruction. METHODS: Retrospective review of medical records for dogs in which silicone tracheal stoma stents were placed. RESULTS: Eighteen dogs had a silicone tracheal stoma stent placed for maintenance of a tracheostomy stoma for periods ranging from three hours to eight months. No intra-operative or immediate postoperative complications were recorded. In 11 dogs the stent was removed by simple traction after a period ranging from 36 hours to 6 weeks, and the tracheal stoma was left to heal by second intention. Five of the 18 dogs were determined as being tracheostomy dependent and underwent conversion to permanent tracheostomy after a period ranging from five days to eight months following stent placement. One dog was euthanased after three months, with the stent still in place, because of poor respiratory function, and one dog died of unrelated reasons. In 6 of 10 dogs (60%) where the stent was in place for five days or more, granulation tissue formation caused dislodgement of the stent. CLINICAL SIGNIFICANCE: Silicone tracheal stoma stents may be used as an alternative to conventional tracheostomy tubes in selected dogs with upper airway obstruction. Long-term use of the stent beyond five days is not recommended because of granulation tissue formation. The long-term consequences of partial tracheal ring resection are unknown.
コメント:18頭の犬に対する後ろ向き研究。周術期の合併症の記載はない。著者は従来の気管切開チューブの代替として使用可能と評価している。5日を超える留置は肉芽組織形成のリスクがあるため、推奨していない(まるふく動物病院 福田大介-2019.8.18)。
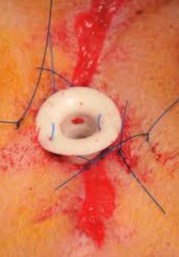
Mazzaferro EM. Temporary tracheostomy. Top Companion Anim Med 2013;28:74-78.
一時的気管切開
Upper airway obstruction can be due to a variety of causes in small animal patients and is often life threatening if left untreated. Placement of a temporary tracheostomy tube may be necessary in the most severe cases of upper airway obstruction until definitive therapy can be implemented. This paper discusses the indications, technique for placement, maintenance, and complications associated with temporary tracheostomy in dogs and cats.
コメント:一時的気管切開に関する適応、手技、メンテナンス、合併症についてのレビュー。ニードル輪状甲状靭帯切開は、一時的気管切開までの酸素投与方法として紹介されている。一時的気管切開の一般的な合併症として気管の脆弱や虚脱、重篤な合併症として、ホルネル症候群、喉頭麻痺が挙げられている(いいのペットクリニック 飯野亮太-2020.1.27)。
Nicholson I, Baines S. Complications associated with temporary tracheostomy tubes in 42 dogs (1998 to 2007). J Small Anim Pract 2012;53:108-114.
42頭の犬における一時気管切開チューブの合併症
OBJECTIVE: To identify the type and frequency of tracheostomy tube complications, and to determine factors associated with these complications, and with poor outcome. METHODS: A database search for dogs undergoing temporary tube tracheostomy was performed. The medical records were scrutinised. The signalment, respiratory disease history, diagnosis, surgery, type and frequency of tube care procedures, type of complications and outcome were recorded. RESULTS: Forty-two records were found. Complications occurred in 36 of 42 (86%) cases. Bulldogs were more likely to dislodge the tube than other breeds (P=0.0376), and cases with three or more complication types underwent more routine care procedures than those with fewer complications (P=0.0370). Thirty-four of 42 (81%) dogs had a successfully managed tracheostomy tube and survived until tube removal, or elective euthanasia without significant tube complications. Bulldogs were also significantly (P=0.0376) more likely to have an unsuccessful tube outcome, as were dogs experiencing severe bradycardia during treatment (P=0.0176). Dogs with unsuccessful tube outcome were significantly (P=0.0331) younger than dogs with successful tube outcome. CLINICAL SIGNIFICANCE: Tracheostomy tubes in dogs have a high complication rate but a good outcome in most dogs. Careful management may improve the outcome of dogs with tracheostomy tubes, especially bulldogs and dogs exhibiting bradycardia during treatment.
コメント:一時気管切開チューブを設置された犬42頭についての後ろ向き研究。86%の症例でなんらかの合併症が認められたが、81%の症例で死亡することなくチューブを抜去することができた。ブルドッグや、治療中に重度徐脈が認められた症例では、より重篤な合併症が生じる傾向があったため、これらの症例ではさらに注意深い管理が必要となる(まるふく動物病院 福田大介-2019.3.4)
Mercurio A. Complications of upper airway surgery in companion animals. Vet Clin North Am Small Anim Pract 2011;41:969-980, vi-vii.
伴侶動物における上気道外科手術の合併症
Surgery of the upper airway is performed in dogs for the correction of brachycephalic airway syndrome and laryngeal paralysis and for temporary or permanent tracheostomy. Although technically simple to perform, upper airway surgeries can lead to the development of significant postoperative complications. This article reviews complications associated with common surgical conditions of the upper airway. It involves a discussion of brachycephalic airway syndrome and associated respiratory and gastrointestinal complications. It also covers laryngeal paralysis with a focus on unilateral arytenoid lateralization and the complication of aspiration pneumonia. The condition of acquired laryngeal webbing/stenosis and potential treatment options is also discussed. Finally, tracheostomies and associated complications in dogs and cats are reviewed.
コメント:BAS、喉頭麻痺、喉頭狭窄、気管切開に関する外科手術の合併症についてのレビュー。永久気管切開術の合併症として、喉頭切開術が実施されなくても、正常な発声能力の喪失が挙げられている(いいのペットクリニック 飯野亮太-2020.1.27)。
Harvey CE, O’Brien JA. Tracheostomy in the dog and cat: analysis of 89 episodes in 79 animals. J Am Anim Hosp Assoc 1982;18:563-566. (PDFあり)
犬・猫の一時的気管切開:79例に対する89処置の解析
Tracheotomy was performed 89 times on 79 dogs and cats at VHUP from 1970 to 1980. Curved metal tubes were placed through a transverse incision between tracheal rings. The most common indication was upper airway obstruction or surgery for upper airway disease. Tube plugging or displacement, gagging, vomiting, and coughing were the most frequent complications. One of two dogs which developed partial tracheal stenosis subsequently died of respiratory obstruction.
コメント:獣医学において一時的気管切開の有用性や合併症を多数の実施症例から解析した最も初期の文献。横切開に金属製気管切開チューブを79例(犬74;猫5)に対し合計89回行なった。上気道閉塞や上気道外科手術に主に行われた。合併症にはチューブ閉塞や滑脱、ギャギング、嘔吐、咳が認められた。気管切開実施例の50%で何らかの合併症が生じたが、管理可能の範囲内であった。この論文の著者は、2例で重大な合併症が生じたが、呼吸困難症例での適用ということを考慮すれば、危険性は低いと結論している。ただし、猫や小型犬での適用には特に注意を要する。概して、術後には十分な観察が必要であることも強調されている。上気道閉塞の呼吸苦から即座に解放される確実かつ唯一の手段であることは明らかであり、適用は避けられない場面があるが、合併症や管理法を熟知すれば臨床的には有用性の高い処置と考えられる(犬・猫の呼吸器科 城下幸仁−2019.1.29)。
永久気管開口術(Permanent tracheostomy)
Grimes JA, Davis AM, Wallace ML, et al. Long-term outcome and risk factors associated with death or the need for revision surgery in dogs with permanent tracheostomies. J Am Vet Med Assoc 2019;254:1086-1093.
永久気管開口術の長期経過観察および死亡または整復術が必要となる危険因子
OBJECTIVE: To evaluate long-term outcomes and identify factors associated with death or the need for revision surgery in dogs with permanent tracheostomies (PTs). DESIGN: Retrospective cohort study. ANIMALS: 69 client-owned dogs that received a PT between January 2002 and June 2016 at 1 of 4 veterinary teaching hospitals. PROCEDURES: Medical records were reviewed, and data extracted included signalment, history, clinical signs, radiographic and laryngeal examination findings, presence of esophageal abnormalities, date and reason for receiving a PT, postoperative complications, cause of death, and survival time. Dogs surviving < 2 weeks after receiving a PT were excluded. RESULTS: Major complications occurred in 42 of 69 (61%) dogs, with aspiration pneumonia (13 [19%]), skinfold occlusion (13 [19%]), and stoma stenosis (12 [17%]) being most common. Revision surgery was performed in 24 of 69 (35%) dogs, most commonly because of stoma stenosis or skinfold occlusion (9/24 [38%] each). Brachycephalic dogs were more likely (OR, 3.5; 95% confidence interval, 1.2 to 10.2) to require revision surgery than were nonbrachycephalic dogs. The overall median survival time was 1,825 days, and dogs that received corticosteroids before receiving a PT, had tracheal collapse, or were older had shorter survival times. CONCLUSIONS AND CLINICAL RELEVANCE: Results of the present study indicated that creation of a PT was a viable treatment option for obstructive upper airway diseases in dogs and that long-term survival after receiving a PT was possible; however, a PT may not reduce the risk of aspiration pneumonia in dogs.
コメント:永久気管開口術を受けた犬における死亡または再手術となるリスクファクターを2002年~2016年の69頭を対象にレトロスペクティブに調査した報告。主な合併症は42/69頭(61%)の犬で発生し、誤嚥性肺炎(19%)、皮膚のたるみによる閉塞(19%)、ろう孔狭窄(17%)であった。短頭種は非短頭種に比べて再手術を必要とする可能性が高かった。生存期間中央値は1825日であったが、術前のステロイド療法、気管虚脱、高齢の要因を持つ症例では生存期間が短かった。永久気管開口術は上気道閉塞に対する有効な治療法であるが、誤嚥性肺炎のリスクを減らすことはできないかもしれない(犬・猫の呼吸器科 稲葉健一-2019.5.6)。
コメント:永久気管開口術の経過を長期に追った貴重な報告である。長期の経過は良好で、術後2週を生存した症例の中央生存値は5年であった。多施設での後ろ向き研究のため、術式や術後のケアが様々であるところにリミテーションはある。気管虚脱の症例は生存期間が短くなっているのは既に気管軟骨の強度が破綻しているためかもしれないので、永久気管開口術ではない方法で気道閉塞を管理する方が良いかもしれない。ステントなどを最初に行えない理由があったのかもしれないが、詳細は不明である。(ぬのかわ動物病院 布川智範-2019.6.8 )
Gobbetti M, Romussi S, Buracco P, et al. Long-term outcome of permanent tracheostomy in 15 dogs with severe laryngeal collapse secondary to brachycephalic airway obstructive syndrome. Vet Surg 2018;47:648-653. doi: 10.1111/vsu.12903
短頭種気道閉塞症候群による重度喉頭虚脱の犬15頭における永久気管開口術の長期転帰
OBJECTIVE: To report the long-term outcome of permanent tracheostomy for the management of severe laryngeal collapse secondary to brachycephalic airway obstructive syndrome. STUDY DESIGN: Retrospective case series. ANIMALS: Fifteen brachycephalic dogs with severe laryngeal collapse treated with permanent tracheostomy. METHODS: Follow-up data were obtained from medical records or via telephone conversation with the owners. The Kaplan-Meier estimator was used to calculate median survival time. Death was classified as related or unrelated to tracheostomy surgery. Complications were classified as major when they were life-threatening or required revision surgery. Owners were asked to classify the postoperative quality of life as improved, unchanged, or worse and the management of the stoma as simple or demanding. RESULTS: The median survival time was 100 days. Major complications were diagnosed in 12 of 15 (80%) dogs, resulting in death in 8 (median survival time 15 days) and revision surgery in 4 dogs. Seven of 15 (47%) dogs died of unrelated causes or were alive at the end of the study (median survival time 1982 days). The postoperative quality of life of 9 dogs was judged as markedly improved. Stoma management was defined as simple in 8 dogs and demanding in 4. CONCLUSION: Permanent tracheostomy was associated with a high risk of complications and postoperative death in brachycephalic dogs. However, long-term survival (exceeding 5 years) with a good quality of life was documented in 5 of 15 dogs. CLINICAL SIGNIFICANCE: Permanent tracheostomy is a suitable salvage option in brachycephalic dogs with severe laryngeal collapse that did not improve following more conservative surgeries.
コメント;BAOSによる喉頭虚脱グレード3の犬15頭に対して永久気管開口術を実施した回顧的研究。標準的外科手術(軟口蓋切除、外鼻孔切除、喉頭小嚢切除)で改善しなかった症例に対して適応。粘液プラグや皮膚皺による閉塞などの重大な合併症が80%で発生し死亡率も高いが、術後20週以内に集中し、その期間を乗り越えた症例の長期予後は良好(いいのペットクリニック 飯野亮太-2019.2.7)。
Davis AM, Grimes JA, Wallace ML, et al. Owner Perception of Outcome Following Permanent Tracheostomy in Dogs. J Am Anim Hosp Assoc 2018;54:285-290.
犬の永久気管開口術に対する飼い主の評価
The purpose of this study was to evaluate owner perception of outcome following permanent tracheostomy (PT) in dogs. Medical records of dogs who received PT from 2002 to 2016 were reviewed. A questionnaire was given to owners verbally or by e-mail to ascertain their perception of their dog’s outcome after PT. Median time to questionnaire administration from PT surgery was 608 days (64-3,708). Owner satisfaction after PT was high (89.7%), with the majority stating they would have the procedure performed again (79.5%). Owners reported an improvement in their dog’s personality (30.8%) and increased activity (41%). Median survival time was 1,825 days (64-2,663), with 6 of 39 dogs (15.4%) alive at study end. Of the 33 dogs who died, 11 (33.3%) died from underlying respiratory conditions suspected to be related to the PT. The overall complication rate was 82.1%, with mucus secretion being the most common. Revision surgery was required in 30.8% of dogs (most commonly due to skin occlusion), and aspiration pneumonia occurred in 17.9% of dogs. Overall, owner satisfaction after PT in dogs is high despite intensive postoperative management, and long survival times can be achieved.
コメント:永久気管開口術を受けた39頭の犬に関する文献。飼い主の満足度は89.7%と高かった。術後中央生存期間(範囲)は1,825日(64~2,663日)であった。合併症の発生が82.1%の症例で認められ、再手術が30.8%で必要であった(まるふく動物病院 福田大介2019.8.18)。
Occhipinti LL, Hauptman JG. Long-term outcome of permanent tracheostomies in dogs: 21 cases (2000-2012). Can Vet J 2014;55:357-360.
21頭の犬の永久気管開口術に関する長期観察
This retrospective study reports long-term outcome, survival, and complications in dogs which received a permanent tracheostomy due to upper airway obstruction. Data were collected from medical records (n = 21) in 2 institutions over a 12-year period. Patients were followed until death, complications, causes of death, and survival times are reported. Major complications were reported in 50% of patients with 20% of patients receiving revision surgery. The most common complications were aspiration pneumonia and need for revision surgery. Median survival time was 328 days with 25% of patients surviving 1321 days or longer. Some (26%) patients died acutely at home at various times after surgery. Permanent tracheostomy is a viable procedure for patients with end stage upper airway obstruction; however, a subpopulation of patients suffers acute death at various times after surgery, which is thought to be due to airway obstruction.
コメント:21症例のうち、50%の犬で何らかの合併症が認められ、20%の犬で再手術が必要となった。中央生存期間は328日で、25%の症例が1,321日以上生存した。26%の症例が退院直後に原因不明で突然死しており、著者は気管開口部の閉塞が原因と推測している(まるふく動物病院 福田大介2019.8.18)。
Stepnik MW, Mehl ML, Hardie EM, et al. Outcome of permanent tracheostomy for treatment of upper airway obstruction in cats: 21 cases (1990-2007). J Am Vet Med Assoc 2009;234:638-643.
猫の上気道閉塞における永久気管切開術21例の転帰(1990-2007)
OBJECTIVE: To determine clinical outcome of permanent tracheostomy in cats with upper airway obstruction. DESIGN: Retrospective case series. ANIMALS: 21 cats. PROCEDURES: Medical records were reviewed for information on history, signalment, clinical signs, results of preoperative clinicopathologic testing, cause of upper airway obstruction, surgical procedure, postoperative complications, and outcome. RESULTS: Causes of upper airway obstruction included neoplasia (squamous cell carcinoma [n = 6] or malignant lymphoma [2]), inflammatory laryngeal disease (5), laryngeal paralysis (4), trauma (3), and a laryngeal mass of unknown cause (1). Fourteen cats had dyspnea in the immediate postoperative period; dyspnea most often resulted from mucous plugs at the stoma or elsewhere in the respiratory tract. Eleven cats died, including 6 cats that died while hospitalized after surgery and 5 cats that died after discharge; 7 cats were euthanatized, most often because of progression of neoplasia; and 2 were still alive at the time of the study. The remaining cat was lost to follow-up after discharge from the hospital. Overall, median survival time for the 20 cats for which information was available was 20.5 days (range, 1 day to 5 years). Cats that underwent permanent tracheostomy because of inflammatory laryngeal disease were 6.61 times as likely to die as cats that underwent permanent tracheostomy for any other reason. CONCLUSIONS AND CLINICAL RELEVANCE: Results indicated that permanent tracheostomy was an uncommon procedure in cats with upper airway obstruction that was associated with high complication and mortality rates.
コメント:多施設後向き研究。6つの米国獣医科大における18年間の臨床記録から21頭の猫に永久気管開口術が実施されていた。経過追跡可能であった20例の生存期間中央値は20.5日、範囲は1日から5年であった。急死の原因は、粘液栓による閉塞を強く疑っている。粘液の由来は喉頭や下気道などの可能性があり限定はされていない。喉頭全摘術、悪性腫瘍、喉頭麻痺は死亡率増加に関連しなかった。炎症性喉頭疾患の猫は他の疾患の猫に比べ、6.61倍死亡率が有意に高かった(95%信頼区間1.50-29.17、P=0.013)。この報告では、炎症性喉頭疾患とは肉芽腫性喉頭炎もしくはリンパ形質性細胞性喉頭炎に限定している。炎症喉頭疾患でなぜ術後死亡率が増加するかの考察はない。もしこれら疾患を疑う場合、永久気管開口術で気道確保せずに、一時的気管切開チューブ設置にて気道確保しつつ内科療法を進めることを強く推奨している。猫には安易に永久気管開口術で上気道閉塞疾患を解決しようとせずに、十分に他の治療オプションを検討するべきであり、時間猶予がなければ一時的気管切開チューブ設置を実施にて上気道閉塞の危機を乗り越えるべきである(犬・猫の呼吸器科 城下幸仁-2020.2.2)。
Guenther-Yenke CL, Rozanski EA. Tracheostomy in cats: 23 cases (1998-2006). J Feline Med Surg 2007;9:451-457.
猫の気管切開術23例(1998−2006)
Tracheostomies can be used to provide a patent airway in animals with upper airway obstruction but have been reported to be more difficult to manage in cats than in other animals. The purpose of this study is to retrospectively describe the indications, complications and outcome of cats undergoing tracheostomy. Twenty-three cats underwent tracheostomy for laryngeal mass (n=13), trauma (n=5) and upper airway swelling (n=5). Major and minor complications were recorded in 10 and 17 cats, respectively. Seventeen cats were discharged to home, four cats were euthanased and two cats died in hospital. Complications with stoma healing were reported in one cat. Of seven cats discharged with a permanent tracheostomy, one cat is alive and six cats survived at home for between 2 and 281 days. Although complications are common, temporary tracheostomies can be beneficial for conditions in which the underlying cause can be treated. Despite risk of occlusion, permanent tracheostomies can be effective palliative procedures for cats with severe upper airway disease.
コメント:7頭の猫で永久気管開口術が行われた。うち3頭は退院後1週間は問題なく過ごしたが、その後短期間で急死した。悪性腫瘍疾患が多く、その場合、生存期間中央値は42日であった。肉芽腫性喉頭炎と診断し喉頭部分切除を行なった猫は例外的に術後1642日以上生存した。著者は、気管開口部閉塞か、基礎疾患による気道分泌物増加で閉塞したと推測している。入院期間中の死亡はなかった。しかし、永久気管開口術は、重度上気道閉塞による苦しみを緩和する手段としては評価しうる、と述べている(犬・猫の呼吸器科 城下幸仁-2020.2.2)。
Hedlund CS, Tangner CH, Montgomery DL, et al. A Procedure for Permanent Tracheostomy and Its Effects on Tracheal Mucosa. Vet Surg 1982;11:13-17. (PDFあり)
永久気管開口術:手技と気管粘膜への影響
Permanent tracheostomies were performed on six dogs which were evaluated clinically and histologically. One dog had abnormal tracheal cartilages and died following tracheal collapse three days postoperatively. Problems with coughing, swallowing, and infection were not noted in the remaining five dogs. The exposed tracheal epithelium temporarily underwent squamous metaplasia but returned to a relatively normal appearance within 16 weeks.
コメント:獣医学において犬の永久気管開口術について複数の症例を提示した最も初期の文献。永久気管開口術の手技の紹介と犬6例の臨床経過を示し、術後16週経過で露出した気管粘膜は安定化することを確認した。現在もこの術式が基本となっている(犬・猫の呼吸器科 城下幸仁−2019.1.29)。
Tチューブ利用(T-tube)
城下幸仁, 飯野亮太. シリコンTチューブ留置にて管理した猫の気管狭窄の1例. 動物臨床医学 2019;28:025-029.
(抄録)猫の気管狭窄は概して予後不良である。11歳の雌の雑種猫が持続性喘鳴を伴う気管狭窄の精査加療のため当院呼吸器科に来院した。喉頭気管鏡検査にて頸部気管内に全周性粘膜肥厚を認め、生検とブラッシング後、気管狭窄部に切開を施しシリコンTチューブを挿入した。ただちに喘鳴は改善した。生検標本の鏡検にて慢性炎症性肥厚と判明した。Tチューブ抜管まで4ヵ月間、この猫は内科療法併用にて管理し無症状に過ごした。さらに抜管後480日間、呼吸症状なく生存した。
コメント:猫の気管狭窄にTチューブ設置して治療した初めての症例報告(犬・猫の呼吸器科 城下幸仁-2019.11.27)
Edens ET, Venker-van Haagen AJ. Experiences with the silicone T-tube in man and dog. Vet Q 1986;8:334-338. (PDFあり)
人と犬でのシリコンTチューブの使用経験
Silicone T-tubes are particularly useful for long-term stenting of the laryngotracheal airway. Silicone is useful when non-autogenous non-reactive soft material is wanted for use in the human and animal body. Two case reports illustrate the use of the silicone T-tube.
コメント:耳鼻咽喉頭科医と臨床獣医の共著によるTチューブ利用の症例報告。PubMed検索にて動物のTチューブ適用した唯一の報告。人の症例は気管食道ろうの外科整復術後の狭窄の症例で、1年半留置して抜管できた。犬の症例は交通事故による気管外傷に気管切開を実施し皮下気腫や術部汚染が遷延化し、外科整復非適応と判断され、Tチューブでの気道確保を実施した。6週間留置し気管壁の修復に成功し抜去可能となった。抜管後2週経過した時点で喉頭気管鏡検査を実施したが、ほぼ正常に復していた(犬・猫の呼吸器科 城下幸仁-2019.3.7)。